A new approach seems poised to make the HIV vaccine a reality.
Researchers at Scripps Research have successfully overcome past technical hurdles to creating a new HIV vaccine; the compound was shown to stimulate a powerful anti-HIV antibody response in animal models.
Enveloping attack
The team based their vaccine on a new strategy (which they describe in their paper). They drew on HIV’s envelope, Env, which is a complex, shape-shifting molecule. Env has previously thwarted vaccine-production efforts since it’s difficult to produce in vaccines in a way that induces useful immunity to HIV.
In order to stabilize Env into a shape that’s useful for the diverse strains of HIV, the team broke it down into several components. Afterward, they stitched them back together on virus-like particles (meant to mimic a whole virus). Stabilized in this fashion, the Env proteins elicited strong anti-HIV antibody responses in mice and rabbits.
“We see this new approach as a general solution to the long-standing problems of HIV vaccine design,” says principal investigator Jiang Zhu, associate professor in the Department of Integrative Structural and Computational Biology at Scripps Research.
One of the main functions of the Env molecule is to grab onto host cells and break through their membrane to initiate infection. Given its vital role, and the fact that this part of the virus has the most exposure to a host’s immune system, Env has been the main target for HIV vaccine efforts. The usual approach was to inoculate people with Env proteins (or bits of them) to coax their bodies into producing Env-binding antibodies. These antibodies would then keep HIV from infecting further cells in the future.
Up until now, that hasn’t work out. The current prevailing hypothesis is that for an HIV vaccine to be effective, it needs to present the Env proteins in a way that closely resembles the original virus. This, however, is a huge challenge. Env protrudes from the viral membrane in tight clusters of three — called trimers — which can take radically different shapes before and after infecting cells. Researchers have failed to find a broadly applicable method for stabilizing Env trimers in the pre-infection shape.
“The trimer-stabilization solutions that have been reported so far have worked for a few HIV strains but have not been generalizable,” Zhu says. “Env trimer ‘metastability’, as we call it, has really been a central problem for trimer-based HIV vaccine design.”
The team drew on Zhu’s previous work, in which he showed that altering a short section of ENV (called HR1) might force Env to stay in the pre-infection (closed) shape. The new paper shows that this strategy does indeed work for diverse HIV strains from all over the world. This “uncleaved prefusion-optimized” (UFO) approach allows researchers to produce Env trimmers in their closed shape with surprising ease and little need for purification starting from pretty standard cells (from a biotech manufacturing point of view). Zhu’s team reports successfully applying the UFO process to “30 to 40 different HIV strains” so far. In most cases, “it has worked like a charm,” Zhu says.
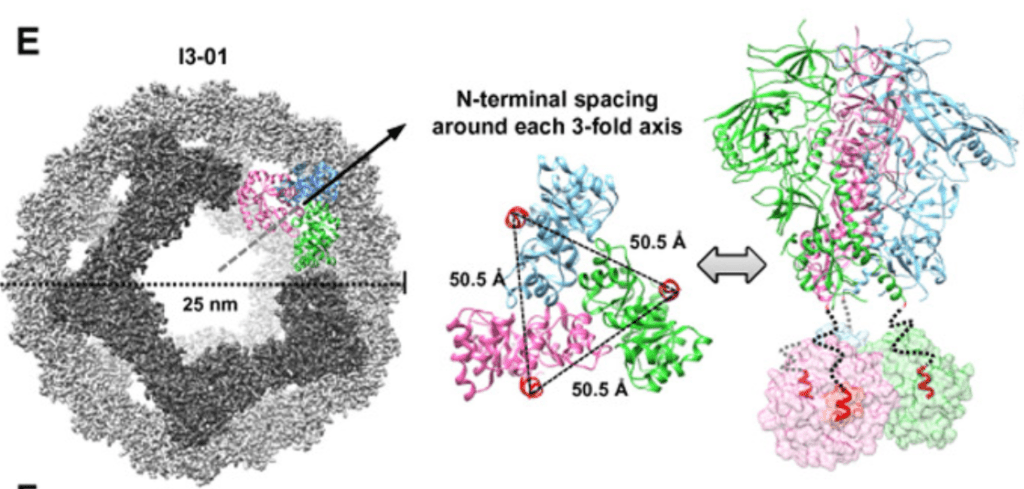
The researchers further refined the vaccine by genetically linking 60 such stabilized Env trimmers to individual nanoparticles that mimic the shape of a virus. The resulting vaccine molecule cannot replicate like a real virus but looks enough like one to the immune system to coax it into action.
Lab tests on mice showed that treatment with these faux viruses led to the production of antibodies that successfully neutralized HIV in only eight weeks. Even better, the HIV strain used to confirm the vaccine’s effectiveness was of a type that prior candidate vaccines generally have failed against.
“This is the first time any candidate HIV vaccine has induced this desired type of antibody response in mice,” Zhu says. Similarly unprecedented results were obtained in rabbits, demonstrating that the nanoparticle-based approach is clearly superior to the use of isolated Env proteins — it elicits a significantly stronger response and does so much more quickly.
Further tests are now underway in 24 monkeys at the National Institutes of Health-sponsored Southwest National Primate Center in San Antonio, Texas.
“We’re now testing two candidate vaccines based on Env trimers from different HIV strains, plus a third candidate vaccine that is a cocktail of three Env-based vaccines,” says Ji Li, CEO of Ufovax, a startup company that has licensed Zhu’s vaccine technology. “We think this new approach represents a true breakthrough after 30 years of HIV vaccine research.”
The paper “HIV-1 vaccine design through minimizing envelope metastability” has been published in the journal Science Advances.
Was this helpful?



