Researchers have developed a novel device that can detect if a lung cancer patient is likely to respond to immunotherapy with 85% accuracy. The procedure is non-invasive and only takes a few minutes to give the result, unlike standard procedures that require a biopsy and may take weeks.
Patients who have been diagnosed with non-small-cell-lung cancer (NSCLC) typically have to go through another stage of diagnosis in order to find the best treatment. Immunotherapy is one option, but it only works in roughly a fifth of all patients.
Immunotherapy boosts the body’s natural defenses to fight cancer by employing substances made by the body or in a laboratory to improve or restore immune system function. Immunotherapy drugs may work when other treatments don’t or they can boost other cancer treatments. However, there are also downsides.
Side effects may include flu-like symptoms, including fever, chills, and fatigue. Other types of immunotherapy can cause swelling, weight gain from extra fluids, heart palpitations, a stuffy head, and diarrhea. In about 10% of patients undergoing immunotherapy, organs such as the liver, lungs, and bowel can become inflamed because the body’s immune system starts to attack its own cells.
In order to determine whether immunotherapy is the right treatment for a patient with advanced NSCLC, doctors have to take a sample from the lungs and then analyze them in the lab. The procedure is very invasive and can take weeks for results to come back.
Michel van den Heuvel, a professor of thoracic oncology at the Radboud University Medical Centre in the Netherlands, along with colleagues, developed a small device that contains sensors capable of detecting volatile organic compounds found in the breath of patients with NSCLC.
The device, called eNose, is meant to indicate whether or not the patient will respond to anti-PD1 immunotherapy.
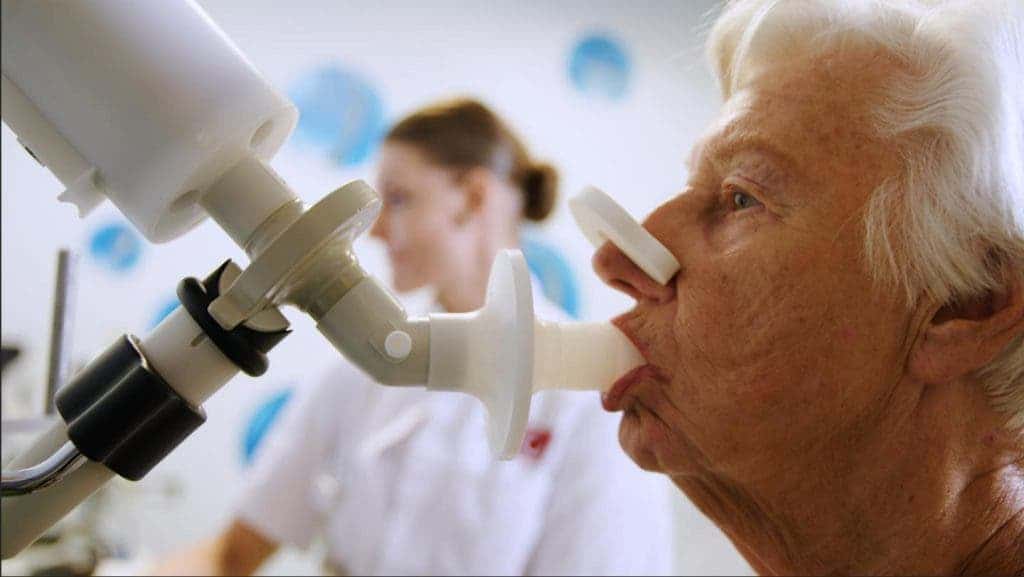
“When using the eNose, the patient takes a deep breath, holds it for five seconds and then slowly exhales into the device. The eNose sensors respond to the complete mixture of VOCs in the exhaled breath; each sensor has its highest sensitivity to a different group of molecules. The sensor readings are sent directly to and stored at an online server for real-time processing of the data and for ambient air correction because the air that you exhale is influenced by the air that you inhale. The measurement takes less than a minute, and the results are compared to an online database where machine-learning algorithms immediately identify whether or not the patient is likely to respond to anti-PD1 therapy,” expained Rianne de Vries, a PhD student at Amsterdam University Medical Centres and chief operating officer of Breathomix, a spinoff that is currently producing eNose.
The researchers performed a clinical trial involving 143 patients with advanced NSCLC at the Netherlands Cancer Institute. They used eNose to record the breath profile of the patients two weeks before immunotherapy. Three months later they used a standard assessment procedure to determine whether the patients responded to the therapy or not. The results were then compared to eNose’s predictions.
“We found that before the start of treatment with immunotherapy, the eNose analysis of exhaled breath from the patients with non-small cell lung cancer could distinguish between responders and non-responders with an accuracy of 85%,” said Dr. Mirte Muller, first author of the new study published in the Annals of Oncology.
The study found that 24% of the patients did not respond to immunotherapy. “This means that in 24% of NSCLC patients this treatment could be avoided, without denying anyone effective treatment,” Muller added.
This evaluation was conducted in a clinical setting and, as such, does not capture the full scope of a larger-scale lab trial. However, these promising results lay the foundation of new trials in the future.
“We are convinced that this study merely scratches the surface. It represents the first introduction of modern precision medicine, namely that molecular fingerprints can be easily obtained and quickly analysed on the spot. This truly offers new possibilities for the individual patient and the doctor. The power of this eNose system is that it has been properly validated, both technically and clinically, which is essential. We believe that analysis of exhaled breath is going to become an important diagnostic tool and will guide future treatment in oncology as well as in many other diseases,” Prof. van den Heuvel concluded.
As for detecting cancer itself, we’ve got that covered — thanks to man’s best friend. One 2011 study found dogs can identify breast and lung cancer with a 95% accuracy compared to a biopsy. UK doctors working at the Milton Keynes hospital found canines are 93% effective at sniffing prostate cancer. Researchers are working to emulate the canine sniffer is electronic devices.



