The production of polio vaccine could be revolutionized, Norwich researchers say. The process is cheap, fast, and effective.
A leafy vaccine

A multidisciplinary team of researchers from the John Innes Centre has hijacked a relative of the tobacco plant and turned it into a “factory” for polio vaccine. They used virus-like particles (VLPs), which resemble viruses but are not infectious and contain no viral genetic material. Think of it like a mannequin — on the surface, it looks just like the real thing, but there’s nothing inside.
The good thing about this approach is that it has all that’s needed to train the immune system to fight the real virus, without putting it at any risk. In this case, researchers genetically engineered a VLP which looks just like the polio virus. Then, the genetic material was implanted into bacteria which then infected plants. As the infection unfolded, the plants started producing the virus-like particles which can be used for the vaccine.
To extract the particles, leaves were simply mixed with water, blended, and the polio vaccine was extracted. This final part of the process is extremely simple but taken together, the entire process is highly innovative and creative. The only thing that’s left is to scale it up.
Professor Lomonossoff, from the John Innes Centre said:
“This is an incredible collaboration involving plant science, animal virology and structural biology. The question for us now is how to scale it up – we don’t want to stop at a lab technique.”
The beauty of it is that given the nature of the process, you don’t need more complex lab equipment to scale it up — just more greenhouses.
“The beauty of this system of growing non-pathogenic virus mimics in plants, is that it boosts our ability to scale-up the production of vaccine candidates to combat emerging threats to human health,” said Prof Lomonossoff.
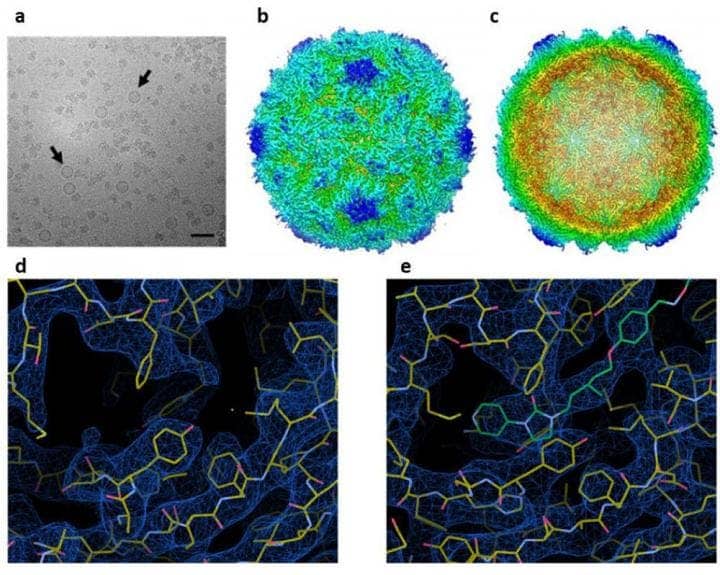
Lab tests indicated that the virus-like particles are able to generate an adequate response from the immune system — basically, it acts as a vaccine.
Using plants instead of bacteria and yeast is an attractive proposition which has been attempted before. It’s not the first time VLPs have been grown in plants, but previously, VLPs of papilloma and hepatitis B viruses had proven too unstable to make practical vaccines using this technique. The main problem is the missing viral DNA which holds the cell together. The British researchers managed to bypass this technique, and they say that it can be applied to other diseases as well.
“In an experiment with a Canadian company, they showed you could actually identify a new strain of virus and produce a candidate vaccine in three to four weeks,” Lomonossoff told the BBC. “It has potential for making vaccines against emerging epidemics, of course recently we had Zika and prior to that we had Ebola. It’s highly responsive, and that’s one of the great attractions of the technology.”
But it’s not all rosy just yet. Aside from proving the technique with other viruses, there are also legal hurdles to pass. Dr Tarit Mukhopadhyay, a lecturer in vaccine development at University College London, said:
“The initial results look impressive. However, there are very few plant-based vaccine manufacturers and almost no licensed human vaccines that are currently produced in plants.”
Exterminating polio
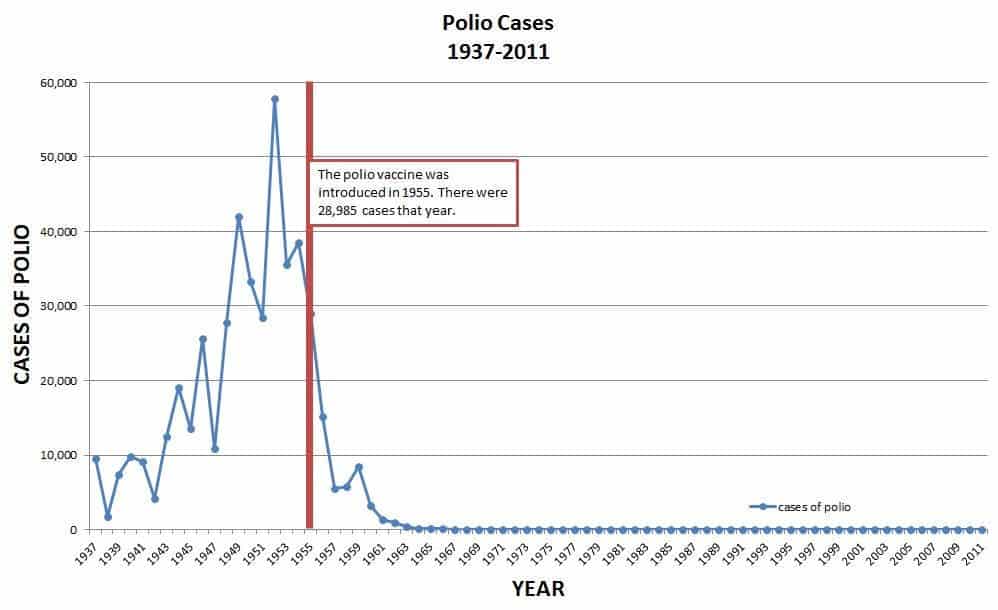
Still, if this technology lives up to its potential, we may be within reaching distance of truly exterminating polio. The crippling disease only manifests itself in 1% of all cases, but when it does, it can cause paralysis or even kill the patient. Since 1988, the Global Polio Eradication Initiative led by the WHO has reduced the prevalence of the disease by over 99%, and there are currently only three countries where polio is endemic — but it can still be “imported” from place to place.
Just recently, the UN declared Somalia polio-free, after three years without a new case. But continuing with the vaccination campaign is vital if we want to rid the world of the virus. In Syria, as the civil war prevented the vaccination campaigned, new cases of polio started to emerge.
The problem is that current vaccines require massive amounts of the virus to be produced. Aside from potential shortages (which have been reported in recent years), using the live virus not only represents a risk of the virus escaping, the use of the live attenuated (weakened) virus, effectively maintains polio in the global population.
The endgame of polio is in sight, but we need to make the right steps to avoid nasty surprises. So far this year, there have been 45 cases of polio; still, there’s a big difference between 45 and zero.



