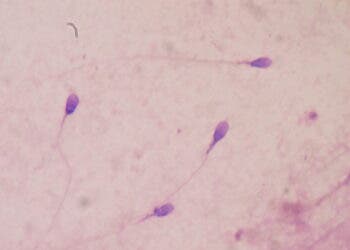
XYY syndrome is one of the most usual causes that renders some men unable to father children. About one in 500 boys are born with either an extra X or Y chromosome giving a total of 47 chromosomes instead of the usual 46. Often symptoms may be subtle and many people do not realize they are affected, but one common consequence is sterility.
This doesn’t necessarily mean that such men can’t pass on their genes to offspring, in this day and age. British researchers at the London’s Francis Crick Institute showed that it’s possible to create sperm in the lab starting from small pieces of connective tissue taken from the ears of infertile male mice.

Back to the cellular roots
For cells to differentiate into tissue that would eventually become skin, neurons, or that clump to form the liver or heart, they first start from stem cells. Today, however, it’s possible to go through the reverse process — turning tissue cells into undifferentiated ones called induced pluripotent stem cells (iPS). This enables the development of an unlimited source of any type of human cell needed for therapeutic purposes.
This is truly a very powerful method and in the 10 years since Nobel Prize-winner Dr. Shinya Yamanaka discovered IPSCs, regenerative medicine and drug discovery-development have accelerated their use of these cells. IPS cells can be used, for instance, to grow new organs in the lab that are an exact biological fit for any donor.
Diseases such as Alzheimer’s, Parkinson’s, Huntington’s and Down’s syndrome now have models that forego the use of ethically controversial ECSs. For drug screening and development, IPSCs are in use for in-vitro studies since these cells are capable of immortal growth in culture and provide genuine, human testable models. New drugs can be screened against cell culture models to determine their safety and efficacy, thanks to IPSCs.
From ear tissue to sperm…
In our case, the researchers transformed fibroblast connective tissue cells collected from sterile male mice into stem cells. In the process, the extra chromosome disappeared. The stem cells were then coaxed to differentiate or develop into immature sperm cells.
When these cells were injected into the testis of mice, they became properly functioning and healthy sperm. And ultimately, it was this sperm that was used to fertilize eggs, leading to healthy offspring.
Theoretically, it should be possible to translate the findings to men that have three sex chromosomes. The researchers went a step further into proving this by showing that they could make stem cells from XYY men’s fibroblasts which lacked the extra chromosome.
“The findings have relevance to overcoming infertility and other trisomic phenotypes,” the authors wrote in their paper.
The only huge drawback that would prevent a clinical trial is safety. Some of the mice that were injected with the immature sperm developed tumors and right now there is no way to make viable sperm outside the body, though that may change.
In any event, these are very encouraging results. If the scientists can find a way to vastly reduce the risk of tumor or can develop a method that can render healthy sperm in a lab tube, many men would be grateful. Like most things in experimental medicine, however, it might take another decade before this happens.
The findings were reported in the journal Science.