Treatment for a skin condition called psoriasis is also effective at removing the early plaque buildup that clogs arteries, restricts blood flow, and increases risk of heart attacks.
Psoriasis is a rather strange condition which affects around 2-4% of all people. It manifests as red or flaky patches of skin, usually on a person’s elbow, knee, or scalp, with the intensity of symptoms varying wildly — from a barely noticeable rash to painful eruptions which can be very unpleasant and painful.
We’re not really sure what causes it, but it seems that psoriasis is connected to faults of the immune system. Treatments for severe instances generally work by suppressing the immune system, keeping it at bay. Now, a new study has found that a particular treatment for severe psoriasis can also help reduce some heart issues.
“Psoriasis severity is related to the burden of coronary disease – our findings suggest treating the psoriasis may potentially benefit coronary heart disease,” said study author Dr Nehal Mehta, Chief of Inflammation and Cardiometabolic Diseases at the National Heart, Lung, and Blood Institute (NHLBI), National Institutes of Health (NIH), Bethesda, Maryland, US.
The treatment in case is called biological therapy — essentially, a type of drugs that suppresses the immune system. Biologic drugs are manufactured in a living system such as a microorganism, or plant or animal cells. They tend to be very large, complex molecules or mixtures of molecules and are often produced using recombinant DNA technology.
Arterial diseases develop when blood vessels become damaged or diseased. Cholesterol-containing deposits (plaque) can also clog them up and are one of the main causes of coronary artery disease. Previously, some studies have linked psoriasis with an early development of coronary plaque.
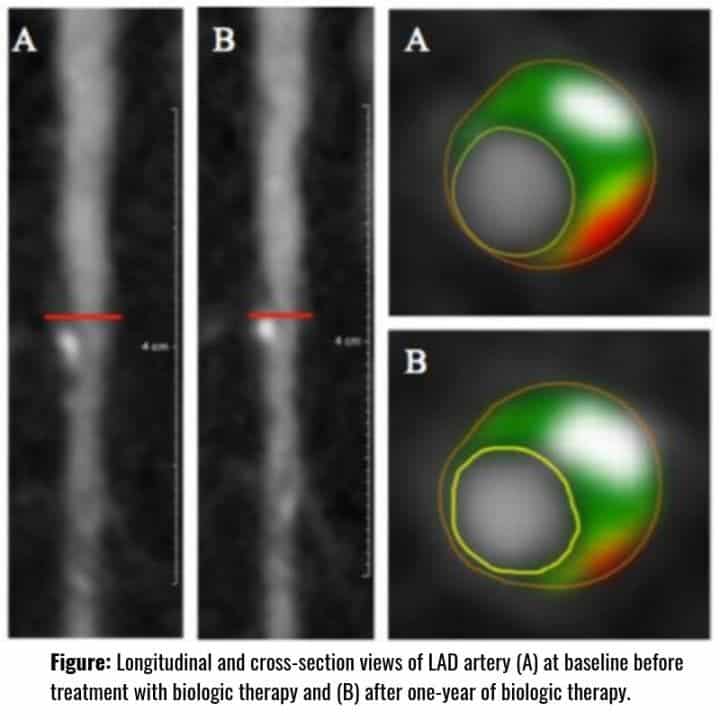
The study found that psoriasis patients who took biologic therapy for one year had an 8% reduction in coronary plaque burden, a frequent cause of heart attacks (see figure) — similar to the effect of a low dose statin, which is administered particularly to reduce cardiovascular disease. The make-up of coronary plaques also improved in those taking biologics, making them less hazardous.
At the same time, psoriasis patients who did not take biologic therapy had a 2% increase in the coronary plaque burden. The reason for this improvement is the reduction in inflammation — the drugs were effective at reducing overall inflammation, which appeared to also reduce the burden of plaque.
“We found that these anti-inflammatory drugs commonly used to treat severe psoriasis also improve plaque in the coronary artery making them more stable and less likely to cause a heart attack. This occurred in the absence of changes in traditional cardiovascular risk factors including blood pressure and blood lipids,” Mehta explains.
“This appears to be an anti-inflammatory effect. In the absence of improvement in other cardiovascular risk factors, and without adding new cholesterol medications, patients’ soft-plaque still improved. The only change was the severity of their skin disease,” said Mehta. He also says that many psoriasis sufferers don’t take immunosuppresants because they fear other infections.
In addition to shedding new light about psoriasis, this finding could also be used to reduce the global burden of heart disease. The 8% reduction might seem small, but considering that 15 million Americans, and many more worldwide, suffer from atherosclerotic cardiovascular diseases, and more than 7 million people worldwide suffer from a heart attack every year, the difference can be quite substantial.
However, further research is still required in order to confirm these findings. Since this is still an observational study, Mehta says they will now focus on a randomized, controlled trial.
The study has been published in Cardiovascular Research. DOI: 10.1093/cvr/cvz009



