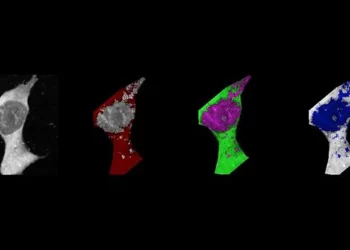
New research shows how different human cells respond to rhinovirus, the vector of the common cold. The results could help explain why some people are more susceptible to the disease than others.

Common colds, asthma attacks, and a host of other diseases associated with the respiratory tract share a common cause — rhinoviruses. However, not all people are made the same: some are more resistant to the pathogen, while others collapse into bed at the merest whiff of it.
In a bid to understand why, one team from the Yale University studied how key human cells respond to the pathogen.
Where’s the chicken soup?
To get to the bottom of things, the team worked with epithelial cells harvested from the nasal passages or lungs of healthy human donors. The team exposed both types of epithelial cells — kept in cultures under the same environmental conditions — to the virus.
Epithelial cells are a specialized type of cell that creates membranes and linings throughout the body. They’re usually the first bits to come into contact with pathogens, and, as such, possess traits that help them fight off bacteria and viruses. Rhinoviruses also have to contend with these cells when trying to infiltrate the body. Upon exposure to the bugs, epithelial cells lining our airways react to the threat, usually clearing it out of our systems before it gets a foothold and triggers symptoms. In some cases, however, this mechanism doesn’t seem to work: exposed to rhinoviruses, they fall mildly, or even seriously, ill.
The team reports that under business-as-usual scenarios, nasal cells have the more robust antiviral reaction among the two samples of cells. Further lab tests involved activation of the RIG-I pathway — a pattern-recognition network that the body uses to identify pathogens — in both types of sample cells so the team could see how each operated under emergency scenarios.
Upon activation of the RIG-I network, both cell types produced antiviral responses and beefed up their defenses against oxidative stress. Viral activity usually puts oxidative stress, a kind of chemical damage, on the cells they attack — so such a reaction should help them weather the invasion. Nasal cells showed the strongest antiviral response, while bronchial (deeper respiratory system) cells exhibited the strongest oxidative resistance of the lot.
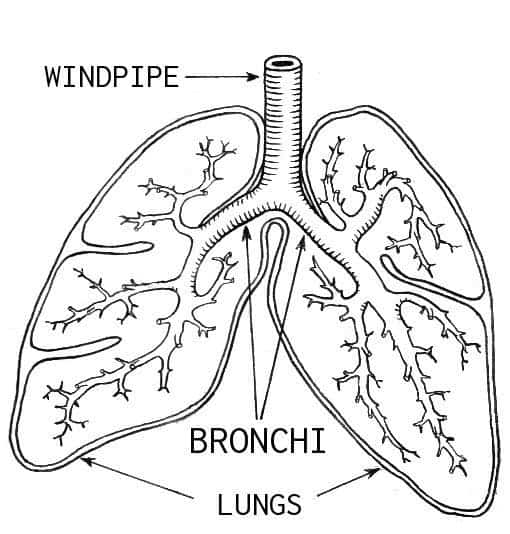
Excellence comes at a cost, however: the team also found that cells can act against oxidative stress or viruses, but not both at the same time. This was particularly interesting as inhaled irritants — for example cigarette smoke or tree pollen — also generate oxidative stress on cells, the team explains.
Nasal cells exposed first to cigarette smoke and then to rhinoviruses were more vulnerable to the virus’ effects, the team reports.
“Your airway lining protects against viruses but also other harmful substances that enter airways. The airway does pretty well if it encounters one stressor at a time. But when there are two different stressors, there’s a tradeoff,” says lead researcher Ellen Foxman.
“What we found is that when your airway is trying to deal with another stress type, it can adapt but the cost is susceptibility to rhinovirus infection. [The cells] survive the cigarette smoke but can’t fight the virus as well. And the virus grows better.”
Foxman says their study underscores a mechanistic link between environmental exposure and our body’s ability to resist the common cold. The findings also help explain why smokers tend to be more susceptible to rhinovirus infections.
The team hopes their efforts will lead to the discovery of new strategies to combat respiratory viruses, which cause an estimated 500 million colds and 2 million hospitalizations in the United States per year.
The paper has been published in the journal Cell Reports.