New research at the University of Maryland (UMD) has uncovered how bacteria that cause Lyme disease survive and persist for months following our body’s immune response.
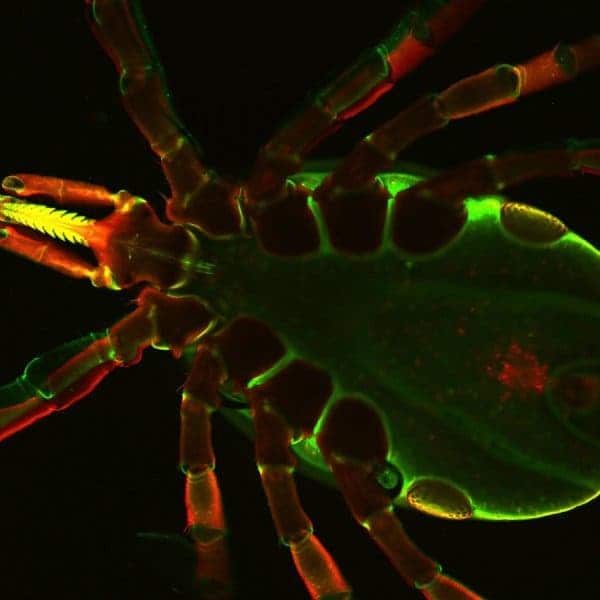
Image credits Dr. Utpal Pal / University of Maryland.
Throughout his 12 years of work at the UMD, Dr. Utpal Pal has gained a unique understanding of the works of Lyme disease and the bacteria that causes it (spirochete Borrelia burgdorferi). His previous research isolated the protein marker we use to identify when this spirochete infects the body. A new paper from his lab sheds light on one of this bacteria’s scariest and least understood abilities, by describing a protein it produces that disables our bodies initial immune responses. The new study also explains how this bacteria can re-appear in the body weeks after treatment.
When life gives you limes
Borrelia burgdorferi is one of the few pathogens that can persist in the body for long periods of time. In light of this fact, there has been keen interest from the medical community in understanding why and how it does it. Such knowledge would be a major breakthrough for the treatment of tick-borne diseases like Lyme, which is becoming an increasingly prevalent public health issue.
“Most people don’t realize that they actually are walking around with more bacterial cells in their bodies than their own cells, so we are really bags of bacteria,” Pal says. “Most are good, but the second your body detects something that is a pathogen and can cause disease, your immune system starts to work.”
According to Pal, Lyme disease isn’t actually caused by the bacteria, but by your body’s reaction to it. When the infection is first detected, our immune system has to work on incomplete information: it knows something is trying to invade, but not exactly what. So, it sends a versatile, nonspecific wave of attack in a bid to fight off the pathogens before they set up camp. This stage usually takes a few hours to a few days at most.
If unsuccessful, our immune system gets readied for a prolonged conflict. It takes between seven to ten days to gather data on the enemy, finally sending a second, more numerous and highly specialized wave of reinforcement to wipe the floor with whatever pathogens are still alive and kicking.
In the case of Lyme disease, however, this dance doesn’t go according to our body’s schedule. Sometime between six months to a year after traditional antibiotic therapy, many people experience returning, non-objective symptoms of varying intensity for which there is no currently-known treatment (but plenty of bogus ones) — a condition known as Post-Treatment Lyme Disease Syndrome.
Dr. Pal and colleagues found that even in the absence of the protein used to defeat the first attack from our immune systems, the infection can reoccur a few weeks later. This suggests Borrelia, just like our immune system, uses a layered defense strategy, something that has never been observed before — and which could explain what causes chronic cases of Lyme disease.
“[Borrelia burgdorferi] wins the first battle, and your body overreacts so much that it causes intense inflammation in all the joints and areas that the bacteria spreads by sending so many reinforcements to kill it. Borrelia is then killed, but the inflammation remains and causes many of your symptoms for Lyme disease,” Pal explains.
“That is why killing Borrelia in the first wave of immunity is so important.”
According to estimates from the Centers for Disease Control and Prevention (CDC), there are about 300,000 new cases of Lyme disease in the US each year. However, these cases are largely underestimated and reported due to the attention given to mosquito-transmitted diseases like malaria. Pal says that ticks are actually a greater public health concern than people realize: he says “the majority” of vector-borne diseases in the US can be traced back to ticks, with 6 out of the 15 distinct tick diseases (including Lyme) transmitted by the Ixodes tick.
The paper “Plasticity in early immune evasion strategies of a bacterial pathogen” has been published in the journal Proceedings of the National Academy of Sciences.