British researchers have shown that something as simple as undergoing a lung CT scan might help people quit smoking. Even if it comes out fine.

A smoking gun
The World Health Organization estimates that there are 1.1 billion smokers in the world — that’s every one in three adults. China is by far the biggest producer and consumer of cigarettes, with more than 350 million residents being smokers. India follows with 120 million smokers, while the US can ‘boast’ 36.5 million smokers. Tobacco ends up killing half of its users.
In recent times, smoking rates have gone down dramatically in the developed world. Countries like England and Australia are reporting all-time lows in smoking rates, partially fueled by higher taxes. In the European Union, banning smoking inside bars and clubs also played a vital role, but still — a worrying number of people still smoke, ignoring the numerous and far reaching health hazards.
The reasons why people start smoking aren’t really that varied. Most people start smoking in their teens, due to peer or cultural pressure (the smoking is cool idea). Almost 90% of smokers picked up the habit by 18, and 99% of smokers picked it up by the time they were 26. Usually, when smokers reach adulthood, they’re already addicted and find it very hard to quit. If you talk to most smokers, they’ll tell you they’ve tried quitting at least once but failed for one reason or another. There are countless books and ‘methods’ to quit smoking, but there’s no silver bullet. But we may be missing out on something fairly simple, a new study found: medical tests.
To quit or not to quit
Researchers from Cardiff University, King’s College London, Queen Mary University of London and the University of Liverpool’s Institute of Translational Medicine studied 4,055 participants aged 50 to 75. They were split into two groups: one that underwent low-dose CT screenings for their lungs, and a control group who didn’t undergo screening.
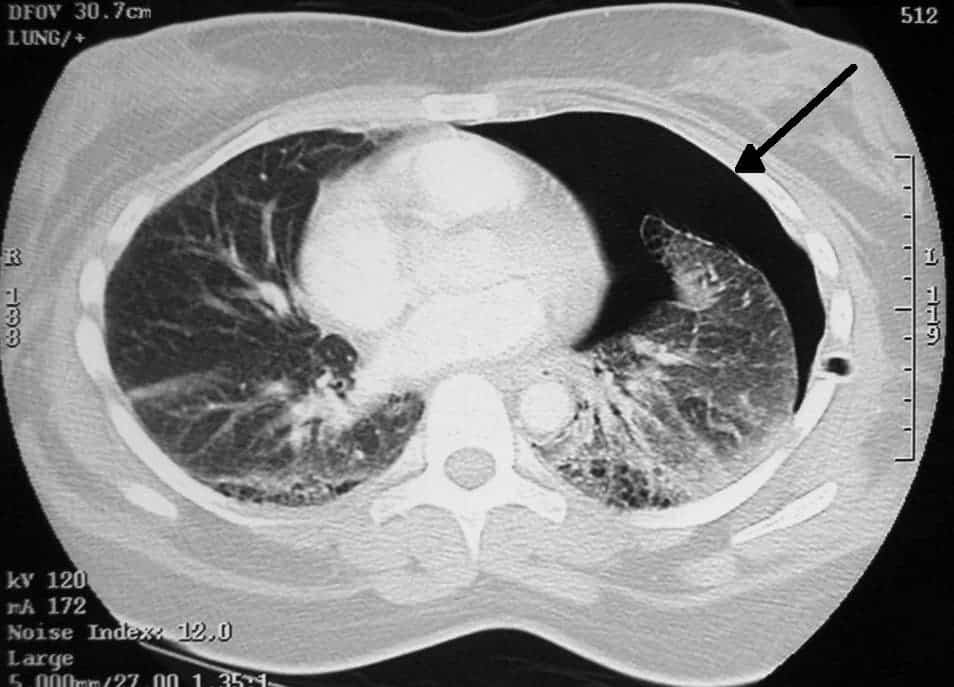
The control group reported cessation rates of five percent after two weeks and ten percent after two years. For the CT scan group, rates were ten percent and fifteen percent respectively — that’s a 100% and a 50% increase.
Perhaps most interestingly, this happened regardless of the study results. It was just the medical test itself that persuaded people to give up the nasty habit. Dr Kate Brain, from Cardiff University comments:
‘Our trial shows that CT lung cancer screening offers a teachable moment for smoking cessation among high-risk groups in the UK. We now need evidence about the best ways of integrating lung cancer screening with stop-smoking support, so that services are designed to deliver the maximum health benefits for current and future generations.’
Because this study actually had two groups (a CT scan and a control group), researchers also bypassed the “correlation is not causality” debate. Without this, you could have argued that people who opt for a CT scan care more about their health and are more likely to give up smoking — but this is a significant indication that the CT is causing the increased cessation rate.
It might not seem like much, but considering the sheer damage that smoking does, it’s an avenue that’s worth investigating. Prof John Field, University of Liverpool’s clinical professor of molecular oncology, chief investigator of the UK Lung Cancer Screening Trial believes that this can make a significant difference in tackling lung cancer.
‘The findings of this study dispute the belief that a negative screening result offers a “licence to smoke.” Engaging with lung screening can give smokers an opportunity to access smoking cessation support — at a time when they are likely to be more receptive to offers of help.’
However, CT scans are not easily available in all countries. It can be expensive, it can take months and months of waiting, or it may simply not be available. It would be interesting to see if results are similar for other, perhaps simpler tests.
Journal Reference: Kate Brain et al — Impact of low-dose CT screening on smoking cessation among high-risk participants in the UK Lung Cancer Screening Trial. http://dx.doi.org/10.1136/thoraxjnl-2016-209690






