New research confirms that schizophrenia’s cognitive symptoms are correlated with lower synaptic density in certain parts of the brain.
Researchers have hypothesized that there is a link between schizophrenia and malfunctioning synapses since the early 1980s but lacked proper tools needed to investigate this in living brains. However, it was confirmed in post-mortem brain samples and animal cells in the lab.
But there’s no better proof of something than seeing it in action. New research at the Medical Research Council (MRC) London Institute of Medical Sciences did just that by using advanced brain-imaging techniques to peer into the synapses of living schizophrenia patients.
Instant synapses, just add protein
“Our current treatments for schizophrenia only target one aspect of the disease—the psychotic symptoms—but the debilitating cognitive symptoms, such as loss of abilities to plan and remember, often cause much more long-term disability and there’s no treatment for them at the moment. Synaptic loss is thought to underlie these symptoms,” says Professor Oliver Howes from the MRC London Institute of Medical Sciences, Imperial College London and King’s College London, the paper’s lead author.
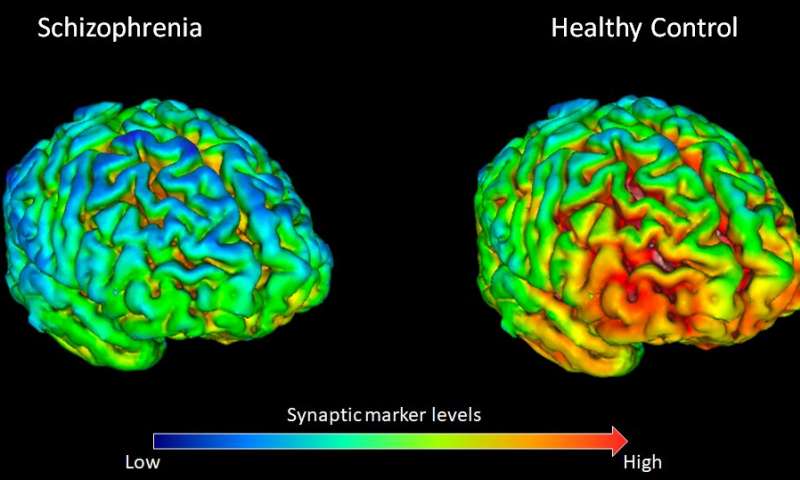
For the study, the team enlisted the help of 18 adults with schizophrenia and 18 people without (these were the controls). The research was made possible by a tracer molecule that emits a signal that can be picked up by a PET (positron emission tomography) brain scan. This tracer is injected into the bloodstream of a subject and binds to SV2A, a specific protein found in brain synapses. Animal and post-mortem human studies have shown that SV2A is a reliable marker for synaptic density in the brain.
The team reports that patients with schizophrenia showed lower levels of SV2A in the frontal and anterior cingulate cortices of the brain, which are involved in planning and other high-level functions. In essence, the lower levels of SV2A proteins seen here suggest a lower number of synapses (and thus, brain functionality) in the area.
“Our lab at the MRC London Institute of Medical Sciences is one of the few places in the world with this new tracer, which means we’ve been able for the first time to show there are lower levels of a synaptic protein in people with schizophrenia,” Professor Howes adds.
“This suggests that loss of synapses could underlie the development of schizophrenia.”
The schizophrenia patients that participated in this study had all received antipsychotic medication, which could affect the results. To address this, the team gave haloperidol and olanzapine, two antipsychotic drugs, to lab rats for 28 days, then analyzed their brains using the same method. Such medication had no effect on SV2A protein levels, they found, which helped to validate their results. This step also indicated that the antipsychotic medication currently in use doesn’t lead to a loss of synaptic density or function, which is always nice to know.
Therapeutic options for schizophrenia remain few and far between. The condition is a highly debilitating one, and any effective avenue of treatment would dramatically improve the quality of life for patients. Studies such as this one serve as a launching pad for developing future treatments, according to Dr. Ellis Onwordi from the MRC London Institute of Medical Sciences, lead author of the paper. The findings can also help guide brain research into other similar conditions by showcasing “how the extraordinarily complex wiring of the human brain is altered by this disease.”
“Having scans that can characterise the distribution of the approximately 100 trillion synapses in the living brain, and find differences in their distribution between people with and without schizophrenia, represents a significant advance in our ability to study schizophrenia,” he adds.
“We need to develop new treatments for schizophrenia. This protein SV2A could be a target for new treatments to restore synaptic function.”
In the future, the team hopes to scan the brains of younger people during the early stages of schizophrenia, to better understand how it develops in the brain. Do all the changes seen in this study happen suddenly, or do they develop over time as the condition progresses? Such data could help us better treat the condition, and maybe even stop it altogether.
The paper “Synaptic density marker SV2A is reduced in schizophrenia patients and unaffected by antipsychotics in rats” has been published in the journal Nature Communications.





