Malaria is one of the most common and dangerous diseases in the world, with the World Health Organization estimating over 200 million cases every year. There are several ways to try to treat malaria, but the results are debatable and often times not as effective as desired. Now, a team has demonstrated a new compound which effectively destroys malaria in 48 hours.
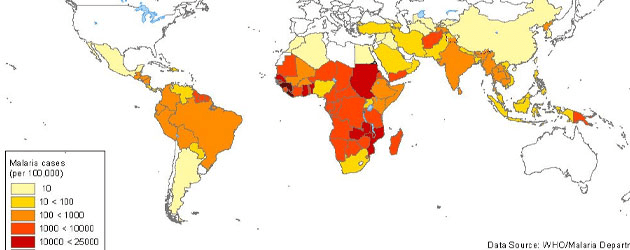
Malaria is a disease caused by parasitic protozoans (a type of single cell microorganism) which are carried by mosquitoes – if the mosquito bites you and sucks your blood, it also injects the parasite. The most affected countries are in Africa, but there is also a high incidence in South-East Astia and South America; it is associated with poverty, especially in areas with warm and wet climates which encourage the development of mosquito populations. It’s estimated that in Africa alone, the disease causes damages of $12 billion every year due to increased healthcare costs, lost ability to work and effects on tourism. Despite a need, no effective vaccine exists, although several promissing efforts to develop one are ongoing. The best way to fight the disease is to prevent mosquito bites with net and insect repellants, but when that doesn’t work and people do get infected, treatment options are often times limited and not very effective.
Now, researchers from St. Jude Children’s Research Hospital believe they have found a very good treatment for malaria. They developed a compound which targets only the red blood cells infected by the disease, leaving the healthy ones alone and basically wiping out the disease in 48 hours. Planning has begun for safety trials of the compound in healthy adults.
The compound is called (+)-SJ733, and it was identified in a previous study, with scientists now showing its effectiveness against malaria. In a mouse model of malaria, a single dose of (+)-SJ733 killed 80 percent of malaria parasites within 24 hours, and after another 24 hours, the parasite was undetectable. To make things even more interesting, the way the compound acts suppress development of drug-resistant parasites, which is very important.
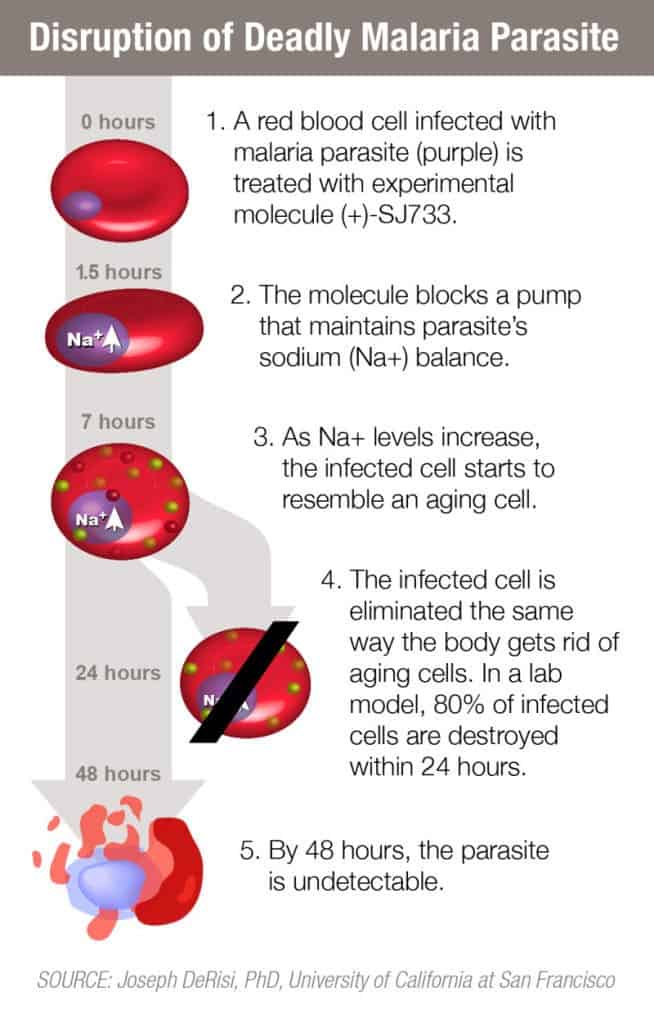
“Our goal is to develop an affordable, fast-acting combination therapy that cures malaria with a single dose,” said corresponding author R. Kiplin Guy, Ph.D., chair of the St. Jude Department of Chemical Biology and Therapeutics. “These results indicate that SJ733 and other compounds that act in a similar fashion are highly attractive additions to the global malaria eradication campaign, which would mean so much for the world’s children, who are central to the mission of St. Jude.”
My first reaction when I read the article was to be a bit worried. I mean, destroying infected red blood cells… that sounds a bit dangerous, right? Well, it’s actually really safe, and here’s why.
The way the malaria infection develops is as following – after an infection, you don’t get sick immediately. The disease first travels to the liver, where it stays for 1-4 weeks (usually); this is the incubation period. After the incubation period, the disease destroys the infected liver cells and enters the bloodstream. There, they infect the Red Blood Cells (RBC). They enter a RBC and multiply more and more until they burst out of it and move on to the next. This is generally why malaria causes cyclic fever – whenever it bursts out of RBCs and goes into the blood stream, you get a fever. RBCs are produced in bone marrow and normally have a life span of 3-4 months, after which they age and are destroyed by the body. The thing is, an infected RBC would be destroyed anyway by the virus – the drug does it in a nicer and safer way for the body – the compound isn’t destroying any additional cells.
“With this drug, only the red blood cells with a malaria parasite in them are affected. The malaria parasites life cycle is ~48 hours when it is infecting red blood cells, so you don’t actually “kill.. someone’s red blood cells” any more than if they weren’t taking the drug”, one of the authors said in a Reddit comment.
Planning has already begun for clinical trials; if the drug is deemed safe, it will start soon. It won’t hit the shelves anytime soon, as clinical trials tend to last for several years.
Journal Reference:
- María Belén Jiménez-Díaz, Daniel Ebert, Yandira Salinas, Anupam Pradhan, Adele M. Lehane, Marie-Eve Myrand-Lapierre, Kathleen G. O’Loughlin, David M. Shackleford, Mariana Justino de Almeida, Angela K. Carrillo, Julie A. Clark, Adelaide S. M. Dennis, Jonathon Diep, Xiaoyan Deng, Sandra Duffy, Aaron N. Endsley, Greg Fedewa, W. Armand Guiguemde, María G. Gómez, Gloria Holbrook, Jeremy Horst, Charles C. Kim, Jian Liu, Marcus C. S. Lee, Amy Matheny, María Santos Martínez, Gregory Miller, Ane Rodríguez-Alejandre, Laura Sanz, Martina Sigal, Natalie J. Spillman, Philip D. Stein, Zheng Wang, Fangyi Zhu, David Waterson, Spencer Knapp, Anang Shelat, Vicky M. Avery, David A. Fidock, Francisco-Javier Gamo, Susan A. Charman, Jon C. Mirsalis, Hongshen Ma, Santiago Ferrer, Kiaran Kirk, Iñigo Angulo-Barturen, Dennis E. Kyle, Joseph L. DeRisi, David M. Floyd, R. Kiplin Guy. ( )-SJ733, a clinical candidate for malaria that acts through ATP4 to induce rapid host-mediated clearance ofPlasmodium. Proceedings of the National Academy of Sciences, 2014; 201414221 DOI: 10.1073/pnas.1414221111
Was this helpful?