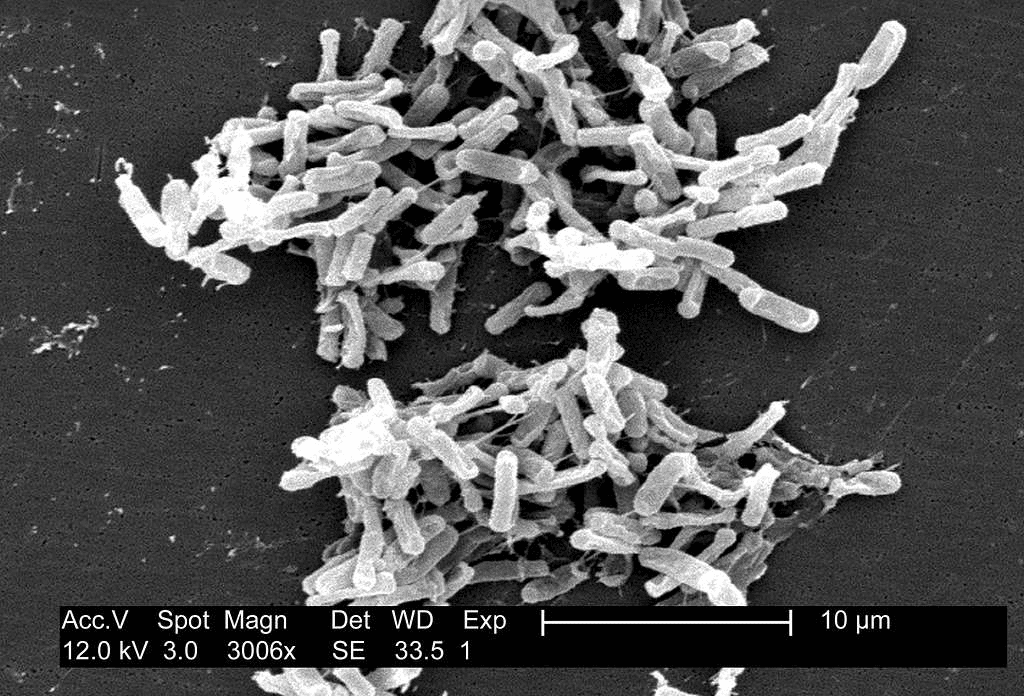
Treating infections of C. difficile is, as the name suggests, difficult. The most common treatment is antibiotics, but the virus is resilient and the infection often returns to patients. In some cases, it can even be fatal because we don’t have any good treatments. But we actually do have good treatments, a study claims.
“Our new study shows that we can effectively cure the infection through the early use of fecal microbiota transplantation (FMT) after completing the standard treatment, to prevent relapses,” he says.
The study was conducted in Denmark, a country of under 6 million people, where every year, over 2,500 people are affected by the infection. In the United States, half a million people are infected a year, and 29,000 are killed by the virus. Having a way to deal with this problematic infection, and a cheap one at that, would be a great advantage.
Pooping to victory
It’s not the first time fecal microbiota treatment (FMT) has been suggested as a potential solution for this type of infection and for other conditions as well. In fact, poop transplants have been found to be effective against everything from gut infections to brain problems. But initially, the method was regarded more as a fringe, unusual treatment — but things are changing.
In the new study, researchers led by Simon Mark Dahl Baunwall, a Ph.D. student at the Department of Clinical Medicine and a doctor at Aarhus University Hospital, recruited 42 participants. Of these, 21 participants were given FMT treatment, whereas the other 21 were given an antibiotic treatment or placebo.
“We found that treatment with FMT after completing the standard treatment cured 19 out of 21 patients, whereas only seven out of 21 treated with a placebo or another antibiotic were cured. In other words, the probability of curing the infection is three times greater after treatment with FMT than with our current standard treatment alone,” explains Baunwall.
In fact, the treatment was found to be so effective that the study had to be stopped for ethical reasons: there’s no way you could give someone a placebo or an antibiotic treatment in good faith when you’re seeing that another treatment works so much better.
“In rare cases, it can happen that you discover that the treatment you are investigating is so effective that it is ethically indefensible to continue,” says Baunwall. “Our study is one example, in that the new FMT treatment is so much better than the standard treatment with antibiotics that it would be unethical to continue, because the patients in the control group would risk not receiving the FMT treatment.”
The procedure is fairly straightforward. It relies on the idea that people suffering from this type of infection have an imbalance in their gut microbiota. So by transplanting feces from healthy donors, this imbalance can be fixed and in turn, can help fight the infection.
There are indications that the treatment could also be useful for a range of other conditions.
“At the moment, many studies of FMT treatment for various diseases are being carried out worldwide, with the most promising of these indicating beneficial effects in patients with inflammatory bowel disease and multi-resistant bacteria,” says Simon Mark Dahl Baunwall.
However, despite the treatment being confirmed now as a solution by several studies, it’s not deployed nearly as often as it should. In Denmark, the European country probably most advanced in this treatment, just 1 in 4 patients who could benefit from this treatment are given it. In Europe, the figure is 1 in 10 — and in other places, it’s even lower. Australia seems to be the place where the approach is most popular, and positive results are showing. It’s a promising method, and we’d be wise to pay more attention to it.
The study was published in The Lancet.
Was this helpful?



