The bad news? COVID-19 can be transmitted through poop. The good news? We can use that to our advantage and track the outbreak. The caveat? The science is somewhat debated.
Prior research has shown that when people are infected with SARS-CoV-2, it shows up in their stool samples. Recent research has even confirmed that these are active, infectious viral pieces. So poop can, at least in theory, be capable of passing the disease (at least in people suffering from a severe infection). But this is unlikely to make a significant difference in the grand scheme of things, at least not directly.
Poop is, thankfully, not an important means of transmission for this particular virus, but it could be a way to monitor it. Several teams have already pointed out that sewage water might be a useful and non-invasive tool to track COVID-19 spread in a community and detect clusters.
The downside of it is pretty obvious: you don’t know who has the disease, or exactly how many people have it, but it’s still very useful: you follow the amount of virus in the water, and when you see a sudden rise, you might be alerted of an emerging infection cluster.
Having an alert system could be of great help — and poop could be that alert system.

Here’s a common scenario: the government is looking at ways to relax the pandemic lockdown. At the same time, it is vital to make sure that the number of COVID-19 cases doesn’t spiral out of control. But there’s a catch: there’s a lag between when people contract the disease and when they start manifesting the disease. If you wait for people to start developing symptoms, you may already be too late to nip the outbreak in the bud.
What we flush down ultimately ends up in the sewage system, and that includes viruses. The idea is not new. Sewage water can tell us a lot of things about the community, from how rich people are to what type of diseases the community has.
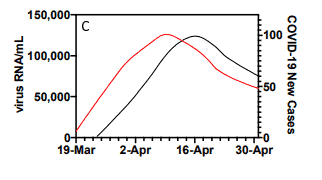
Several research groups have already shown data suggesting that sewage water could be used for this purpose, and a new study at Yale backs that idea up. The study, which features the chart at the top of the article, has stirred a lot of debate.
Unlike other studies, this study utilized primary sewage sludge instead of raw wastewater for virus RNA measurements (sewage sludge being comprised of solids that are removed during primary sedimentation steps and typically gravity thickened). Sludge was preferred because it tends to have a higher concentration of viruses, which makes it easier to detect the trends.
While the study only analyzed data from one plant (and the researchers caution that there may be significant differences in different plants), the results are very encouraging, suggesting that sewage is indeed a good predictor of COVID-19 infections.
“Raw wastewater and sludge-based surveillance is particularly useful for low and middle-income countries where clinical testing capacity is limited,” the study concludes.
But there’s a caveat: the chart looks almost too good. In the real world, nothing is correlated this well, and even if sewage sludge can predict coronavirus infection, this is too perfect to be believed at face value.
So a couple of researchers took a look at the data behind the graph and found a few issues with it. Nick Brown, self-appointed data police cadet who often comments on statistics on Twitter analyzed the data from the study, and found that the original study authors did a bit of statistical trickery.
What the chart does is that it correlates the trend lines for smoothed data presented in the study. Let’s break it down in simpler terms. The data looks like this:
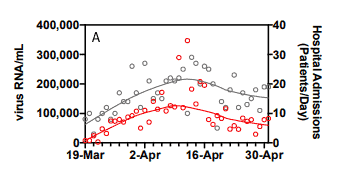
Scatter plots such as this one often deploy a trend line, which is basically a way to visualize the approximate trend followed by the data. This line itself is an approximation — as you can see above, it can’t correlate perfectly.
Then, this is smoothed, which is another approximation. Sure, the smoothed data trend-lines fit perfectly, but the real data doesn’t fit quite as smoothly. There’s still a correlation between the actual data (as was revealed by Brown and several other researchers commenting on the study, but it’s not nearly as spectacular. It’s still exciting and warrants further investigation, but the statistical artifice is unfortunate and disappointing.
The bottom line
This study has not yet been officially peer-reviewed (although unofficially, it was truly put to the gauntlet). Alexander Danvers published an excellent write-up of why researchers sometimes do this: there is a perverse incentive for researchers to publish as much as possible and as stand-out-y as possible. It’s almost certainly not ill-intent, but rather sloppiness, Danvers writes. The study is valuable and creative, and shows a plausible, cheap, and non-invasive way of predicting COVID-19 infections. With a bit more attention, we wouldn’t have spent the past few paragraphs diving into this whole issue.
“The key takeaway here isn’t that the Yale researchers who conducted the poop study are bad. The work is thoughtful and creative, and even being able to predict COVID-19 outbreaks with 15% accuracy is useful. The takeaway is that the behavior of scientists is governed by incentives, and these need to be better aligned with the production of high-quality science,” writes Danvers.
It’s definitely not perfect, and there is a lot of fine-tuning, but sewage water is still pretty much on the table when it comes to predicting outbreaks.
The loosening of restrictions has had mixed results, with some places continuing to see declining infection rates, while others reporting a dramatic rise in cases. While things like mandatory face masks and contact tracing are believed to play a role here, at this point, it’s impossible to say where the disease will make a resurgence and where it won’t. Having access to a cheap and non-invasive way to raise the alarm when COVID-19 cases are on the rise could make all the difference in the world.
We’d be crazy not to use this.






