The new study could revolutionize how we treat cancer.
“It has recently become apparent that the immune system can cure cancer,” the study starts off. Indeed, the body often has tools to fight cancer, but sometimes, it needs to be ‘told’ how to do so. A new study by Stanford researchers reports that injecting minute amounts of two immune-stimulating agents directly into solid tumors does exactly that. It basically removes all traces of cancer — even in distant, unrelated tumors. Basically, they’ve developed a cancer vaccine that wipes away all tumors from the body.
“When we use these two agents together, we see the elimination of tumors all over the body,” said Ronald Levy, MD, professor of oncology. “This approach bypasses the need to identify tumor-specific immune targets and doesn’t require wholesale activation of the immune system or customization of a patient’s immune cells.”
While both agents have been used in clinical trials, it’s the combination of the two that seems to be extremely effective. Furthermore, one of them has already been approved for human use, while the other has been used in several unrelated studies, without posing any major health risks.
The key lies in stimulating cancer-specific T cells (a particular type of lymphocytes). The first agent is a short stretch of DNA called a CpG oligonucleotide. CpG oligonucleotides elicit a strong response from T cells and have been successfully used as vaccine adjuvants. The other agent is an antibody that activates the T cells and instructs them to lead off the charge against the cancer cells. Because the vaccine is applied directly into the tumor, only T cells inside the tumor are affected.
“This is a very targeted approach,” Levy said. “Only the tumor that shares the protein targets displayed by the treated site is affected. We’re attacking specific targets without having to identify exactly what proteins the T cells are recognizing.”
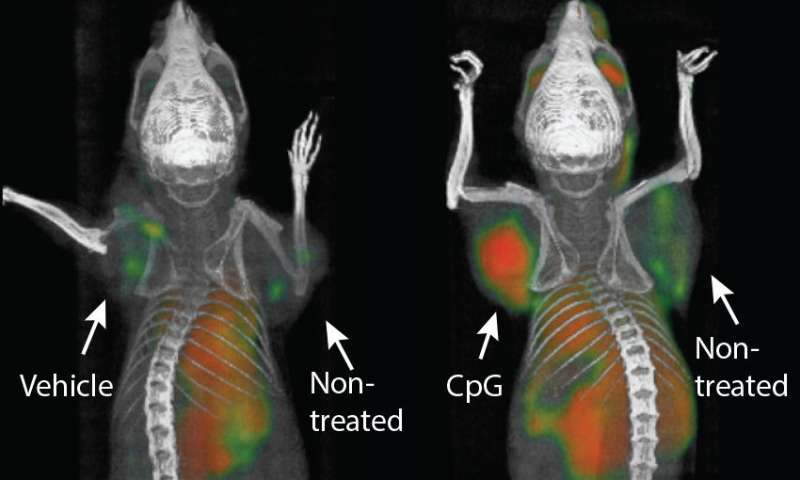
It’s not the first time researchers have tried to boost the body’s immune system to fight off cancer — on the contrary, several approaches have been trialed, with varying levels of success. For instance, some teams have targeted strategic checkpoints that limit the anti-cancer activity of immune cells, while others have genetically modified the body’s immune cells to defeat cancer. However, these approaches have significant drawbacks and are often extremely expensive and time-consuming. The method developed by Levy and his colleagues is only a one-time shot and seems to have no major drawbacks, while being extremely effective.
“All of these immunotherapy advances are changing medical practice,” Levy said. “Our approach uses a one-time application of very small amounts of two agents to stimulate the immune cells only within the tumor itself. In the mice, we saw amazing, bodywide effects, including the elimination of tumors all over the animal.”
Of course, just because this vaccine was successful on rats doesn’t mean it will be successful in humans. A review of studies has shown that 90% of drugs tested in rat studies fail in the human trials. But there are reasons to be optimistic.

For starters, even a 10% chance of developing a cancer vaccine seems pretty worthwhile given the lack of alternatives. Secondly, both the two agents have proven quite effective in humans, it seems quite likely that together, they will have a similar effect to what was observed in rats. Furthermore, because they are both safe to use, a human clinical trial is set to start soon, without significant delays. The clinical trial is expected to recruit about 15 patients with low-grade lymphoma. If successful, it could usher a whole new age of cancer treatment.
Levy envisions a world where this approach is used widely either as a single treatment or before surgically removing a tumor, to prevent the spread of lingering cancer cells.
“I don’t think there’s a limit to the type of tumor we could potentially treat, as long as it has been infiltrated by the immune system,” Levy said.
Journal Reference: Idit Sagiv-Barfi et al. Eradication of spontaneous malignancy by local immunotherapy. DOI: 10.1126/scitranslmed.aan4488.






