An experimental therapy using bacteriophages (viruses of bacteria) successfully cured a patient of a multi-drug resistant bacterial infection. No antibiotic, no matter how strong, could help the patient who had been in a coma for two years. The findings suggest that personalized phage therapy can be very successful and will likely propel more research groups to devote more resources for such life-saving initiatives. The World Health Organization estimates that by 2050, 50 million people will die because of antibiotic-resistant infections. No new class of antibiotics has been discovered in the last three decades.
When bacteria resist
In late 2015, Tom Petterson, a 69-year-old professor in the Department of Psychiatry at UC San Diego School of Medicine, was vacationing with his wife in Egypt when he suddenly became ill. Local doctors quickly diagnosed him with pancreatitis, an inflammation of the pancreas, and when standard care failed he was urgently flown to Frankfurt, Germany. There, doctors found he had been infected with a multidrug-resistant strain of Acinetobacter baumannii.
The German doctors also discovered a pancreatic pseudocyst which causes fluid to build up around the pancreas. Antibiotics seemed to fail. The only thing that worked was a drug of last resort — a mix of meropenem, tigecycline, and colistin, which is known to cause kidney damage among its many side effects. The situation warranted this extreme measure, though, and once his condition became stable enough, Patterson was flown to the Thornton Hospital at UC San Diego Health. Here disaster waited. The doctors found that upon arrival the bacteria had become resistant to all antibiotics.
To make matters worse, as Patterson was prepared for transfer to a long-term acute care facility, an internal drain slipped, spilling bacteria into his abdomen and bloodstream. The patient immediately entered in septic shock and soon after fell into a coma. He would stay in a coma for the next two months. His days were numbered but family and colleagues at the university didn’t stay idle.
“There came a point when he was getting weaker and weaker, and I didn’t want to lose him. I wasn’t ready to let him go and so I held his hand and said, ‘Honey, they’re doing everything they can and there’s nothing that can kill this bug, so if you want to fight, you need to fight. Do you want me to find some alternative therapies? We can leave no stone unturned,'” the patient’s wife, Steffanie Strathdee, recalled. Strathdee is the chief of the Division of Global Public Health in the Department of Medicine at UC San Diego and no stranger to crippling diseases.
Two can play this game: infecting bacteria
Strathdee read everything she got her hands on. While researching, she was informed about a case from Tblisi, Georgia where a patient suffering from a ‘difficult’ infection was ‘miraculously cured’ after undergoing phage therapy.
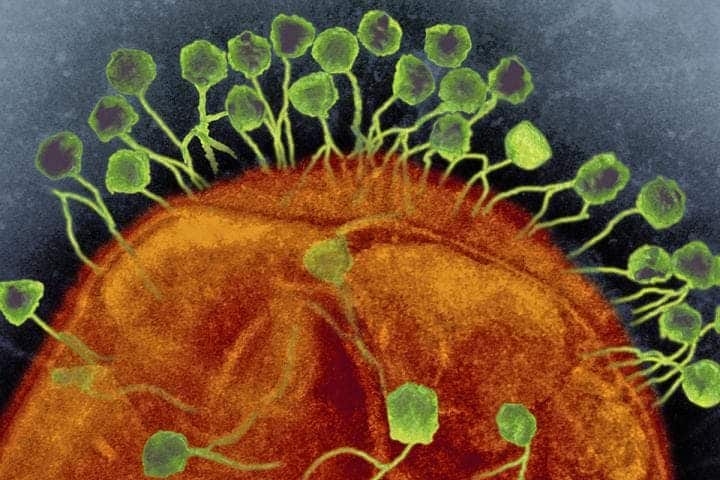
Bacteriophages are viruses, and the most numerous kind to boot. By some estimates, there are 1031 bacteriophages on the planet or more than every other organism on Earth combined. That includes bacteria. If bacteria infects humans, bacteriophages infect the bacteria. These phages cause a trillion trillion successful infections per second and destroy up to 40 percent of all bacterial cells in the ocean every day.
Bacteriophages were formally discovered in the mid to late teens of the 20th century, with the first publication coming out in 1915. In the 1920s and the 1930s, phage therapy was commonly used to treat various bacterial infections but as antibiotics became more widespread and easy to use, phage therapy turned into a simple mention in medical textbooks. Some parts of Eastern Europe and the Soviet Union were still involved with phage therapy research, it’s worth adding.
More than a hundred years since phage therapy was described, the joke’s on us. Countless strains of bacteria are becoming resistant to antibiotics. Common STDs like gonorrhea will become untreatable in the next decade by some accounts, and mortality because of multi-drug bacterial infections will become widespread. Already, hundreds of thousands of people around the world die from hospital-acquired multi-drug resistant bacteria and the World Health Organization estimates antimicrobial resistance will kill at least 50 million people per year by 2050.
Though obscure, Strathdee managed to come across people who were working with phage therapy. They found three team with phages that could target Patterson’s specific infection: the Biological Defense Research Directorate of the NMRC in Frederick, MD; the Center for Phage Technology at Texas A&M University; and AmpliPhi, a San Diego-based biotech company specializing in bacteriophage-based therapies. All three agreed to help and the phage samples were sent to San Diego State University where they were purified. Meanwhile, emergency approval for the samples’ use was given by the Food and Drug Administration.
Against all odds
Patterson was given the phages through catheters into his abdominal cavity and intravenously so the therapy acted more broadly. Patterson’s condition began to improve and within three days since the first IV phage therapy, he had emerged from his long coma.
“As a treating doctor, it was a challenge,” said Chip Schooley, one of Strathdee’s colleagues. “Usually you know what the dosage should be, how often to treat. Improving vital signs is a good way to know that you’re progressing, but when you’re doing it for the first time, you don’t have anything to compare it to.
“A lot was really worked out as we went along, combining previous literature, our own intuition about how these phages would circulate and work and advice from people who had been thinking about this for a long time.”
Patterson described the experience as miraculous, though his body had been severely weakened after losing 100 pounds in coma, mostly muscle.
“The phage therapy has really been a miracle for me, and for what it might mean that millions of people who may be cured from multidrug-resistant infections in the future. It’s been sort of a privilege,” Patterson confessed.
Though the sample size of the study only measures one person, Patterson’s case study gives hope that personalized therapy with bacteriophages can undo possibly any infection where antibiotics don’t work. Most people around the world won’t have Patterson’s privilege of having friends and family who are among the best doctors in the world. It will be an immense challenge to translate this sort of therapy into something that’s as easy and cheap as antibiotics are today. Well, cheap and easy for now at least.



