ZME Science has reported extensively on how 3-D printing is being implemented in the medical sector with some fantastic results. Yet, the real revolutionary thing about 3D printing – whether used for product prototyping, printing prostheses or spare parts on the International Space Station – is that anyone can use it.
Such is the story of Michael Balzer who made a 3D model of his wive’s skull, who was diagnosed with a life-threatening tumor, printed it, then sent it to renowned surgeons all over the country. Eventually, a doctor used the skull to prepare for a delicate, novel operation and removed the woman’s tumor with minimal invasion, as opposed to other methods. Had it not been for Balzer’s creative thinking, his wife would’ve likely gone blind in one eye, if not lost her life.
Eventually, a doctor used the skull to prepare for a delicate, novel operation and removed the woman’s tumor with minimal invasion, as opposed to other methods. Had it not been for Balzer’s creative thinking, his wife would’ve likely gone blind in one eye, if not lost her life.
Medicine in the hands of common people

Balzer and his wife, Pamela Shavaun Scott, are no strangers to health problems. Balzer, a former Air Force technical instructor and software engineer, lost his job after struggling with a long illness and Scott had her thyroid removed only a couple months prior to discovering the tumor.
It was the thyroid surgery that taught the couple how to approach their hardest moment together. Typically, the thyroid is removed by making a big cut in the throat which leaves a big and unaesthetic scar, followed by a long period of recovery. With proper diligence and research, the couple found doctors who used a novel procedure. They traveled from California to the Center for Robotic Head and Neck Surgery at the University of Pittsburgh Medical Center where a robotic arm carefully made minimal amounts of sharp cuts, otherwise impossible to make by a shaky human hand. This taught them the value of making use of the latest, cutting-edge technology out there and not going for the very first recommendation.
Yet, only a couple of months after the surgery Scott reported dreadful headaches. Fearing complications following the thyroid surgery, Balzer urged his wife to have an MRI scan- – she submitted. Disaster. Doctors found a three-centimeter tumor lodged behind her left eye. The two were heart struck, but the doctors who made the consultation didn’t share their worry. They reported that such tumors were common among women and recommended Scott should have it checked again in a year. Balzer wasn’t convinced, and sought a second opinion – quite a few actually. He e-mailed the MRI scans to doctors around the country, who almost unanimously agreed the women should immediately schedule for surgery.
A few months later, Scott had another MRI. This time, the doctors’ reaction was different: they were appalled by what seemed an accelerated tumor growth, indicating a far more severe condition than initially diagnosed. However, when Balzer — a seasoned 3D designer — rendered his wive’s DICOM files (the standard digital format for medical imaging data) atop previous MRIs, he found that the tumor hadn’t grown. The radiologist was just looking at it from another angle and it appeared bigger.
“I thought, ‘why don’t we take it to the next level?’” Balzer says for Makerzine. “Let’s see what kind of tools are available so that I can take the DICOMs, which are 2D slices, and convert them into a 3D model.”
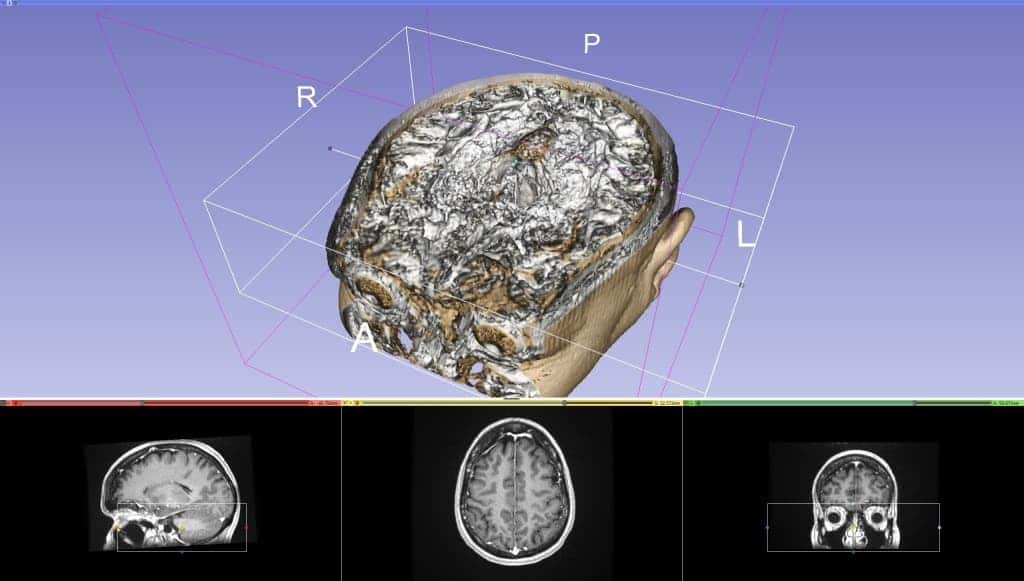
He then took the model and printed it to have a better idea of kind of treatment they could seek. Scott’s tumor, known as meningioma, sits somewhere beneath the brain. So to reach it and remove it, doctors have to saw the skull, literally uproot the brain, reach out under it and eject the tumor. Yes, it’s as bad as it sounds.
Following such an operation, Scott would have stood at a considerable risk of losing her smell, taste or even sight, since nerves can easily become loose.
Desperate, Blazer send the 3D model to doctors across the country, looking for some alternative treatment. He was in luck, he found a surgeon in the same Pittsburgh research center where Scott had her thyroid removed. A neurosurgeon there agreed to consider a minimally invasive operation in which he would access the tumor through Scott’s left eyelid and remove it using a micro drill.
Blazer sent the doctor a few full-sized models of his wife’s skull, which the team there used it to practice and plan the procedure. Scott had the tumor removed at UPMC in May 2014 through a small opening above her left eye. Doctors noticed that the tumor had begun to entangle her optical nerve and had she waited more than six months for the surgery, she most certainly would have gone blind. Following the eight-hour long procedure, 95% of the tumor was extracted and no visible marks were left visible. It was a sound victory – one that goes beyond the husband and wife’s life story.
Blazer’s creative thinking was made famous in medical circles throughout the country. Unwittingly, he layered the groundwork for the Medical Innovation Lab in Austin, Texas — a lab that will use 3D printed models to help plan procedures and to explain diagnoses to patients.
“What you can now do through 3D printing is like what you’re able to do in the software world: Rapid iteration, fail fast, get something to market quickly,” says Dr. Michael Patton, CEO of the Lab, which launched in October 2014 . “You can print the prototypes, and then you can print out model organs on which to test the products. You can potentially obviate the need for some animal studies, and you can do this proof of concept before extensive patient trials are conducted.”
Here’s how to print your own medical features, be it a skull, bone or even organs if you’ve had an MRI or CT scan.
- Ask your doctor for the DICOM files
- Download 3D slicer and use the Region Growing tool to segment the image
- Extract the 3D mesh of the surface and save as STL
- Use ParaView to simplify the mesh
- Print .






