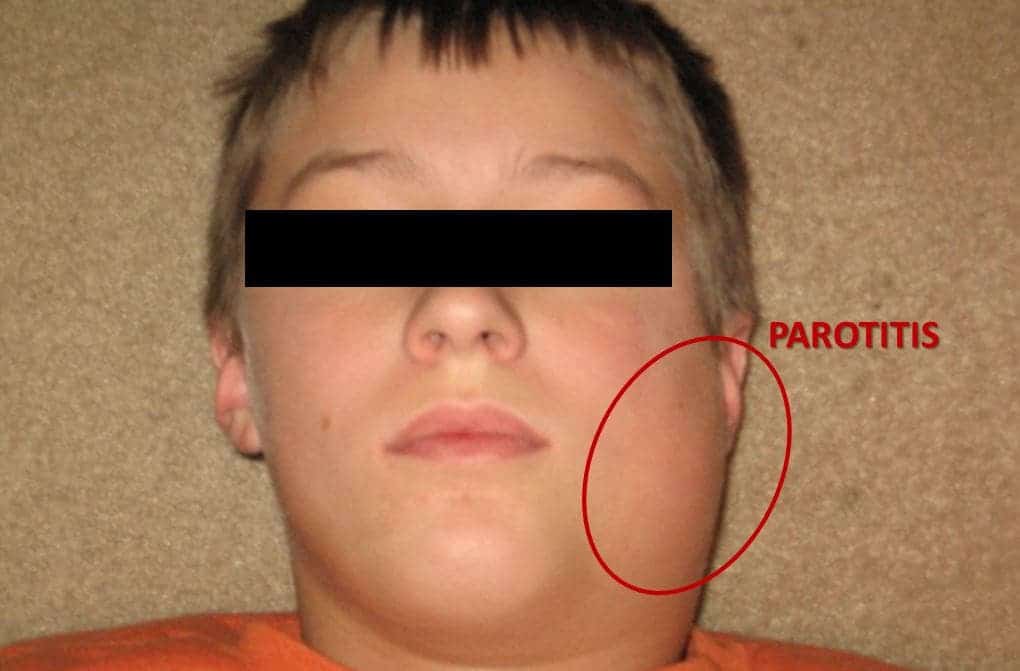
Parotitis is the inflammation and swelling of one or both salivary glands. The only known cause of epidemic parotitis among humans is mumps, a vaccine-preventable disease caused by the mumps virus, a member of the Rubulavirus genus of the Paramyxoviridae family. Before the approval of the mumps vaccine in the late 1960s, mumps was one of the most frequently reported diseases during childhood. Since 1990, the Advisory Committee on Immunization Practices (ACIP) has recommended children routinely receive two doses of measles–mumps–rubella vaccine (MMR) and this had a significant impact on reducing the occurrence of mumps.
According to two new articles published in Clinical Infectious Diseases, parotitis may be a complication of infection with the influenza virus. Both studies reviewed recent non-mumps related cases of parotitis following influenza and other viral infections, showing that after mumps had been ruled out, doctors and healthcare professionals should consider influenza when examining a patient who presents with parotitis. Furthermore, the investigators found that influenza A(H3N2), the flu strain behind the northern hemisphere 2017-2018 severe flu season, may be more likely to cause parotitis.
The first study by researchers from the US Centers for Disease Control and Prevention (CDC) investigated the etiology and clinical features of parotitis not caused by mumps during the 2014-2015 US influenza season in 320 American cases. The cases occurred in 27 states, mostly in men (65%). Almost two-thirds of patients (64%) were under 20 years of age. The subjects answered a questionnaire about their illness, and the CDC tested patient samples for several viruses. Viruses were detected in 210 buccal swab specimens (71%) of 294 non-mumps parotitis (NMP) patients with adequate samples for testing. These included 156 influenza A(H3N2), 42 human herpesvirus 6B (HHV6B), 32 Epstein-Barr virus (EBV), 8 human parainfluenza virus type 2 (HPIV2), 2 human parainfluenza virus type 3 (HPIV3), 3 adenovirus, 4 herpes simplex virus type 1 (HSV-1), and 1 herpes simplex virus type 2 (HSV-2). Influenza A(H3N2), HHV6B and EBV were the most frequently co-detected viruses. Because buccal swab specimens are not optimal for detecting influenza RNA, it is possible that the results underestimate the presence of influenza.
The second study by the same group of CDC researchers focused on interviews with 50 patients who had parotitis and were lab-confirmed to have an influenza infection between February to April of 2015. The results were compared with responses from 124 patients with lab-confirmed influenza infections that did not have parotitis. Patients described painful facial swelling, consistent with acute parotitis, which developed shortly after the onset of systemic or respiratory symptoms. Facial swelling lasted for about four days before subsiding. Seven cases were severe enough for the patients to be hospitalized during their illness, this includes two patients who were admitted to the intensive care unit (ICU). Their findings suggest that it may be prudent to include influenza in the differential diagnoses among patients who present with acute parotitis, particularly during flu seasons where influenza A(H3N2) is the dominant strain circulating.
So does the influenza virus cause parotitis?
Other reports of influenza A (H3N2) infection among patients with parotitis during the same flu season in Canada, England, and Scotland show that there is consistency.
In the accompanying commentary by Andrew Pavia, MD, of the Division of Pediatric Infectious Diseases at the University of Utah in Salt Lake City, he noted that the presence of the influenza virus detected in over half of patients with non-mumps parotitis adds strength to the association between flu and parotitis but does not prove it. He wrote, “In the absence of experimental data or the demonstration that influenza virus replicates in salivary glands, it will be hard to prove to a high degree of scientific certainty that influenza causes parotitis.” However, these two studies “strongly suggest that parotitis can be added to the long list of syndromes caused by influenza.”






