Modern technology is impressive, extremely useful, and sometimes a bit disturbing. Thanks to a new development, parents might soon be able to see their unborn babies developing in realistic 3-D immersive visualizations.
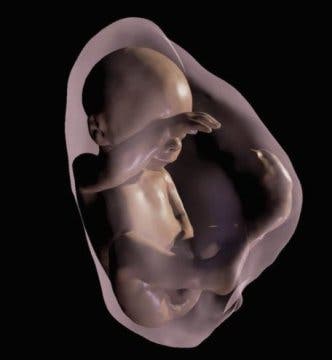
Credit: Image courtesy of Radiological Society of North America
Even if you’re not a parent you have to admit this is pretty cool. The new technology transforms MRI and ultrasound data into a 3-D virtual reality model of a fetus. Initially, sequential MRI slices are used as a scaffold for the model, and then the entire fetus baby is reconstructed in 3D. The accurate model includes the womb, umbilical cord, placenta and fetus, and researchers argue that the technology could even be used for educational purposes – not just for eager parents.
“The 3-D fetal models combined with virtual reality immersive technologies may improve our understanding of fetal anatomical characteristics and can be used for educational purposes and as a method for parents to visualize their unborn baby,” said study co-author Heron Werner Jr., M.D., Ph.D., from the Clínica de Diagnóstico por Imagem, in Rio de Janeiro, Brazil.
They key is the virtual reality which makes the visualization so spectacular. Dr. Werner and colleagues used the latest-generation Oculus Rift 2 headset. Oculus Rift is a virtual reality headset developed and manufactured by Oculus released earlier this year, one of the best virtual reality technologies available at the moment.
“The experience with the Oculus Rift has been wonderful,” Dr. Werner said. “It provides fetal images that are sharper and clearer than ultrasound and MR images viewed on a traditional display.”
But this is more than just a cool visualization technique, it could actually save lives. A big advantage is that it offers an assessment tool for fetal airway patency. Fetal airway patency is basically the way through which the unborn baby’s airways open and close, and this technology could highlight dangerous abnormalities. Researchers already report that the technology has proven useful in one case, where a baby suffered from an abnormality that required postnatal surgery. They hope to use this approach more broadly over the next year.
“The physicians can have access to an immersive experience on the clinical case that they are working on, having the whole internal structure of the fetus in 3-D in order to better visualize and share the morphological information,” Dr. Werner said. “We believe that these images will help facilitate a multidisciplinary discussion about some pathologies in addition to bringing a new experience for parents when following the development of their unborn child.”






