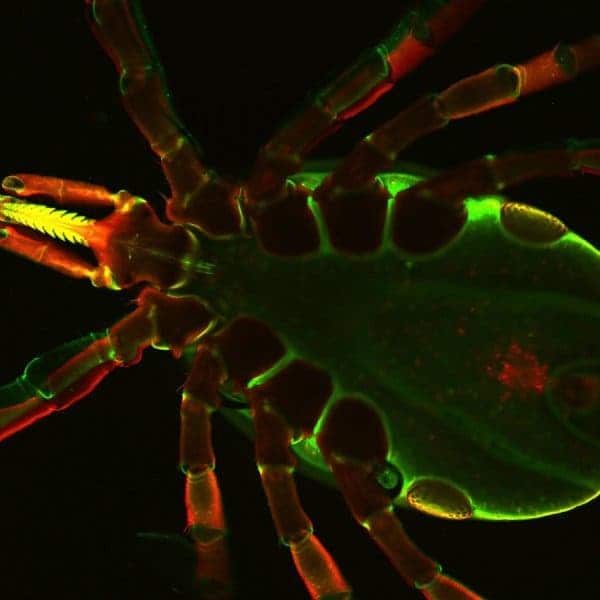
Lyme disease is the most common vector-borne disease in the United States, affecting more than 300.000 people per year. It’s caused by the bacteria Borrelia burgdorferi, which is transmitted to humans through the bite of infected black-legged ticks.

The most common treatment for the disease is oral antibiotics, typically doxycycline, used in the early stages of Lime. Nevertheless, for reasons still unclear, the antibiotics don’t work for up to 20% of the people with the disease, which has led researchers to look at alternative approaches.
“Some researchers think this may be due to drug-tolerant bacteria living in the body and continuing to cause disease,” Jayakumar Rajadas, director of the Biomaterials and Advanced Drug Delivery Laboratory at the Stanford School of Medicine. “Others believe it’s an immune disorder caused by bacteria during the first exposure.”
Rajadas and a group of researchers from Stanford and Loyola College decided to investigate whether two different antibiotic drugs, cefotaxime and azlocillin, could prove more effective at killing the bacteria in the early stages of the disease than the currently prescribed antibiotic doxycycline.
The team first tested to see whether different doses of the drugs could kill drug-tolerant borrelia bacteria grown on laboratory plates better than a standard Lyme disease antibiotic. They did these three times in triplicate and at different ages of the bacteria.
The results were highly positive. At high concentrations, both drugs could kill the bacteria cells and outperformed the standard Lyme disease antibiotic. When the study team tested the drugs at lower doses, azlocillin outperformed the standard antibiotic and cefotaxime.
The next step was testing the two new drugs in a small number of laboratory-bred mice that they infected with the bacteria. They treated the mice at different stages of the disease and gave them a daily dose of either azlocillin, cefotaxime, or the standard treatment for Lyme disease for 5 days.
The researchers found that both the standard treatment and azlocillin completely cleared the infection in the early stages of the disease, while cefotaxime did not. After three weeks, they couldn’t find any bacteria in the mice that had been given azlocillin, while the ones that had been given the standard treatment still had it.
Now, the team plans to test azlocillin in a clinical trial on humans. Although these preliminary results are promising, this was a small study carried out in laboratory-grown mice, so researchers may not see similar results in humans. However, as the Food and Drug Administration (FDA) has already approved azlocillin.
“We have been screening potential drugs for 6 years,” Venkata Raveendra Pothineni, Ph.D, said. “We’ve screened almost 8,000 chemical compounds. We have tested 50 molecules in the dish. Our main goal is to find the best compound for treating patients and stop this disease.”
The study was published in Nature.