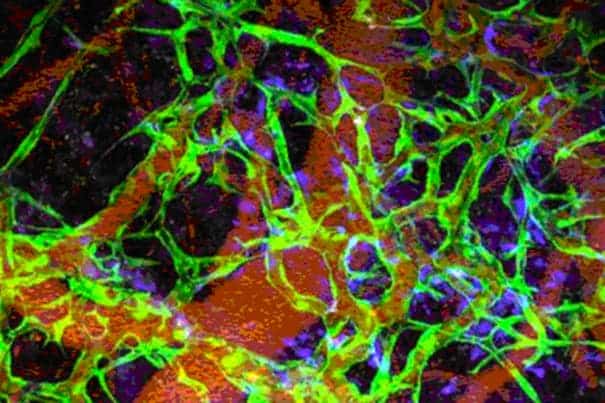
Researchers at Harvard-affiliated Massachusetts General Hospital (MGH) have successfully grown and inserted functional blood vessels into animal models after they used vascular precursor cells derived from human induced pluripotent stem cells (iPSCs). These blood vessels lasted for as long as nine months, much longer than any previous attempt, making the Harvard researchers’ efforts seem extremely promising. Patients suffering from damaged blood vessels, like those suffering from type-1 diabetes, could particularly benefit.
“The discovery of ways to bring mature cells back to a ‘stemlike’ state that can differentiate into many different types of tissue has brought enormous potential to the field of cell-based regenerative medicine, but the challenge of deriving functional cells from these iPSCs still remains,” says Rakesh Jain, Andrew Werk Cook Professor of Radiation Oncology (Tumor Biology) at Harvard Medical School (HMS), director of the Steele Laboratory for Tumor Biology at MGH, and co-senior author of the study. “Our team has developed an efficient method to generate vascular precursor cells from human iPSCs and used them to create networks of engineered blood vessels in living mice.”
Indeed, only in recent years has the opportunity of developing stemlike cells from mature cells surfaced, but even so advances so far have been remarkable. This isn’t the first attempt at creating blood vessels from iPSCs, though. Previous studies attempted to generate the types of cells required to build blood vessels — endothelial cells that line vessels and connective tissue cells that provide structural support — however either these didn’t last very long or didn’t work at all once they were inserted inside the animal model.
Generating blood vessels from adult cells
The team of researchers at Harvard had to face this challenge, so they adapted a method originally used to derive endothelial cells from human embryonic stem cells (hESCs). That method uses a single protein marker to identify vascular progenitors; in this study, the researchers sorted out iPSC-derived cells that expressed not only that protein but also two other protein markers of vascular potential. They then expanded that population using a culture system that team members had previously developed to differentiate endothelial cells from hESCs, and they confirmed that only iPSC-derived cells expressing all three markers generated endothelial cells with the full potential of forming blood vessels.
These cells, in combination with mesenchymal precursors that generate essential structural cells, were then put to the test and inserted onto the surface of the brains of mice. Within two weeks, the implanted cells had formed networks of blood-perfused vessels that appeared to function as well as adjacent natural vessels and continued to function for as long as 280 days in the living animals. The same combination was also implanted under the skin of mice, however this procedure required five times as many cells to work properly.
The researchers also worked with iPSCs derived from the cells of patients with type 1diabetes (T1D), which often causes damage to blood vessels. As with cells from healthy individuals, precursors derived from T1D-iPSCs were able to generate functional, long-lasting blood vessels. Key differences in cell generation potential were noticed, however, which require more study.
“The potential applications of iPSC-generated blood vessels are broad — from repairing damaged vessels supplying the heart or brain to preventing the need to amputate limbs because of the vascular complication of diabetes,” says co-lead author Rekha Samuel, formerly of the Steele Laboratory and now at Christian Medical College, in Vellore, India. “But first we need to deal with such challenges as the variability of iPSC lines and the long-term safety issues involved in the use of these cells, which are being addressed by researchers around the world. We also need better ways of engineering the specific type of endothelial cell needed for specific organs and functions.”
The findings were documented in a report published in the journal Proceedings of the National Academy of Sciences(PNAS) Early Edition.
Was this helpful?



