The discovery of a human antibody that kept the deadliest strain of malaria at bay in mice studies provides new hope that we may finally defeat the parasite.

Image credits NIAID.
Malaria ticks all the right boxes for a horrible disease. First and foremost, it’s deadly. In cases when it’s not, malaria will nonetheless inflict some pretty terrible symptoms on you — ranging from headaches to paroxysm, quite severe brain damage and even coma. It will usually spring up again weeks or months after the initial infection, and tends to keep doing that until it finally gets you. It’s also infuriating to deal with, unless you like staying on the lookout for mosquitos 24/7.
Finally, it’s just kind of gross: malaria isn’t caused by a virus or a bacterium, but by parasitic protozoans — unicellular organisms capable of animal-like behavior such as complex movement or predation. They all belong to the Plasmodium genus, and the most dangerous among them is Plasmodium falciparum.
Despite considerable efforts, there is still no 100% effective, long-term vaccine against malaria — and because of that, the disease can still reap some 430,000 lives each year, primarily youngsters in sub-Saharan Africa.
The means to an end
New research carried out by a massive collaborative effort — bringing together researchers at the National Institute of Allergy and Infectious Diseases (NIAID), part of the National Institutes of Health, the Fred Hutchinson Cancer Research Center in Seattle, the Johns Hopkins Bloomberg School of Public Health in Baltimore, the Seattle Biomedical Research Institute, and Sanaria Inc., Rockville, Maryland — could finally give us the tools to reliably protect ourselves even from P. falciparum.
The story begins with the blood of a volunteer that had received an experimental vaccine made from whole, but weakened, malaria parasites (called PfSPZ Vaccine-Sanaria). In what biologists probably call a Darwinsend, this volunteer’s body actually produced an antibody to clear off the impaired parasites. The patient was later exposed to infectious, malaria-carrying mosquitos (this was performed under tightly controlled lab conditions, don’t try this at home) and did not become infected — the antibodies actually worked.
Called CIS43, these antibodies were isolated from the volunteer’s blood for further mouse trials. During these trials, CIS43 proved to be highly effective in preventing malaria infection. If additional human clinical trials confirm its anti-malaria effect, the team is confident that CIS43 could form the launching pad for a new prophylactic (i.e. preventive) treatment against malaria, one that should confer resistance for several months after administration.
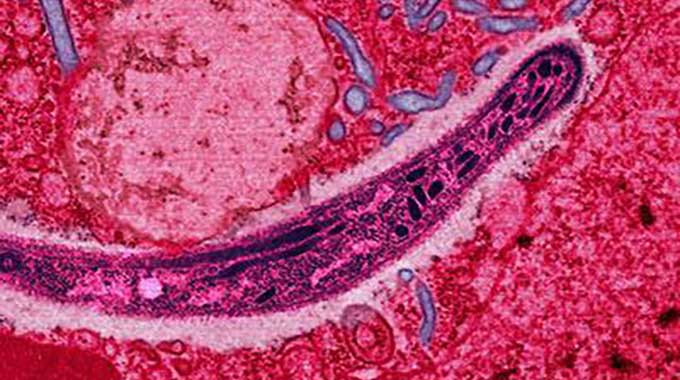
Image credits Ute Frevert, Margaret Shear / Wikimedia.
Such a treatment could be a boon for tourists, health care workers, or military personnel who travel to areas where malaria is common. Should the CIS43-based compound remain effective for up to six months at a time, it could be used to virtually eliminate the disease in malaria-endemic regions as part of a larger treatment plan, alongside antimalarial drugs.
Those questions, however, will need to be answered with future research. What we know so far is that CIS43 works by binding to a specific region of a key surface protein in the parasites. This region — called an epitope — only occurs once across the whole length of the protein, and is shared across 99.8% of all known P. falciparum strains. In other words, this is a chink in the parasite’s armor. Almost all the strains have it, which means they all need to have it for some task — and if we block that spot, we prevent the protein completely from performing that function.
Researchers at the NIAID Vaccine Research Center are now planning to assess how efficient and safe the use of CIS43 is in controlled, human malaria infection trials sometime next year.
The paper “A human monoclonal antibody prevents malaria infection by targeting a new site of vulnerability on the parasite” has been published in the journal Nature Medicine.
Was this helpful?



