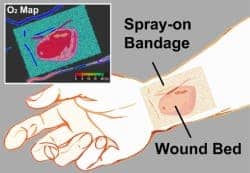
An interdisciplinary team of researchers has created a paint-on, see-through, “smart” bandage that glows to indicate a wound’s tissue oxygenation concentration. Oxygenation plays a crucial role in healing, so mapping it in severe wounds and burns can help to significantly improve the success of surgeries to restore limbs and physical functions.
“Information about tissue oxygenation is clinically relevant but is often inaccessible due to a lack of accurate or noninvasive measurements,” explained lead author Zongxi Li, an HMS research fellow on Evans’ team.
This bandage doesn’t only enable this in a non-invasive way, but does so three simple, compact and inexpensive components:
- – a bright sensor molecule with a long phosphorescence lifetime and appropriate dynamic range;
- – a bandage material compatible with the sensor molecule that conforms to the skin’s surface to form an airtight seal;
- – an imaging device capable of capturing the oxygen-dependent signals from the bandage with high signal-to-noise ratio.
Furthermore, the bandage is quite easy and painless to take off.
“The bandage comes off easily – the liquid bandage dries into a tacky gel underneath a plastic layer; the entire bandage comes off with simple peeling. We experimented on 20/1000 of an inch skin grafts, which are almost see-through and very fragile, and found that the bandage could be applied and removed without causing any damage”, team leader Conor L. Evans at the Wellman Center for Photomedicine of Massachusetts General Hospital (MGH) and Harvard Medical School (HMS) said on Reddit.
How the smart bandage works

The bandage is applied like a viscous liquid which then solidifies in less then a minute. After it has dried, a transparent barrier layer is then applied atop it to protect the film and slow the rate of oxygen exchange between the bandage and room air, making the bandage sensitive to oxygen coming from only inside the skin. Oxygenation is very important in dealing with wounds.
“Oxygen plays an important role in wound healing, as it is essential to biological functions such as cell proliferation, immune responses and collagen synthesis. Poor oxygenation is directly associated with the development of chronic ischemic wounds, which affect more than 6 million people each year in the United States alone at an estimated cost of $25 billion”, the authors write.
The key to the glow is phosphorous – an element which can absorb light wavelengths and then release them, glowing. The more oxygenation, the stronger they glow.
“How brightly our phosphorescent molecules emit light depends on how much oxygen is present,” said Li. “As the concentration of oxygen is reduced, the phosphors glow both longer and more brightly.”
The last element is a camera-based readout device which does two things: triggers the emission of the phosphors inside the bandage and then monitors the phosphorous emission.
“Depending on the camera’s configuration, we can measure either the brightness or color of the emitted light across the bandage or the change in brightness over time,” Li said. “Both of these signals can be used to create an oxygenation map.”
Applications and further development
The applications of such a bandage are pretty straightforward – they could monitor the developments of severe wound and burns, especially in ischemic (restricted blood supply) conditions, postoperative monitoring of skin grafts or flaps, and burn-depth determination. The fact that this can be done cheaply and in a non-invasive way make it all the more betteer.
“The need for a reliable, accurate and easy-to-use method of rapid assessment of blood flow to the skin for patients remains a clinical necessity,” said co-author Samuel Lin, an HMS associate professor of surgery at Beth Israel Deaconess Medical Center. “Plastic surgeons continuously monitor the state of blood flow to the skin, so the liquid-bandage oxygenation sensor is an exciting step toward improving patient care within the realm of vascular blood flow examination of the skin.”
But even though the achievement is remarkable in itself, the team is already working on future developments.
“We’re developing brighter sensor molecules to improve the bandage’s oxygen sensing efficiency,” said Emmanuel Roussakis, another research fellow in Evans’ laboratory and co-author, who is leading the sensor development effort.
They are also working on revealing other parameters aside for oxygenation – such as pH, bacterial level and specific disease markers.
“In the future, our goal for the bandage is to incorporate therapeutic release capabilities that allow for on-demand drug administration at a desired location,” says Evans. “It allows for the visual assessment of the wound bed, so treatment-related wound parameters are readily accessible without the need for bandage removal—preventing unnecessary wound disruption and reducing the chance for bacterial infection.”
It’s also important to note that this bandage has a shelf life of over a year – so it’s quite likely that we’ll be seeing it in practice in the near future.
Journal Reference: Zongxi Li, Emmanuel Roussakis, Pieter G. L. Koolen, Ahmed M. S. Ibrahim, Kuylhee Kim, Lloyd F. Rose, Jesse Wu, Alexander J. Nichols, Yunjung Baek, Reginald Birngruber, Gabriela Apiou-Sbirlea, Robina Matyal, Thomas Huang, Rodney Chan, Samuel J. Lin, and Conor L. Evans. Non-invasive transdermal two-dimensional mapping of cutaneous oxygenation with a rapid-drying liquid bandage. Biomedical Optics Express, Vol. 5, Issue 11, pp. 3748-3764 (2014). http://dx.doi.org/10.1364/BOE.5.003748