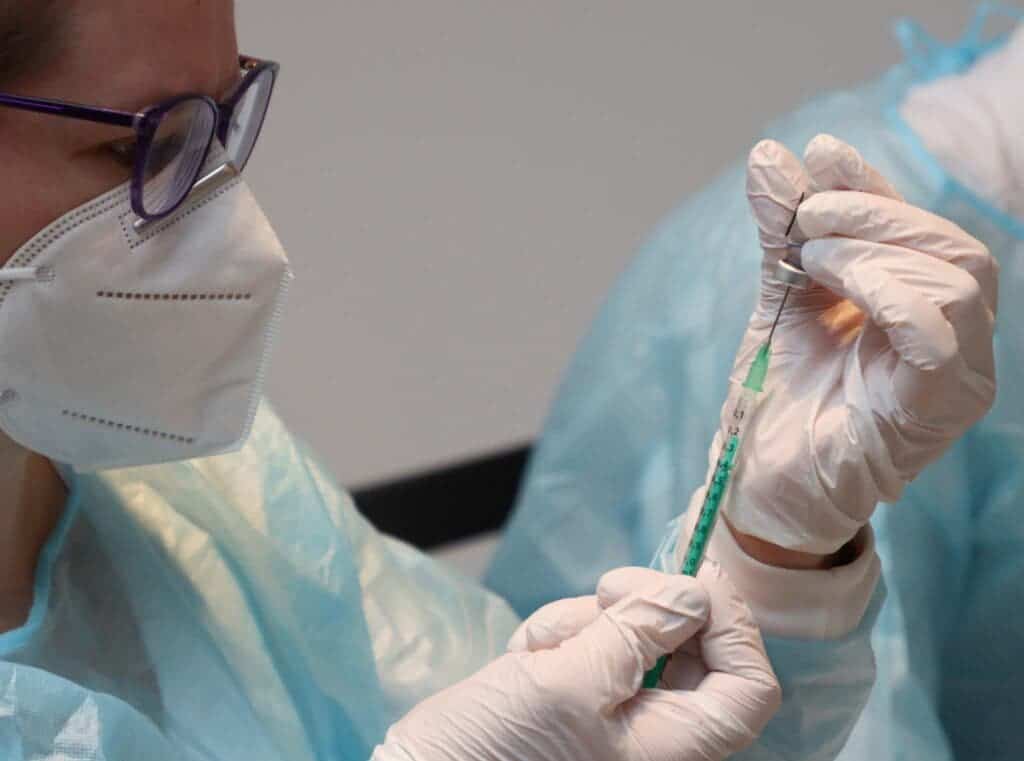
Every year there’s a new vaccine, which means you need to have an annual shot if you want to stay protected. That’s a pretty major inconvenience, especially for people who are anxious about needles or are vaccine-hesitant in general. That’s simply a fact of life at this point because the influenza virus mutates very rapidly, constantly changing the outer structure of its protein coat, at which point we need a new vaccine.
However, virologists from the prestigious Icahn School of Medicine at Mount Sinai in New York and the University of Pennsylvania think they could significantly extend the shelf life of flu shots by years. Using the same mRNA technology that went into the COVID-19 vaccines, the researchers created an mRNA-based cocktail that encodes four major influenza proteins that tend to remain the same and tested it on mice, with positive results.
Closer to a one-shot universal flu vaccine
One of the most used vaccines in the world is the measles, mumps, and rubella (MMR) vaccine, which we virtually all got as a child starting at the age of 12 to 15 months. Nowadays, this vaccine is delivered in two doses, after which it provides almost 100% protection for life. This is an ideal vaccine because measles is a highly stable virus that is unlikely to replicate. Smallpox and polio, highly contagious viruses that were almost eradicated through vaccination, are also stable with low mutation rates. On the flip side, however, viruses that mutate relatively frequently will eventually adapt to escape vaccine-induced immunity, so people need to get a new shot.
This is why we’re advised to get a new tetanus shot every ten years, but also why viruses that replicate extremely fast and mutate a lot, like flu-causing influenza, pose a major challenge to vaccine makers. Last year’s flu vaccine offered protection against four different strains that were in circulation, but this flu season there will be new ones. And because flu vaccines don’t exactly match the rapidly evolving influenza viruses, their effectiveness can vary wildly. For instance, in the U.S., flu vaccine effectiveness ranged from a lot of 19% to a high of 60% from 2009 to 2019.
Modern flu vaccines contain harmless parts of four strains of the influenza virus (an influenza A (H1N1) virus, an influenza A (H3N2) virus, and two influenza B viruses), not the whole virus. When you are given the flu jab, your immune system reacts to the parts, makes cells, and special proteins called antibodies that will protect you against the flu. Because the vaccines are made from the inactivated virus in egg cultures, these particles have lost their ability to cause disease. Some flu shots do contain a live, albeit weakened virus, such as those used in the nasal spray vaccine.
The antibodies produced by the vaccine target the head of the hemagglutinin (HA) protein of the influenza virus, keeping it from replicating and making you sick. The problem is that the virus changes the structure of hemagglutinin every season, thereby escaping protective immunity. But what if we make vaccines that target proteins that change less during the mutation process?
That’s what the new study set out to do. Researchers led by, Norbert Pardi, an assistant professor of microbiology at the University of Pennsylvania Perelman School of Medicine, and Florian Krammer, a virologist at the Icahn School of Medicine at Mount Sinai, applied the same strategies that led to the creation of the COVID vaccines and designed an mRNA influenza vaccine that targets four proteins that tend to change little across viral strains.
In mRNA vaccines, rather than a weakened virus or fragments of it, the payload consists of harmless molecules, including messenger RNA containing bits of genetic code that instructs cells in our bodies to produce certain proteins, which ramp up the immune system to offer protection when the real viral threat featuring the same proteins is encountered. The genetic code makes no changes to DNA (that’s actually impossible with current technology), so there are no permanent changes.
For their new vaccine, the researchers used multiple bits of code that cause the body to express antigens for matrix protein 2, the stalk part of hemagglutinin, nucleoprotein, and neuraminidase. They then tested this vaccine on 20 mice that were never infected with influenza prior to this experiment. The rodents were administered various combinations of the new vaccine. Some were injected with a vaccine for just one or two of the mRNA segments, for example, while others got all four. Also, some of these mice also got the vaccine more than once.
After the mice were exposed to an assortment of different flu strains, the researchers analyzed the blood samples from the rodents. All the new mRNA configurations elicited an immune response but it was only the quadrivalent vaccine that offered real protection from infection and flu symptoms. The researchers also found that some of the combinations, such as those that included nucleoprotein, led to an increase in the production of cytotoxic T cells, which play a major role in combating flu infections in both mice and humans.
“Taken together, our data demonstrate that the mRNA-LNP quadrivalent group 2 influenza virus vaccine is a promising vaccine candidate that targets diverse influenza virus strains,” the authors concluded.
Hopefully, clinical trials with people may start soon — although in this field ‘soon’ typically means in a couple of years. In the meantime, I guess we’ll just have to take that flu shot every year. ‘Tis the season, after all.
The findings appeared in the journal Proceedings of the National Academy of Sciences.
Was this helpful?



