
The World Health Organization (WHO) has ranked vaccine hesitancy as one of the top 10 health threats in the world for 2019. Other threats flagged by the WHO were diabetes, cancer and heart disease, people living in vulnerable settings, antimicrobial resistance, Ebola, weak primary health care, dengue, and HIV.
The 🌍 is facing multiple health challenges.
10 health issues WHO will tackle in 2019:
1⃣Air pollution & Climate change
2⃣Noncommunicable diseases
3⃣Influenza
4⃣Vulnerable settings
5⃣Antimicrobial resistance
6⃣Ebola
7⃣Primary health care
8⃣Vaccines
9⃣Dengue
🔟HIV#HealthForAll pic.twitter.com/5Hh5sruuCo— World Health Organization (WHO) (@WHO) January 15, 2019
Vaccine hesitancy is sad and worrying because vaccination also plays a role in reducing antimicrobial resistance as well as reducing complications in patients with non-communicable diseases – two other global factors in WHO’s top 10 list of health threats. There are well-documented reports showing that some vaccines decrease antibiotic use, thus lowering the likelihood of antibiotic resistance. Studies also show that people with type 2 diabetes can significantly lower their risk of major cardiovascular events such as stroke and heart failure during the influenza season by getting the flu vaccine.
Vaccine hesitancy refers to delay in acceptance or refusal of vaccines despite availability of vaccination services. Dr. Bruce Y. Lee, perfectly explains what vaccine hesitancy is – “it is people questioning whether to get vaccinated or more often whether children should be vaccinated, despite the abundance of scientific evidence showing the effectiveness of vaccines in preventing disease, despite the lack of proven alternatives, and despite experts around the world urging people to get vaccinated.”
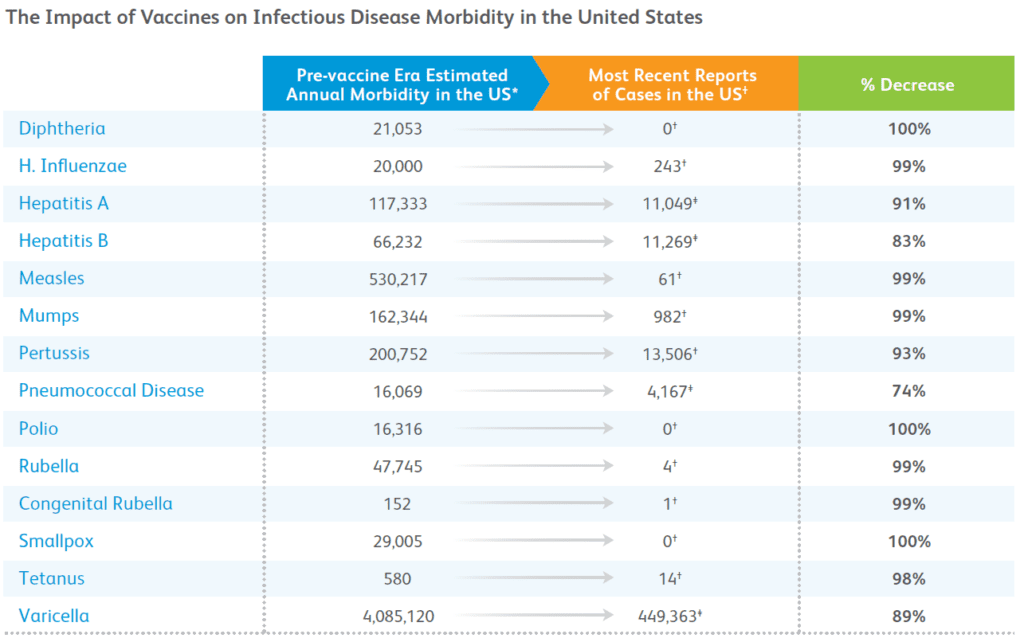
Vaccination is one of the most cost-effective ways of preventing disease – it currently prevents up to 3 million deaths a year from tuberculosis, diphtheria, tetanus, pertussis (whooping cough), polio, measles, hepatitis B, and Hib (Haemophilus influenzae b) infections. A further 1.5 million deaths could be avoided if global vaccine coverage rate improved. Vaccines have an indisputable track record – through vaccines, we have eradicated smallpox and contained polio to just three endemic countries and greatly reducing many other diseases
One of the biggest drivers of health behaviors is risk perceptions. Anti-vaccine information shapes this and science advocates need more effective responses. We need to highlight stories about the success of vaccines, educate people on how to appraise information (distinguish facts from fake news), have pro-active communication between parents and healthcare professionals, provide education materials on social media platforms).
#Vaccine advocates need to 1) highlight stories about success of #vaccines, 2) educate people on how to appraise information, 3) have pro-active communication between parents & #healthcare professionals, 4) provide education materials on social media platforms. #VaccinesWork pic.twitter.com/M5Z6Qmy44I
— Dr Melvin Sanicas (@Vaccinologist) January 21, 2019
There are several anonymous anti-vaccination messages on social media that have no clear sources other than blogs and dubious publications. A lot of these websites are still referencing Andrew Wakefield’s retracted and fraudulent paper published in The Lancet. Compare this with the real doctors and healthcare professionals and experienced scientists who are willing to clearly put their names and list their experience and qualifications on messages that support vaccination.






