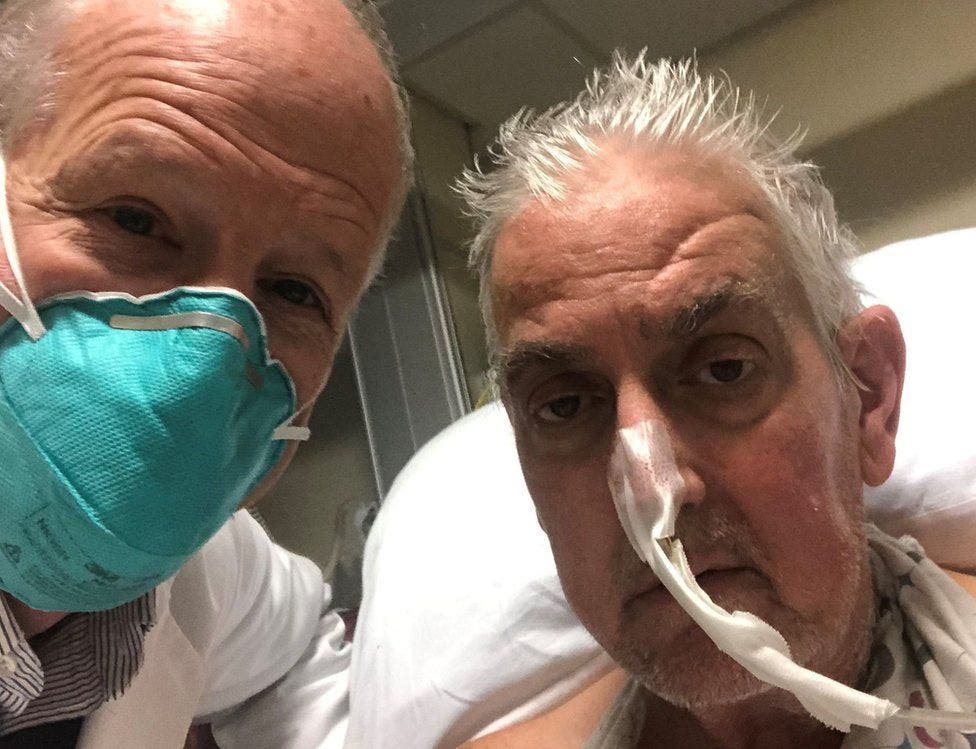
David Bennett, a 57-year-old American diagnosed with terminal heart disease, had spent the last six weeks bedridden attached to a machine that kept him alive. Due to this decaying condition, the man was not eligible for a heart transplant. It seems like there was no hope left, but the restriction only applied to human hearts. Mr. Bennett was given a second shot by doctors at the University of Maryland Medical Center who, during a grueling seven-hour surgery, replaced his failing heart with that of a genetically-modified pig. This is the first time the heart of a pig has been transplanted into a human, a procedure known as xenotransplantation.
A medical gamble
In the second half of 2021, surgeons at New York University Langone Health successfully grafted a pig kidney to a human. They actually did this twice. However, both patients were brain-dead and the kidneys from the ungulates were externally attached to the human body via a large blood vessel. By contrast, Mr. Bennett is conscious and could prove that xenotransplantation actually works in the real world.
Out of all mammals, a pig’s organs are the most compatible with those of humans in terms of size and metabolism. For many years, doctors have already been using pig valves in replacement surgeries. But even so, an untreated pig heart will be quickly and furiously rejected by the human body, which is why the animal used in the transplant had been genetically modified to knock out several genes that express molecules that humans do not. Biocompatibility can make or break a transplant and issues can appear even between organs sourced from humans, not to mention those belonging to an entirely different species.
The procedure was deemed a success. The transplanted heart is beating a pulse and drives pressure, but it is too quick to draw definite conclusions. The patient might live only a few extra days or weeks, but he could just as well live another year — such is the nature of experimental medical procedures on the terminally ill.
“It’s working and it looks normal. We are thrilled, but we don’t know what tomorrow will bring us. This has never been done before,” said Dr. Bartley Griffith, the director of the cardiac transplant program at the University of Maryland and one of the doctors who performed the procedure.
More than 100,000 Americans are on organ transplant waiting lists. Demand far exceeds supply, with thousands dying each year in the U.S. before they get their chance at a transplant. Although more Americans received a human donor heart in 2021 than ever before, there’s still an acute shortage of organ donors. In this context, xenotransplantation represents a silver lining.
Scientists hope that animal-to-human organ transplants will become one day become the norm, revolutionizing the way we treat organ failure. However, entering this door is not without its many challenges. Organ rejection regularly occurs even between seemingly well-matched human donors and recipients.
Mr. Bennett decided to choose this unproven procedure because he had no other options. Although his condition is currently stable, his prognosis is rife with uncertainty. He is still hooked up to machines that assist in breathing and heart functioning and is scheduled to be taken off these machines next week. During this time, the patient will be closely monitored, especially in the first 48 hours that are particularly critical.
“It was either die or do this transplant,” Mr. Bennett said before the surgery, according to officials at the University of Maryland Medical Center. “I want to live. I know it’s a shot in the dark, but it’s my last choice.”