The fight against drug-resistant microbes just got a bit better. Chemical changes to a drug called Vancomycin make it 25,000 times more potent, much more likely to kill even the toughest pathogens.
Science strikes back
There’s more and more talk of a post-antibiotic world, as more and more pathogens are building up a resistance to antibiotics. Antibiotic resistance occurs when an antibiotic is no longer effective at controlling or killing bacterial growth. Bacteria which are ‘resistant’ can multiply in the presence of various therapeutic levels of an antibiotic and are increasingly dangerous as they continue to multiply and to pass their resistance to their offspring.
This has long been considered a distant problem but in recent years, it became obvious just how acute this issue is. Take gonorrhea, for instance, a relatively common disease which causes an estimated 33 to 106 million new cases each year. The disease used to be simple to treat, but that’s not often the case nowadays. In fact, many doctors believe that gonorrhea will soon become impossible to treat in the near future, and this is not an isolated disease. The World Health Organization has developed a list of 12 pathogens which can very well become immune to everything we can throw at them. But scientists are not sitting idle.
After developing the 2.0 version of an antibiotic called Vancomycin, US researchers have taken things even further and developed the 3.0 version — which is ungodly strong.
A last resort
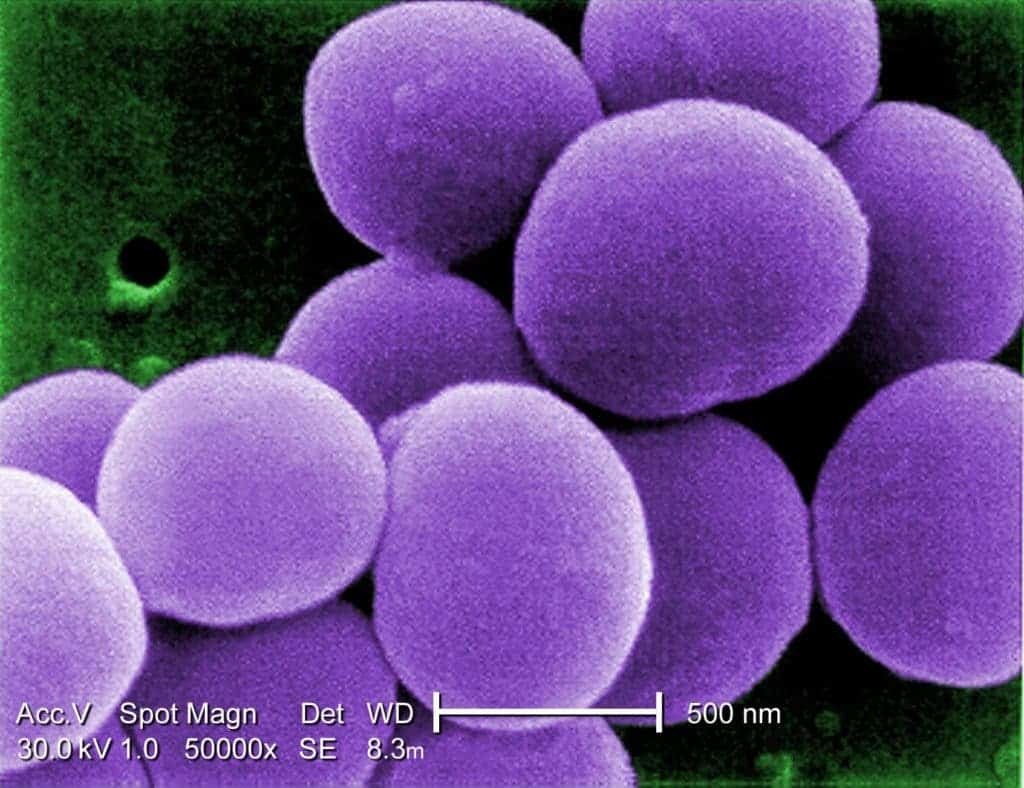
Vancomycin is an antibiotic used to treat a number of bacterial infections, usually administered intravenously. It’s often the first line of defense against complicated skin infections, bloodstream infections, bone and joint infections, as well as meningitis caused by Staphylococcus aureus (VRSA). But Vancomycin is also regarded as a last-resort drug.
It kills bacteria by preventing them from building cell walls, destroying wall-building protein fragments called peptides. But bacteria have adapted. They’ve replaced the peptides that the antibiotics try to target, to others which Vancomycin can’t bind to. In some cases, they’ve adapted so much that nothing can kill them, even the last-ditch Vancomycin.
According, to the U.S. Centers for Disease Control and Prevention, drug-resistant bacteria kills 23,000 people every year just in America. It’s not clear how many of these cases involve Vancomycin, but looking at things globally, improving this drug could save a lot of lives.
In order to make it stronger, researchers implemented all the improvements demonstrated by others groups. Dale Boger, a chemist at the Scripps Research Institute in San Diego, California, took everything and the kitchen sink and threw it into Vancomycin, in the hope that it would make it a more potent drug.
It worked. Using more weapons proved instrumental, as pathogens simply couldn’t adapt to everything.
“Organisms just can’t simultaneously work to find a way around three independent mechanisms of action,” he says. “Even if they found a solution to one of those, the organisms would still be killed by the other two.”
Boger also says that this demonstrates a new, improved way of coming up with antibiotics. Typically, there’s a lot of trial-and-error involved in antibiotic design, but doing things purposelly and planned, while extremely difficult, can also be very rewarding.
“As an alternative to championing the restricted use of antibiotics or conceding that bacteria will always outsmart us, can durable antibiotics be developed that are capable of continued or even more widespread use?” Then, maybe, drugs could “overcome the forces of evolution and selection responsible for bacterial resistance, that are less prone or even impervious to resistance development, that avoid many of the common mechanisms of resistance, and that are more durable than ever before.”
So far, the drug has only be tested in a lab environment. Researchers will now test the new drug on animals, and if everything goes fine with that, on humans. If its potential is confirmed, then humanity’s last line of defense against drug-resistant bacteria just got a lot stronger. But it’s still the last line of defense.
Journal Reference: Akinori Okano Nicholas A. Isley and Dale L. Boger — Peripheral modifications of [Ψ[CH2NH]Tpg4]vancomycin with added synergistic mechanisms of action provide durable and potent antibiotics. doi: 10.1073/pnas.1704125114
Was this helpful?