In a study published Monday in the journal Scientific Reports, researchers from the University of Queensland caution that the surge in scarlet fever cases may pose an unexpected threat.
Evolution is a wonderful thing — it brought us out of the primordial puddle and took us to the Moon, and will hopefully power us to even greater heights. It’s an awesome thing, and I’m a big fan of it. But evolution does tend to have one nasty habit — it never stops, not even for the bugs that are trying to kill us dead.
One of those bugs is group A Streptococcus; it’s the biological vector of scarlet fever, a condition that commonly affects children from 5 to 12. Most of those infected with this bacteria only develop strep throat, but in some cases it can escalate into a full-blown case of scarlet fever, thus named for the red, sandpaper-like rash it causes on the skin.
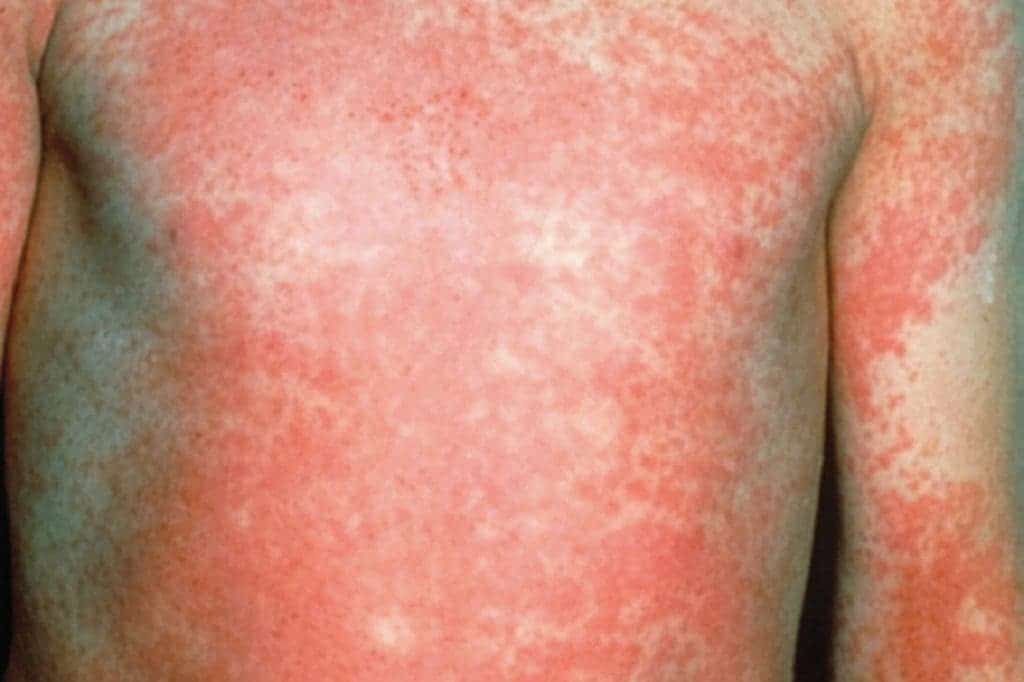
Image via newsshopper
It used to be a deadly disease, but with the advent of modern antibiotics it’s just unpleasant — while there is no vaccine for it, medication can easily treat the condition.
But if the Streptococcus is easily kept in check with antibiotics, why the sudden increase in number of scarlet fever cases in the recent years? The answer is evolution — more to the point, evolution of drug-resisting bacteria.
“We now have a situation which may change the nature of the disease and make it resistant to broad-spectrum treatments normally prescribed for respiratory tract infections, such as in scarlet fever,” lead study author Nouri Ben Zakour said in a statement.
Ben Zakour’s team analyzed samples from 25 confirmed scarlet fever patients and 9 patients suffering from a number of group A strep infections from China and Hong Kong. They were able to confirm that a strain of group A strep that emerged in the 1980s was the common cause for all of the infections.
The usual treatment, penicillin, still works on this strain — other common antibiotics do not. The team found evidence of tetracycline, erythromycin and clindamycin resistance, raising immediate concerns for the patients who are allergic to penicillin. However, we’re all at risk here. Should a strain develop that also has resistance to penicillin, there will be few treatment options left for doctors.
The increase of antibiotic resistant bacteria should come as no surprise. As such substances become more and more common in the environment as consequence of human and agricultural use, more and more bacteria are exposed to them. Any that survive will multiply, and when they infect a human host they’ll be immune to one or more antibiotic substances. Antibiotic resistance causes an estimated 2 million illnesses and 23,000 deaths every year in the United States.
The findings, Ben Zakour said, suggest that monitoring the spread and evolution of this bacteria is of the utmost importance. The fact that penicillin still seems to work in most cases of scarlet fever means that it isn’t time to panic. But this is just the latest example of the ticking time bomb that is antibiotic resistance.






