A team of researchers from the University of Southern California (USC) and UC San Francisco (UCSF) has mapped the relationship between patterns of activity in the brain and mood variation. Based on these links, the team built an automated ‘decoder’ that can predict changes in a patient’s mood by monitoring their brain activity.

The findings very encouraging — they could lead to new and more effective treatments for mood and anxiety disorders, especially for patients that do not respond to conventional treatments.
Think of a number, any number
While not an actual mind-reading device, the team’s decoder comes pretty close. Its development is a significant step towards novel, closed-loop therapies that use brain stimulation to help treat the millions of patients suffering from debilitating disorders that other avenues of treatment simply fail against.
For the study, the team recruited seven volunteers. All participants were part of a group of epilepsy patients that had previously had electrodes implanted in their brain to monitor their seizures. Electrode implantation and data collection were handled by the UCSF team, led by Edward Chang, Professor of Neurological Surgery. The decoder itself was developed and built by the USC team, led by Assistant Professor and Viterbi Early Career Chair in Electrical Engineering, Maryam Shanechi.
Across multiple days of monitoring, the researchers recorded large-scale signals generated by the participants’ brains. Signals were continuously recorded from all the seven human volunteers. At the same time, they were periodically asked to fill mood questionnaires on a tablet, so the team could track their emotional state over time. The questionnaires were 24-question-strong, each asking the patient to “rate how you feel now” by tapping one of 7 buttons (which were spread on a continuum between fully-negative and full-positive states, e.g., “depressed” and “happy”). A higher score corresponded to a more positive mood state.
Starting from this data, Shanechi’s team developed the process through which mood variations can be predicted over time starting from each subject’s brain signals — the first time such a technique has been developed.
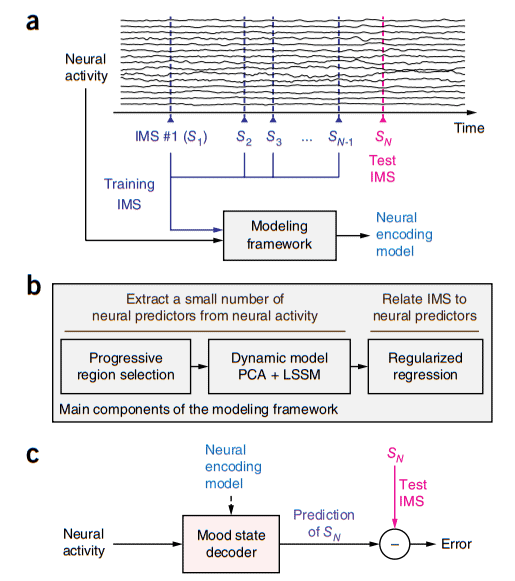
Image credits Omid Sani et al., 2018, Nature.
“Mood is represented across multiple sites in the brain rather than localized regions, thus decoding mood presents a unique computational challenge,” Shanechi said. “This challenge is made more difficult by the fact that we don’t have a full understanding of how these regions coordinate their activity to encode mood and that mood is inherently difficult to assess.”
“To solve this challenge, we needed to develop new decoding methodologies that incorporate neural signals from distributed brain sites while dealing with infrequent opportunities to measure moods.”
Shanechi’s team looked at the participants’ brain signals (distributed across different brain regions) side-by-side with their self-reported moods. This allowed them to spot which patterns of brain activity matched the self-reported moods. With this knowledge in hand, the researchers worked out an automated process that could independently recognize patterns of activity corresponding to each mood. Once built, the decoder showed it can predict mood variations in each patient over multiple days of monitoring.
With over 16 million adults in the United States who suffered at least one major depressive episode in their lifetime (according to the 2016 National Survey on Drug Use and Health), the results of this paper are definitely welcome — especially since treatments such as selective serotonin reuptake inhibitors (SSRIs) can be effective in some but not all patients.
According to the National Institutes of Health-funded STAR*D trial — the longest study to evaluate depression treatments — almost 33% of major depression patients do not respond to treatment. For these people, alternative diagnosis and therapy methods may hold the key to a better quality of life. While open-loop brain stimulation therapy (i.e. treatments that are proactive rather than reactive to a patient’s state) does hold some promise, closed-loop approaches that can track a patient’s mood over time (which the team’s decoder make possible) and deliver a tailored response have the potential to be much more effective.
According to Shanechi, for clinical practitioners, a powerful decoding tool would provide the means to clearly delineate, in real time, the network of brain regions that support emotional behavior.
“Our goal is to create a technology that helps clinicians obtain a more accurate map of what is happening in a depressed brain at a particular moment in time and a way to understand what the brain signal is telling us about mood,” she said.
“This will allow us to obtain a more objective assessment of mood over time to guide the course of treatment for a given patient. For example, if we know the mood at a given time, we can use it to decide whether or how electrical stimulation should be delivered to the brain at that moment to regulate unhealthy, debilitating extremes of emotion. This technology opens the possibility of new personalized therapies for neuropsychiatric disorders such as depression and anxiety for millions who are not responsive to traditional treatments.”
The new decoding technology, Shanechi explained, could also be extended to develop closed-loop systems for other neuropsychiatric conditions such as chronic pain, addiction, or post-traumatic stress disorder.
The paper “Mood variations decoded from multi-site intracranial human brain activity” has been published in the journal Nature.
Was this helpful?



