
Since fever is one of the main symptoms of COVID-19, in many countries temperature checkups are required to enter public indoor premises such as a mall or airport. But these spot checks “are the equivalent of catching a syllable per minute in a conversation, rather than whole sentences,” said Benjamin Smarr, a professor of bioengineering at the University of California San Diego, who thought of a better alternative driven by many more data points.
In a new study, Smarr and colleagues have presented the findings of a trial involving 65,000 people who have worn the Oura smart ring. The wearable device developed by a Finnish startup (also Oura) records temperature, heart rate, respiratory rate, and levels of physical activity. Among the participants, 50 had COVD-19, and scientists say that these infections can be predicted from the ring’s data.
“With wearable devices that can measure temperature, we can begin to envision a public COVID early alert system,” Smarr said in a statement.
Unlike a random temperature spot check, the Oura ring gathers information around the clock, day and night, over long periods of time. This wealth of data allowed the researchers to notice that fever appeared before the participants were reporting symptoms, as well as among those that never reported symptoms. For 38 of the 50 participants, fever was identified when symptoms were unreported or even unnoticed.
Previously, some public health experts have suggested that some cases of fever, and consequently potentially of COVID-19, may go underreported or unnoticed, separate from truly asymptomatic cases. “Wearables, therefore, may contribute to identifying rates of asymptomatic [illness] as opposed to unreported illness, [which is] of special importance in the COVID-19 pandemic,” the authors noted in their study published in the journal Scientific Reports.
The researchers claim that the participants’ data had not been violated during the study’s timeframe. The data was stripped of personal information, including the location data, and each subject is known by a random ID number. The 50 participants had contracted COVID-19 before joining the study but had been wearing Oura rings during the time they fell ill. They provided symptom summaries and granted researchers full access to their rings’ data.
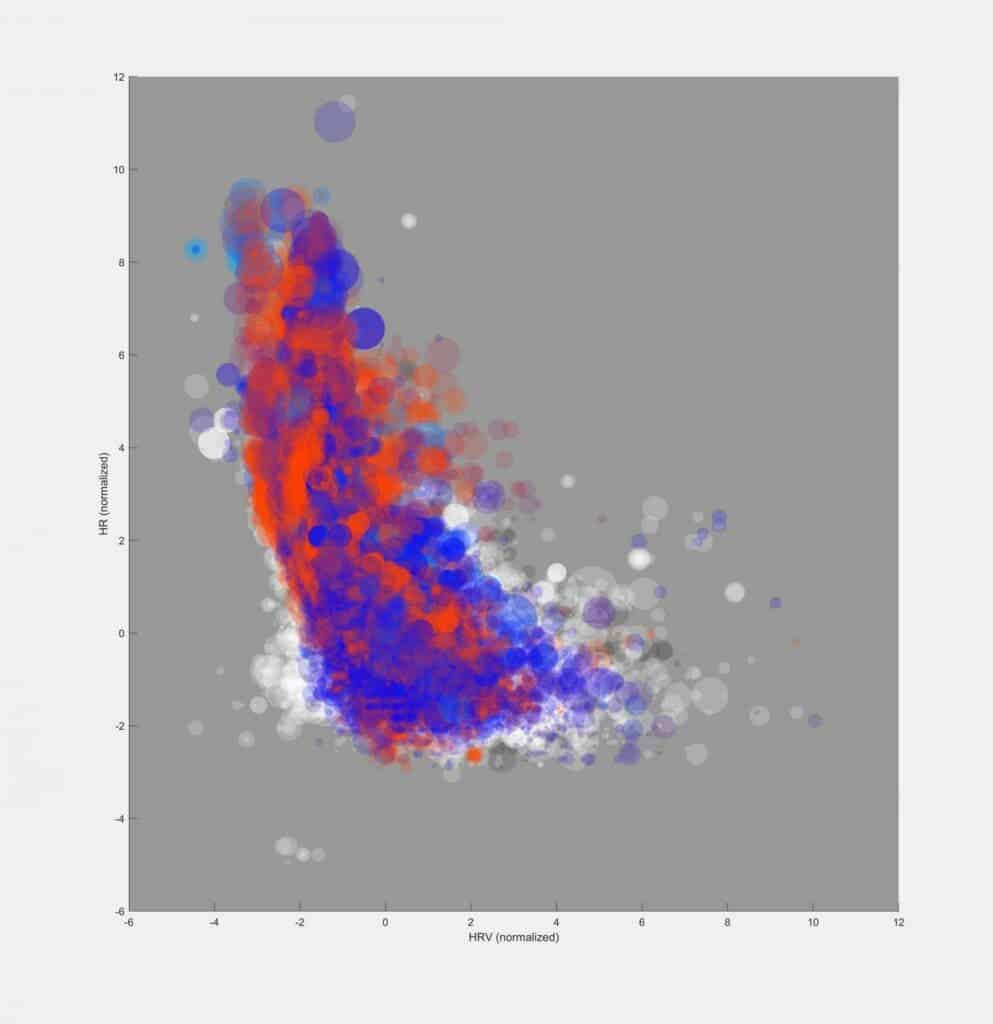
This is how the researchers noticed that temperature signals corresponding to fever among those sick with COVID-19 were very obvious. In fact, the chart tracking people who had a fever looked like it was on fire, Smarr said.
While the sample size of this study is too small to draw conclusions for the general population, the authors claim that their study raises some important questions. How many so-called asymptomatic cases are truly asymptomatic, for instance? How many might just be unnoticed or underreported?
“If wearables allow us to detect COVID-19 early, people can begin physical isolation practices and obtain testing so as to reduce the spread of the virus,” Ashley Mason, a professor in the Department of Psychiatry and the Osher Center for Integrative Medicine at UC San Francisco, said in a statement. “In this way, an ounce of prevention may be worth even more than a pound of cure.”
The researchers are currently working on an algorithm that can predict the onset of symptoms such as fever, cough, and fatigue. They hope to have it ready by the end of the year.






