Ketamine, a drug generally used for anesthesia, but also for recreational purposes, is now in the spotlight for its promising results in fighting depression. As shown in previous research, ketamine improves depression’s symptoms in a few hours, unlike the rest of anti-depressants, which may take weeks, even months to work. Scientists have now discovered exactly how ketamine so rapidly soothes depression.
“People have tried really hard to figure out why it’s working so fast, because understanding this could perhaps lead us to the core mechanism of depression,” says Hailan Hu, a neuroscientist at Zhejiang University School of Medicine in Hangzhou, China, and a senior author of the study.
The team believed that ketamine affected a small part of the brain, called the lateral habenula, also known as the “anti–reward center.”
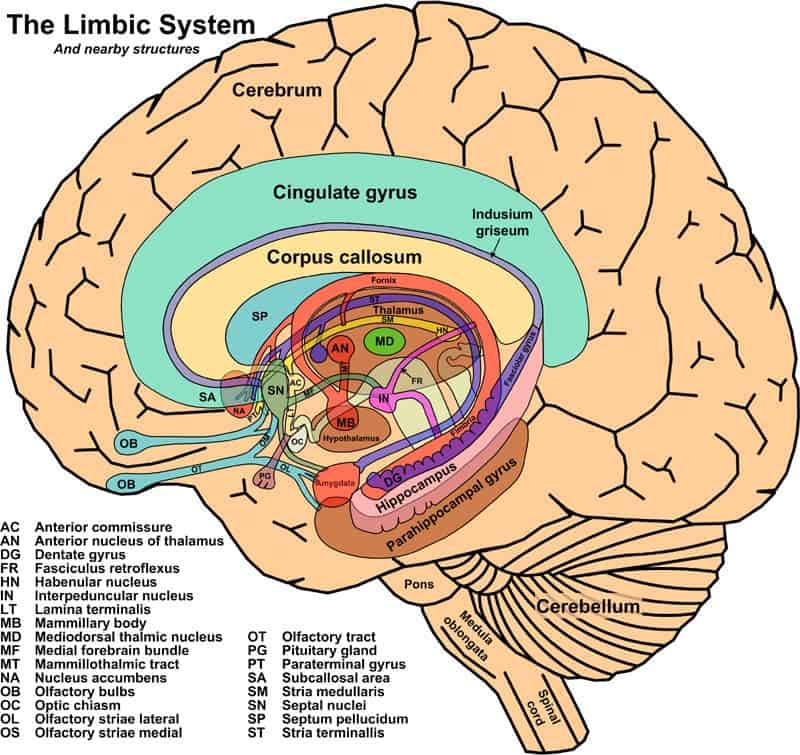
Via Wikipedia
Neurons from the lateral habenula are activated by stimuli associated with unpleasant events, like the absence of the reward or punishment, especially when these are unpredictable. To better understand how they work, here is an example: If a rat or a mouse solves a maze, it will expect some form of reward. If the rodent doesn’t get any reward, even though it had successfully completed a task, the neurons from the lateral habenula will fire, thus inhibiting the activity of the reward areas. Researchers believe that these ‘reward-negative’ neurons in the brain are overreactive in depression.
To see if their hypothesis was right, researchers designed an experiment in which they directly infused the drug into the lateral habenula of rats with depression-like symptoms. Scientists discovered that the pattern of neuronal activity, not the overall activity of the lateral habenula was a key factor in triggering depression: a percentage of the neurons in the lateral habenula fire several times in quick bursts, rather than firing once at regular intervals.
These bursts of activity in rats with symptoms of depression are absent in healthy rodents. An analysis of brain slices of healthy rats showed that they only had about 7% of these bursting type of neurons, in comparison to the depressed rodents that had almost 23% bursting neurons.
Scientists found similar results when recording the brain activity of mice: The animals who suffered stressful events had more bursting cells in the lateral habenula. After using optogenetics — a technique that allows cells to be ‘turned on or off’ with the help of light — the mice became more depressed, refusing to swim in a container of water even if forced.
But after the mice and rats were given ketamine, the number of bursting neurons became similar to the one found in healthy animals. Even when the scientists directed the neurons to fire in bursts, animals that had been administered ketamine no longer exhibited symptoms of depression.
“Anything that can block the bursting … should be a potential target based on our model,” Hu says.
In an accompanying study published at the same time in the journal Nature, the team found a protein synthesized by astrocytes (another type of brain cell that interacts closely with neurons) could be one of these targets. This molecule controls the flow of ions between a cell and its environment and it is involved in the process of resetting the nerve cell after an electrical signal, which requires regathering all the ions that flowed out of the cell during the signal.
The protein identified by the research team changes the amount of potassium available to the nerve cell, altering the cell’s ability to fire again soon. By increasing the amount of this protein, researchers were able to induce depression-like symptoms in mice.
The paper published in the journal Nature truly casts light upon the exceptional anti-depressant mechanism of ketamine, also providing us with important insight into further understanding the pathology of depression.
Was this helpful?



