Scientists from Australia and Japan have invented a blood test that assesses the levels of beta-amyloid build-up in the brain. Beta-amyloids are amino acids crucially involved in Alzheimer’s disease.

The battle against Alzheimer’s is a hard one
Accumulation of beta-amyloid decreases neuronal activity in large areas of the brain. However, beta-amyloid builds up in the brain of an Alzheimer’s patient decades before any clinical signs — such as cognitive problems and loss of memory — show up. This means that in theory, detecting beta-amyloid could enable physicians to detect Alzheimer’s before it actually sets in.
For decades, scientists have been trying to design a blood test, especially as current methods are expensive and cannot be used as screening methods on a large scale. Nowadays, doctors use positron emission tomography imaging (PET scans) or cerebrospinal fluid (CSF) analysis via spinal tap or lumbar puncture to diagnose the disease. That’s not only expensive, but also invasive, unpleasant, and time-consuming. Having a simple blood test could change all that.
However, designing a screening test for the disease has proven extremely difficult as relatively little beta-amyloid is found in the bloodstream, compared to how much lies in the brain. Most past studies have failed to find a correlation between the two but now for the first time, researchers believe they have finally cracked that problem.
Colin Masters, a professor of neuroscience at the Melbourne-based Florey Institute, who has spent 30 years researching an Alzheimer’s test, said mass spectrometry was more sensitive and accurate at detecting beta-amyloid levels than PET brain scans and lumbar punctures. He managed to successfully use this technique to detect beta-amyloid building up in the blood.
“By the time you hit 60 to 70 about 30% of the population are showing signs of this protein aggregating in their brain and that can be picked up now with this blood test,” said Prof Masters.
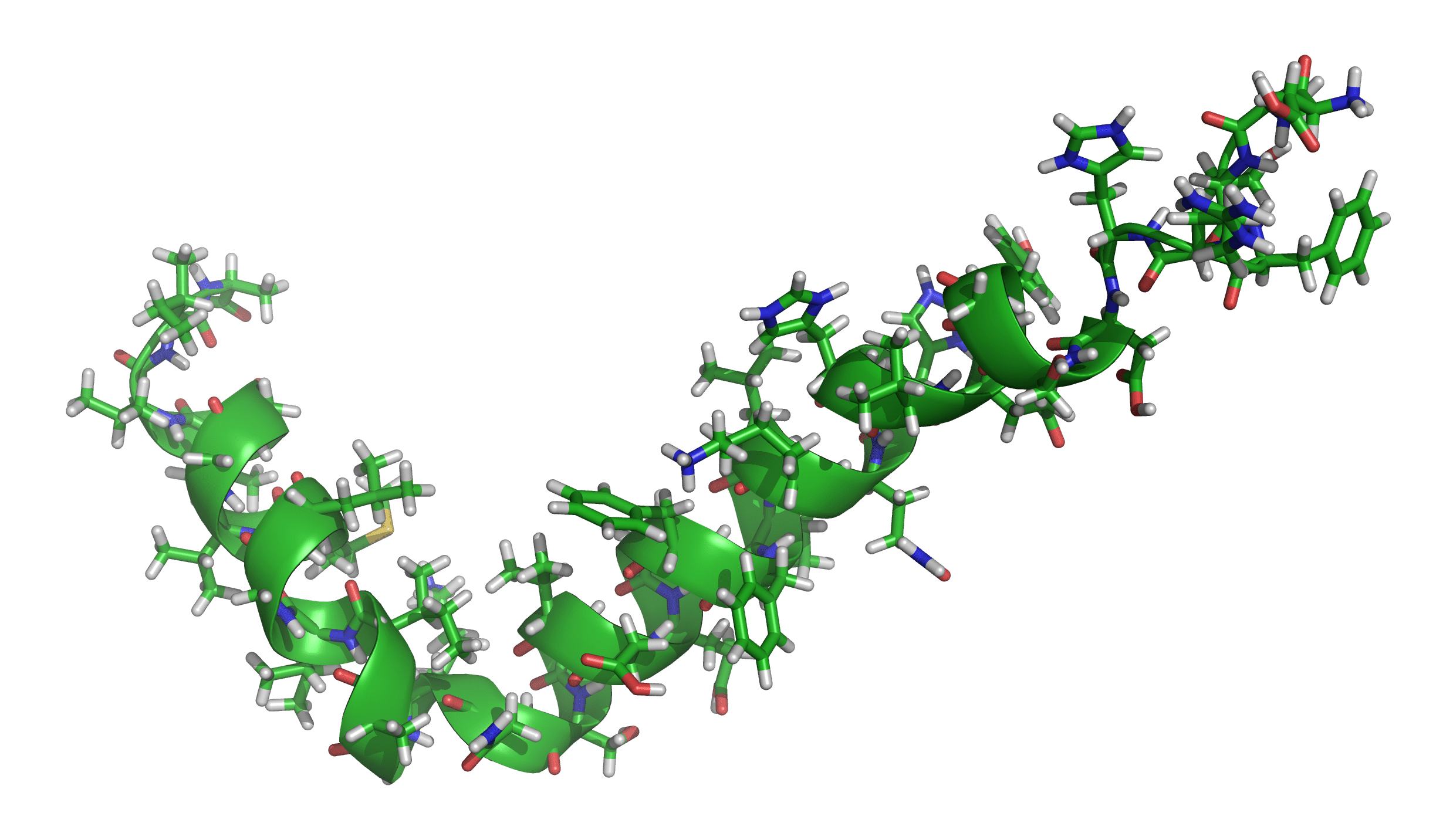
Via: Wikipedia
The blood test, a new hope
A new, painless and more cost-effective Alzheimer’s test could help more people know if they are on the path of developing this condition. This could not only help detect Alzheimer’s quicker and more efficiently, but it could also help researchers ultimately find a cure — ensuring that future medical trials have numerous suitable participants, something which has proven challenging. Usually, present participants have late-stage Alzheimer’s that is treatment-resistant. It is extremely difficult to see if a kind of medicine is helping without having numerous early-stage patients enrolled in trials. If this simple blood test gets scientific approval, it might turn the odds in researchers’ favor.
“If a person knows they are on this pathway well before the onset of any cognitive impairment some would want to alter their lifestyles,” Prof Masters said.
The study included 121 people from Japan and 252 from Australia, both groups involving Alzheimer’s patients with normal brain function and mild cognitive impairment. Researchers found the amount of amyloid present in the blood correlated with the degree of cognitive impairment. Amyloid levels also correlated with findings in the same patients from classical diagnostic tools, PET scans, and CSF measures.
James Hendrix, director of Global Science Initiatives for the Alzheimer’s Association (the largest nonprofit funder of Alzheimer’s research), who was not involved in the new research, thinks that this is a truly important study.
“It is from a top research team. It is a decently large sample size. And most important, they are correlating their results to PET and CSF. That cross-validation to other techniques is great to see—we haven’t seen this before for a blood test in Alzheimer’s,” he said in a statement.
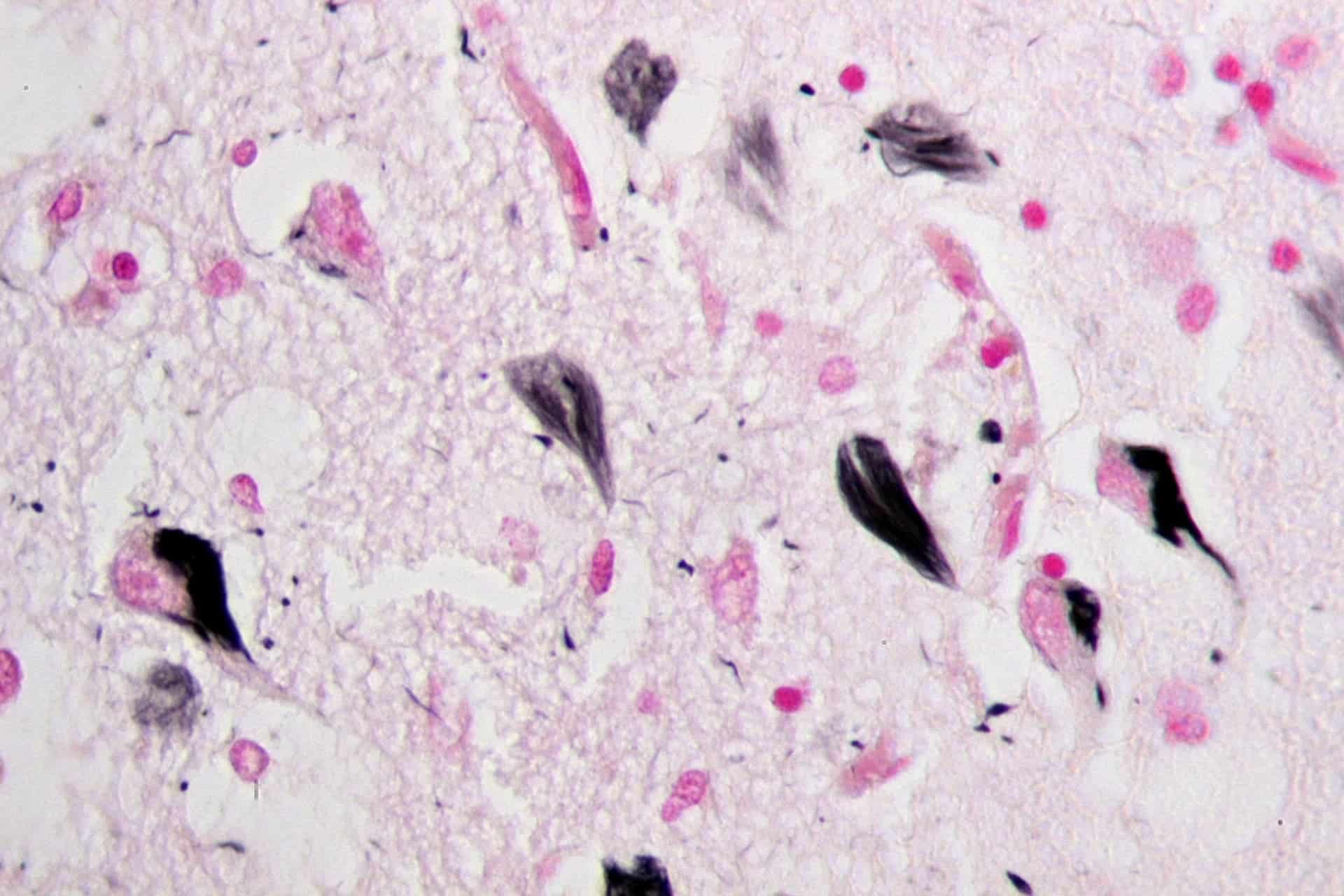
Via: Wikipedia
“I can see in the future, five years from now, where people have a regular checkup every five years after age 55 or 60 to determine whether they are on the Alzheimer’s pathway or not,” hopes Prof Masters.
The paper was published Jan. 31 in the journal Nature.