US researchers say their test is 94% efficient at detecting people at high risk of Alzheimer’s disease. The question remains: what will you do after the diagnosis?
Alzheimer’s is a type of dementia that causes problems with memory, thinking and behavior. It affects around 5% of all people aged 65 and over and, in time, it can have crippling effects. Most people aren’t even aware they have Alzheimer’s until the symptoms become obvious. Testing is expensive and time-consuming, researchers say.
“Right now we screen people for clinical trials with brain scans, which is time-consuming and expensive, and enrolling participants takes years,” said senior author Randall J. Bateman, MD, the Charles F. and Joanne Knight Distinguished Professor of Neurology.
This is where the new blood test comes in. Bateman and colleagues found a way to measure levels of the protein amyloid-beta (a key indicator of Alzheimer’s) in the blood. They can then use this measurement to assess whether the protein has accumulated in the brain and make projections about a person’s likelihood to develop the disease. The analysis can also be combined with two other major risk factors for Alzheimer’s: age and the presence of a gene variant called APOE4 for even better accuracy.
When all these were included, the accuracy went up to 94% — and in some cases, it was even better than today’s existing standard of detection.
Notably, some blood tests were considered false positives because the blood test was positive for amyloid-beta, but the brain scan came up negative. However, for some people with this type of results, the tests turned out positive four years later — indicating that the blood test was quicker to predict the protein building than the brain scan.
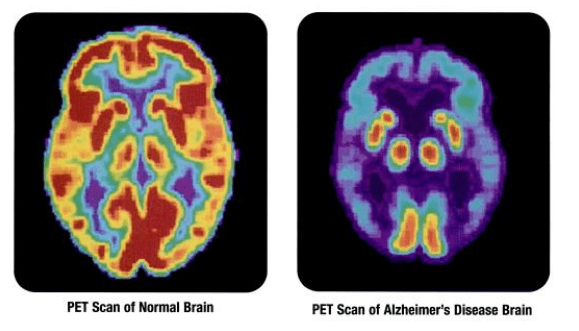
The price is also much lower. Blood tests typically cost a few tens or hundreds of dollars, whereas a PET scan, which is essential in diagnosing Alzheimer’s at the moment, can cost over $4,000 (and is typically used for patient care).
This is important because there is growing consensus among neurologists that while there is no real cure, there are ways to somewhat manage and delay the onset of the disease. By the time people become forgetful and Alzheimer’s is diagnosable, their brains are so severely damaged no therapy is likely to fully heal them.
Furthermore, researchers say, this could usher in a new age of Alzheimer’s research, opening the way to enrolling and analyzing more participants than ever before, with relative ease.
“With a blood test, we could potentially screen thousands of people a month. That means we can more efficiently enroll participants in clinical trials, which will help us find treatments faster, and could have an enormous impact on the cost of the disease as well as the human suffering that goes with it.”
The study High precision plasma amyloid-β 42/40 predicts current and future brain amyloidosis. Neurology. DOI: 10.1212/WNL.0000000000008081






