University of Utah researchers have identified a compound that could offer an alternative to opioids. Sourced from the venom of a small marine snail Conus regius, it blocks pain by targeting a non-opioid pathway in the brain.

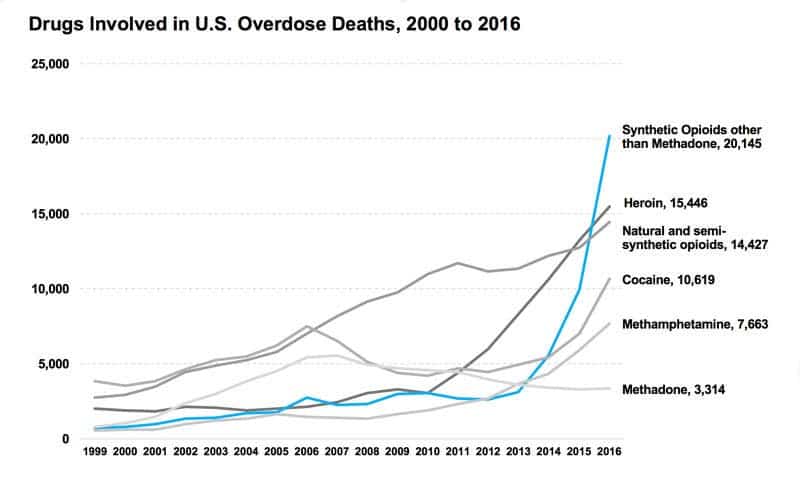
Opioids are very good at blocking pain, making them invaluable for medical applications. But they’re also very good at being addictive, which is a big problem. The CDC reports that some 91 people die from opioid overdose every day in the US alone and they always come back for more.
An alternative to opioids
So an alternative painkiller, one that doesn’t rely on the same brain structures as opioids but has the same punch, is needed. An alternative that the Conus regius, a small cone snail native to the Caribbean Sea, is poised to offer — this predatory critter’s venom, used to paralyze and kill prey, shows promise as a powerful painkiller.
“Nature has evolved molecules that are extremely sophisticated and can have unexpected applications,” begins Baldomera Olivera, Ph.D., professor in biology at the University of Utah.
“We were interested in using venoms to understand different pathways in the nervous system.”
The paper describes a compound isolated from the snail’s venom, called RglA, which acts through a different pathway than that targeted by opioid drugs. Rat studies have shown that its analog RglA4 can block α9α10 nicotinic acetylcholine pain receptors, effectively shutting down this pain pathway. Not only that, but the effect lasts for a long time, even after the substance has been cleared from the rat’s system (which took about 4 hours.) This would suggest that RglA4 has effects that go beyond numbing the sensation of pain — such as a regenerative effect on the nervous system.
“We found that the compound was still working 72 hours after the injection, still preventing pain,” said J. Michael McIntosh, M.D., professor of psychiatry at the University of Utah Health Sciences.
“What is particularly exciting about these results is the aspect of prevention,” he added. “Once chronic pain has developed, it is difficult to treat. This compound offers a potential new pathway to prevent pain from developing in the first place and offer a new therapy to patients who have run out of options.”
Rodent trials
To check if the substance would work on humans, the team took RglA and created 20 analogs of the compound. In essence, they took the bit that fits into the receptors, and put together slightly different configurations of it to see which one worked best. The analog RgIA4 was the one who bound the strongest to the human receptors.
To see how effective it would be as a painkiller, the team administered RglA4 to rodents who had previously been treated with a chemotherapy drug that induces extreme cold sensitivity and touch hypersensitivity. The team also set up two control groups — one which group was treated but didn’t receive RglA4, and one who was genetically modified to lack α9α10 receptors.
“Interactions that are not normally painful, like sheets rubbing against the body or pants against the leg, becomes painful,” said McIntosh.
The rodents who received RglA4 and the genetically altered control group didn’t show any signs of pain, but the other control group did.
“RgIA4 works by an entirely new pathway, which opens the door for new opportunities to treat pain,” McIntosh added.
“We feel that drugs that work by this pathway may reduce burden of opioid use.”
The full paper “Inhibition of α9α10 nicotinic acetylcholine receptors prevents chemotherapy-induced neuropathic pain” has been published online in the journal PNAS.