The WHO has published a list of priority drug-resistant pathogens which can threaten mankind. These bacteria have become so resistant to antibiotics that procedures such as organ transplantation, cesarean sections, joint replacements, and chemotherapy might simply be too risky to perform.
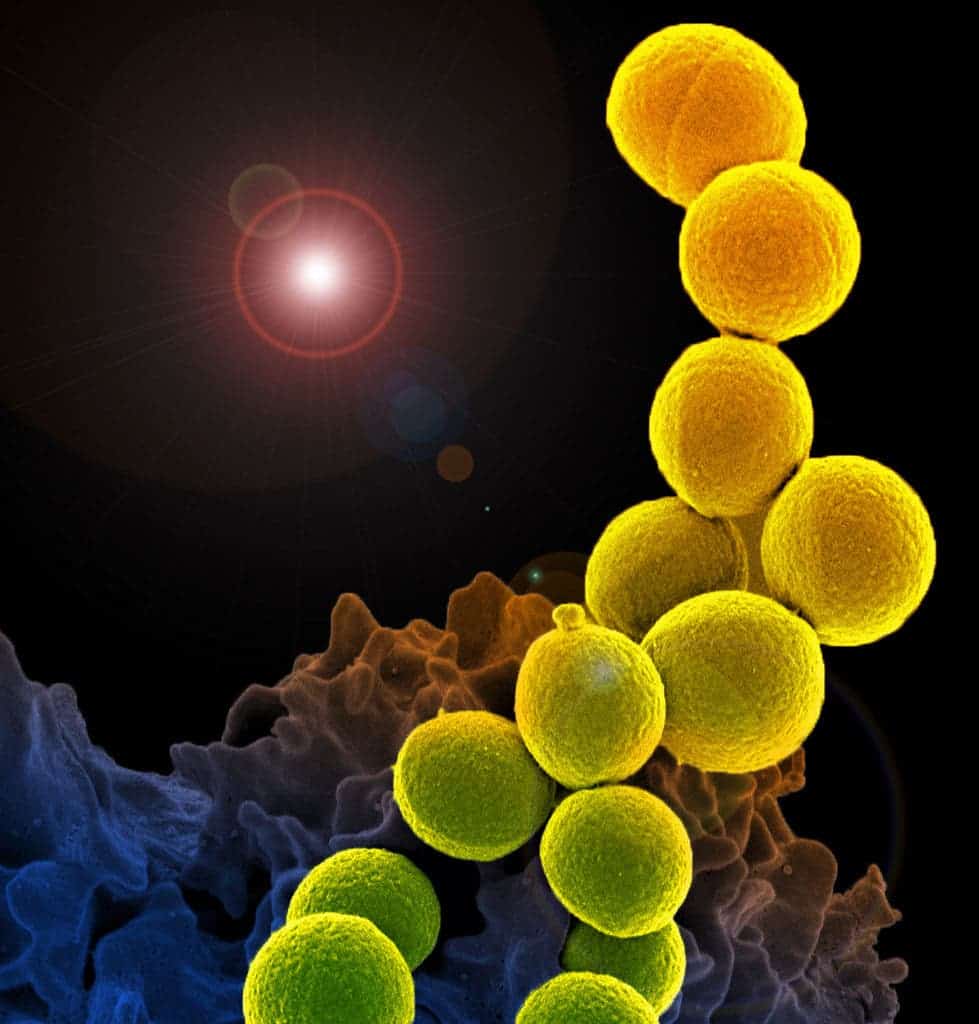
Colorized scanning electron micrograph of a white blood cell interacting with an antibiotic-resistant strain of Staphylococcus aureus bacteria. Credits: NIAID
Humans vs Bacteria
According to the WHO, the market is simply not doing enough to tackle this issue, and if we keep going with the ‘business-as-usual’ approach, then pretty soon we won’t have much in the way of dealing with these pathogens. Antibiotic resistance is developing at a faster rate than we’re implementing new treatments, scientists warn.
“This list is a new tool to ensure R&D responds to urgent public health needs,” says Dr Marie-Paule Kieny, WHO’s Assistant Director-General for Health Systems and Innovation. “Antibiotic resistance is growing, and we are fast running out of treatment options. If we leave it to market forces alone, the new antibiotics we most urgently need are not going to be developed in time.”
Drug-resistant bacteria are not really something new — doctors and researchers have been worried about them for a few good years already. UN Secretary-General Ban Ki-moon said that without a doubt, drug-resistant bacteria is becoming a fundamental threat to human development and security, and world leaders have pledged to address this issue — but they’re not really doing it fast enough. Some 700,000 people are killed by drug-resistant bacteria every year, but that’s nothing compared with what could come in the near future. Projections show that the figure might increase by more than 1000% until 2050, but even then it can get much worse.
“New antibiotics targeting this priority list of pathogens will help to reduce deaths due to resistant infections around the world,” says Prof Evelina Tacconelli, Head of the Division of Infectious Diseases at the University of Tübingen and a major contributor to the development of the list.
“Waiting any longer will cause further public health problems and dramatically impact on patient care.”
Basically, as bacteria evolve and become more and more well-equipped to deal with our treatments, our list of options grows shorter and shorter. Ultimately, we may simply have no way of treating some infections — and we’re seeing glimpses of that already. Since it takes a long time to develop new treatments (if that’s even possible), bacteria can take the upper hand and there’s little we will be able to do to stop them. That’s why the WHO is releasing this list: to underline the urgent need to think ahead and start working overtime towards developing alternative treatments. By “alternative treatments” I mean serious, science-backed treatments, not alternative medicine.
The list
The WHO split the 12 pathogens based on priority. Well, all of them pose risks and are high priority, but this is the priority ranking of the high priority. They didn’t include some very dangerous bacteria for which there are already specialized programs in place — such is the case of drug-resistant tuberculosis.
Other bacteria, such as streptococcus A and B and chlamydia, were not included because they have low levels of resistance to existing treatments and do not currently pose a significant public health threat. So in the WHO list…
Three bacteria are considered to be of critical priority:
- Pseudomonas aeruginosa, carbapenem-resistant
- Enterobacteriaceae, carbapenem-resistant, ESBL-producing
- Acinetobacter baumannii, carbapenem-resistant
Six are considered to be of high priority:
- Enterococcus faecium, vancomycin-resistant
- Staphylococcus aureus, methicillin-resistant, vancomycin-intermediate and resistant
- Helicobacter pylori, clarithromycin-resistant
- several species of Campylobacter, fluoroquinolone-resistant
- Salmonellae, fluoroquinolone-resistant
- Neisseria gonorrhoeae, cephalosporin-resistant, fluoroquinolone-resistant
Three are deemed to be of medium priority:
- Streptococcus pneumoniae, penicillin-non-susceptible
- Haemophilus influenzae, ampicillin-resistant
- • several species of Shigella, fluoroquinolone-resistant
Tim Jinks, head of drug resistant infections at the Wellcome Trust, commented on need for such a list:
“This priority pathogens list, developed with input from across our community, is important to steer research in the race against drug resistant infection – one of the greatest threats to modern health.
“Without effective drugs, doctors cannot treat patients. Within a generation, without new antibiotics, deaths from drug resistant infection could reach 10m a year. Without new medicines to treat deadly infection, lifesaving treatments like chemotherapy and organ transplant, and routine operations like caesareans and hip replacements will be potentially fatal.”
All of us
It should also be noted that a big part of this problem is us — all of us. To put it bluntly, we’re not careful enough when it comes to antibiotics. Too often we pop them like candy, and too often we don’t complete our treatment because “we’re feeling fine now”.
Taking antibiotics without a medic’s advice and not properly completing a treatment cause more trouble than you’d think. What you’re really doing is basically setting up a training camp for bacteria, helping them adapt and breed descendants more resistant to antibiotics.
At the end of the day, no matter how much effort is poured into discovering new treatments, that’s not going to solve things by itself. We also need to focus on prevention of infections and just as importantly, on the use of existing antibiotics.
Was this helpful?



