The novel coronavirus causes a respiratory illness known as COVID-19. However, not all infected individuals experience the same symptoms. Some have mild symptoms, some progress to such severe pathologies that they require intubation on a mechanical ventilator to stay alive, and others still never experience any symptoms at all.
In other words, COVID-19 is actually a syndrome — a collection of symptoms — that manifests itself on a spectrum. Now, a new study suggests that those patients that go on to develop the most severe symptoms of COVID-19 pneumonia might fall into two distinct categories, each requiring different approaches to treatment.
The study is authored by intensive care Italian doctors affiliated with the Medical University of Göttingen, Turin Hospital, and the Health Centre for Human and Applied Physiological Sciences in London.
Writing in their commentary, the authors draw from their experience studying the disease as well as published studies of other researchers, concluding that COVID-19 pneumonia is a specific disease, which is distinct from acute respiratory distress syndrome (ARDS).
Some of the distinctive features of COVID-19 are severe hypoxemia (low levels of oxygen in the blood) associated with near-normal respiratory system compliance.
“This remarkable combination is almost never seen in severe ARDS. These severely hypoxemic patients despite sharing a single etiology (SARS-CoV-2) may present quite differently from one another: normally breathing (“silent” hypoxemia) or remarkably dyspneic; quite responsive to nitric oxide or not; deeply hypocapnic or normo/ hypercapnic; and either responsive to prone position or not. Therefore, the same disease actually presents itself with impressive non-uniformity,” the authors wrote in their study which is due to appear in the journal Intensive Care Medicine.
Based on observations of several cases, the authors propose two primary “phenotypes” that describe the time-related disease spectrum of emergency department cases of COVID-19.
These are “Type L”, which is characterized by low elastance, low ventilation to perfusion ratio, low lung weight, and low recruitability; and “Type H”, characterized by high elastance, high right-to-left shunt, high lung weight, and high recruitability.
In more detail, Type-L COVID-19 pneumonia has the following characteristics:
- Low elastance: the nearly normal compliance indicates that the amount of gas in the lung is nearly normal
- Low ventilation to perfusion (VA/Q) ratio: since the gas volume is nearly normal, hypoxemia may be best explained by the loss of regulation of perfusion and by loss of hypoxic vasoconstriction. Accordingly, at this stage, the pulmonary artery pressure, should be near normal.
- Low lung weight: Only ground-glass densities are present on CT scan, primarily located subpleurally and along the lung fissures. Consequently, lung weight is only moderately increased.
- Low lung recruitability: the amount of non-aerated tissue is very low, consequently the recruitability is low.
Whereas Type H has the following characteristics:
- High elastance: The decrease of gas volume due to increased edema accounts for the increased lung elastance.
- High right-to-left shunt: This is due to the fraction of cardiac output perfusing the non-aerated tissue which develops in the dependent lung regions due to the increased edema and superimposed pressure.
- High lung weight: Quantitative analysis of the CT scan shows a remarkable increase in lung weight (> 1.5 kg), on the order of magnitude of severe ARDS.
- High lung recruitability: The increased amount of non-aerated tissue is associated, as in severe ARDS, with increased recruitability.
Type L and Type H patients are best identified by CT scans.
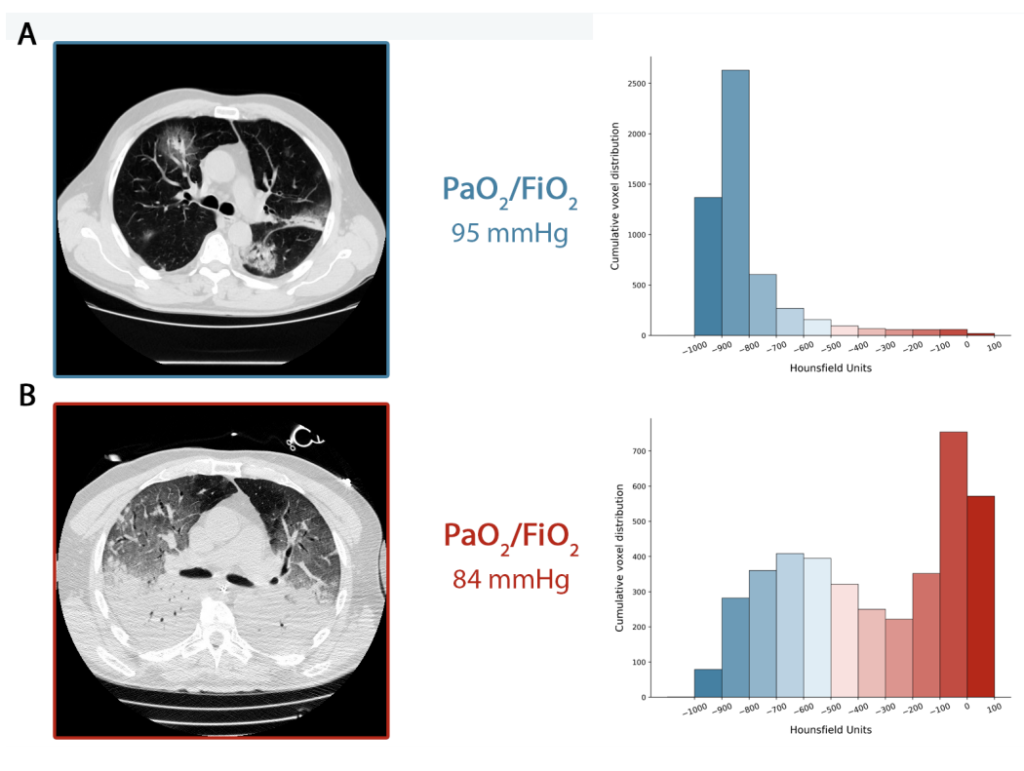
Given the differences in disease progression, it follows that the respiratory treatment offered to Type L and Type H patients must also be different.
Type L patients generally respond well to an increase in the initial fraction of inspired oxygen (FiO2). Patients can transition towards the Type H phenotype when the magnitude of inspiratory pleural pressure swings from 5-10 cmH2O to above 15 cmH2O — the risk of lung injury increases and intubation should be performed as soon as possible. Type H patients should be treated as severe ARDS, the authors concluded.
Was this helpful?



