Researchers in the UK have devised a bandage-like biomaterial that transplants stem cells into severe bone fractures. The easily applied bandage significantly speeds up the healing process, improves recovery, and reduces the risk of infections and poor outcomes for very serious injuries.
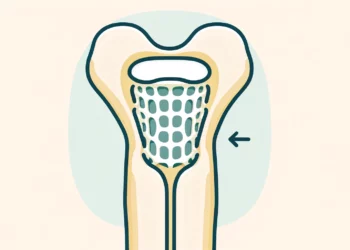
The biomaterial developed at King’s College London simulates structures that are part of healthy human bones. The bandage can then be stuck to a fracture like a plaster, amplifying the natural healing process.
In order to speed up bone healing, the bandage is coated in a protein involved throughout the body in the growth and repair of tissue. Additionally, the material grows bone cells from stem cells in a 3-D gel embedded in the bandage. When the bandage is patched to a fracture, these bone cells are transplanted to the site of injury.
Most broken bones do not require intensive medical care. Typically, doctors will put a broken arm or leg into a cast. The cast doesn’t heal broken bones on their own, but rather hold the affected area in place so the bone heals naturally and straight.
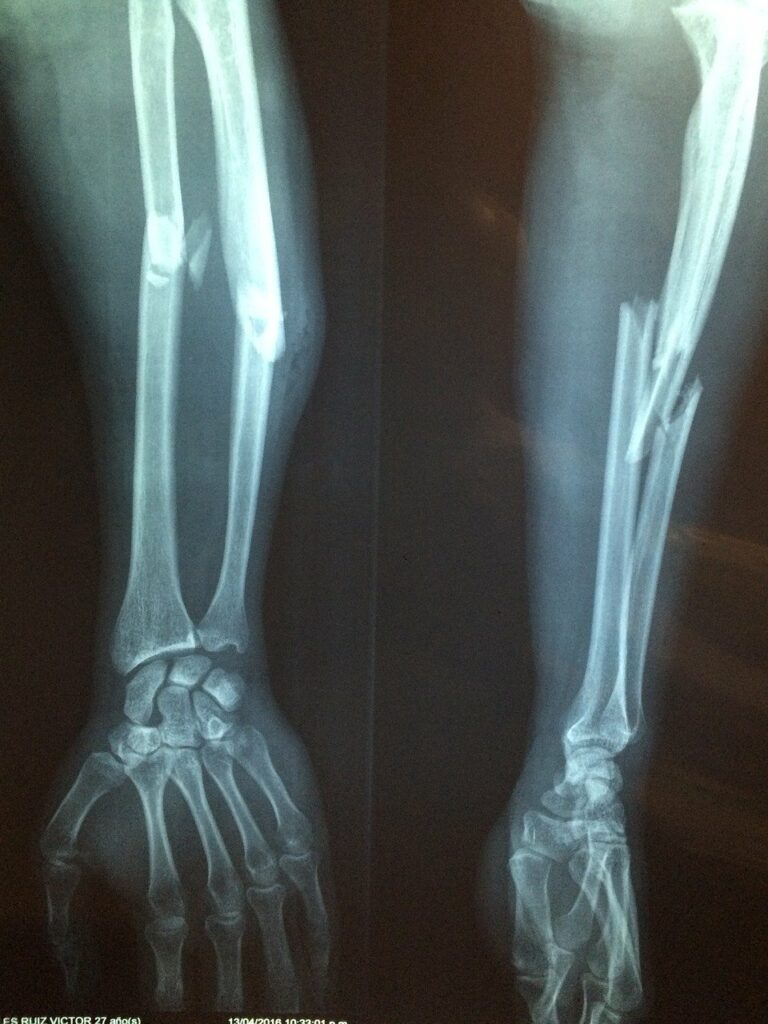
In particularly severe fractures, surgery is often necessary. Sometimes, doctors will insert metal pins and other implants to hold everything in place while the bone heals. Other times, instead of synthetic implants, bone is taken from elsewhere in the body for transplant at the site of injury.
However, following a serious injury, the body’s ability to heal is weakened. This is particularly true for the elderly.
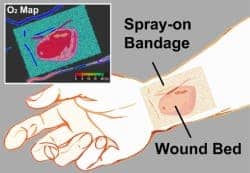
This is why a ‘bone-like bandage’ is appealing: it supports and accelerates the healing of bone fractures without the need for synthetic implants. It is also biocompatible and safe as the researchers designed it to specifically target fracture sites, so it does not leak to healthy tissue.
“Our technology is the first to engineer a bone-like tissue from human bone stem cells in the lab within one week, and successfully transplant it in the bone defect to initiate and accelerate bone repair. The concept of the 3D-engineered tissue and the bandage has the potential to be developed to different injured tissues and organs,” first author Dr. Shukry Habib, from King’s College London, said in a statement.
The findings were reported in the journal Nature Materials.