Throughout the world, the need for donating blood has never been greater. Almost anywhere you look, hospitals are in need of donor blood — but at the same time, the donorship system needs to ensure the lack of harmful viral particles such as hepatitis and HIV.
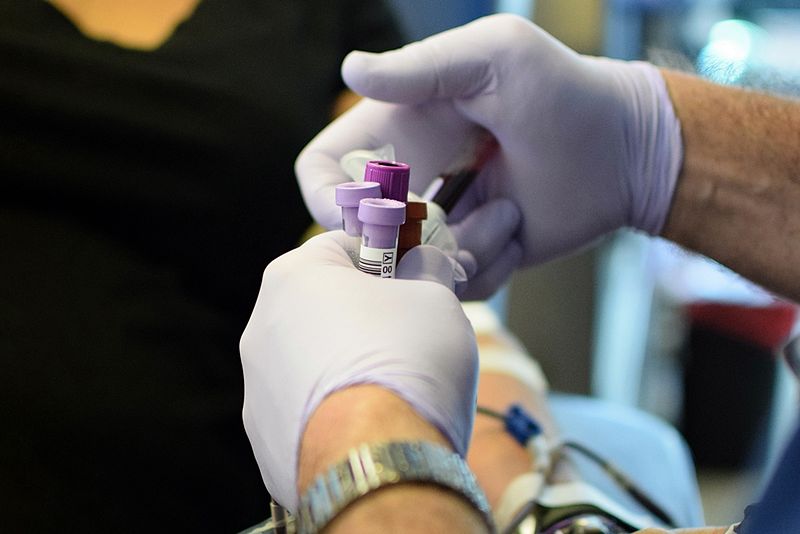
According to recent stats by the WHO, some areas feature an alarming situation: a violation of the research protocol and blood analysis was reported in 35 countries, from the very stage of collection of donated blood. Not all donated blood is always examined for the presence of harmful infections; in some countries where testing is carried out, the proper quality of research is not ensured, WHO officials note.
It seems hard to imagine, but 43% of hospitals performing transfusions don’t even have systems for reporting adverse transfusion events — and when you consider the lack of irregular aces to medical consumables and equipment and the lack of trained personnel, the scale of the crisis becomes apparent. There is a marked difference between low- and high-income countries, the WHO notes.
To ensure the safety of transfused blood, antiviral detection is crucial. However, the diagnostic methods used by modern medicine for detection of viruses are not always accurate; sometimes the results of testing for the presence of viruses and determining their viability, for example, in donated blood, happen to be unreliable. Several factors can be responsible for this lack of detection:
- imperfection of the methods causing mistakes in the research results;
- inability of these methods to recognize viruses at low titers of viral load;
- inability of methods to determine the harmfulness of viruses, that is, to determine their viability;
- violation of the requirements when the research is conducted, including the violation of procedre, human error, etc.
Viruses possess lymphotropic properties, that is, the ability to penetrate and persist in the lymphocytes of a healthy person. Based on scientific and practical works and research carried out by New Medical Technologies, and with the assistance of the scientists from the Institute of Epidemiology and Microbiology of Uzbekistan (UzNIIEMIZ), modern innovative methods have been developed. This approach can be used for detecting viruses and determining their viability, as well as a method for inactivating RNA and DNA containing viruses (COVID-19 is also RNA containing virus). These include Hepatitis B, C and HIV viruses, influenza virus, hemorrhagic fever (Ebola group) possessing lymphotropic properties, and also inactivation method, that is, neutralization of bacteria, endospores and fungi.
Ovik Mkrtchyan, founder of New Medical Technologies company, explains:
“While testing our research method at Republican Center for Blood Transfusion in Uzbekistan, we found that 18% of samples taken with the use of traditional research methods that is, immunoenzyme method and polymerase chain reaction method, contained viral particles. The conclusion is that old methods are not effective enough, and the risk of transmission of dangerous diseases from donor to patient is real.”

The method for detecting viruses in lymphocytes of donated blood has been in development for several years and has become the first completed research in this area. Although similar research work was conducted earlier, for example, by Japanese scientists, unfortunately, it did not result in the creation of a well-defined technology.
“We were the first who developed a correct algorithm for conducting research of donated blood; as a result we have created a new method for determining viable viruses possessing lymphotropism properties,” Ovik Mkrtchyan said.
New Medical Technologies company has developed and patented several methods, including: “Method for excluding false negative results when testing donated blood for infection with hepatitis viruses HBV and HCV, and HIV CC”, “Method for assessing the viability of lymphotropic viruses” and “Method for detecting lymphotropic viruses in biological matrix when the level of virus concentration is below the sensitivity threshold of the polymerase chain reaction method.”
“These inventions are a breakthrough and a confident step in ensuring safety of the donorship system, including recipients’ safety. The method which we have developed for detecting and assessing the viability of lymphotropic viruses, has no analogues,” adds Mkrtchyan.
The advantage of these innovative methods is that there is no need to purchase new equipment in order to use them in practice — the equipment used in every diagnostic PCR laboratory is quite enough. The methods are simple, and assistants of PCR laboratories, after having read the instructions for conducting research and analyzing the results, can easily use the developed methods in practice without special long-time training and face-to-face consultations.
Another area of application of innovative methods developed by New Medical Technologies is the disinfection of medical instruments, other items and surfaces. Mkrtchyan continues:
“There is a certain number of medical instruments which can not be treated with the use of high temperatures and strong chemicals. Such instruments are used in dentistry, surgery, gynecology and cosmetology. As a result, there is a risk of infectiing the patient with blood-borne infections, RNA and DNA containing viruses (it should be noted here that COVID-19 is an RNA containing virus), bacteria, spores and fungi.”
To solve this problem, New Medical Technologies company has created a special installation that applies a photodynamic disinfection method using methylene blue as a photosensitizer (sterilizing agent). The photodynamic method has been used for a long time in medicine for the treatment of diseases in dentistry, oncology, gynecology, urology, ophthalmology, diseases of the respiratory tract and throat, for the treatment of skin diseases, in cosmetology, as well as in the diagnosis of various diseases. Patents for this method have been issued by the USA, Eurasia, China and Uzbekistan, but the photodynamic method is widely used in countries such as the US, Germany, and France.
When methylene blue is photoactivated, singlet oxygen is formed in the solution. A large number of oxygen radicals inactivate RNA and DNA molecules of viruses by cleaving nucleic acids from them and attaching methylene blue molecules in their place. This method does not have disadvantages of other sterilization methods: steam or air sterilization with 100% ethylene oxide, hydrogen peroxide vapor sterilization or formaldehyde vapor sterilization.
The sterilizing equipment developed by the company has no direct analogues and has been highly appreciated by respected professionals and departments engaged in this field; it is recommended for use in medicine and the service sector.
Virus inactivation takes about 60-90 minutes, and for the convenience of medical institutions, we offer installations operating in both automatic and semi-automatic modes, with working chambers of different sizes, from desktop to large ones, allowing you to load a large number of instruments. Sterilizing installations produced by New Medical Technologies company are absolutely safe for staff and the environment; they are not toxic and don’t cause allergies.
Professor Nariman Gulyamov, Dr. habil. in Medicine, is convinced that spread of viral diseases is a global problem.
“Chronic viral diseases are difficult to cure therefore their prevention is extremely important. Any procedures involving skin penetration bear a risk, therefore sterilization of medical instruments ranks foremost. Products developed by New Medical Technologies company make it possible to solve this problem in a reliable and safe manner. The next stage on the way of implementing the developed methods is carrying out large-scale research with the participation of foreign colleagues in the leading research laboratories of the world (Europe and the United States, etc).” Professor N.G. Gulyamov noted.







