As antibiotic-resistant pathogens encroach on our hospitals, one team is trying to strip MRSA of its defenses.
People don’t oft think about this, but the way we treat diseases and pathogens today wouldn’t have been just a luxury for people 100, 150 years ago — it would have been a straight-up miracle dripped from the heavens, day in, day out. We owe this ability — to casually swallow a teeny tiny white tablet and then walk away from deadly infections — to how effective modern antibiotics are at killing germs.
But said germs are evolving to become immune to these compounds — and once they do, they’ll come at us with a vengeance.
New rules of engagement
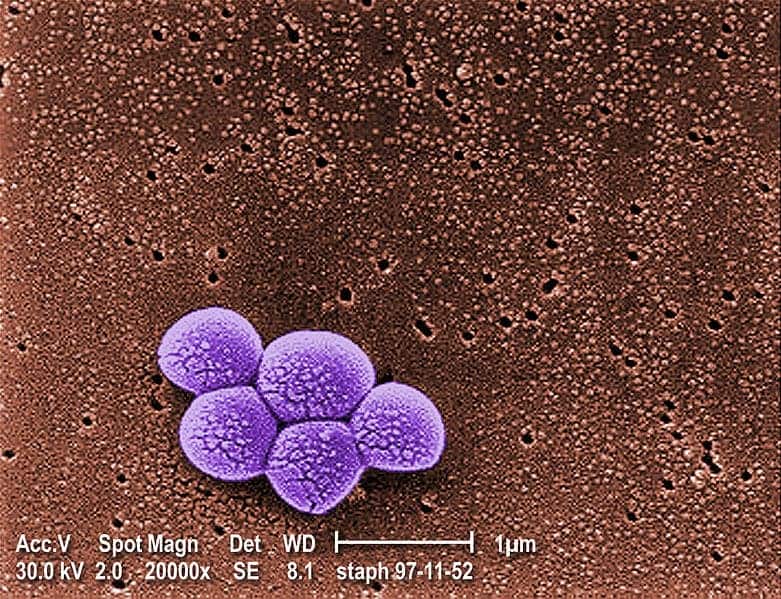
One of the best-known and most widely seen antibiotic resistant pathogen is known as MRSA — methicillin-resistant Staphylococcus aureus. This bacterium, which can easily turn routine medical operations into life-and-death battles, is responsible for most of the 30,000 deaths annually associated with antibiotic-resistant infections in the U.S. alone.
MRSA owes this infamous achievement to its resilience and, frankly, a kind of bacterial ingenuity that lets it shrug off should-be-deadly antibiotics. New research at the Michigan State University, however, is figuring out how to turn one of its strengths against it.
“Attacking the cell membrane and inhibiting its ability to produce lipids, or fats, could be an effective treatment protocol,” said senior author Neal Hammer, MSU assistant professor of microbiology and molecular genetics.
“MRSA, though, bypasses the effects of fatty acid inhibitors by absorbing human lipids.”
The study is based on previous research, which found that MRSA has a fat-absorbing pathway encoded in its genes. The problem with such a pathway is that most of our antibiotics work by destabilizing bacterial cell walls (made of fat molecules). MRSA’s adaptation to antibiotics is especially problematic since it doesn’t simply make our drugs somewhat less effective — it renders most of them completely pointless.
MRSA can absorb fat from the host organism, and then use it as a shield. In the case of us humans, it’s likely using fats (lipids) floating around in the bloodstream. These include compounds such as cholesterol that are a natural (and ample) component in our blood. The team suggests that MRSA can absorb and then integrate these substances into its own membranes. The process makes it virtually immune to antibiotics that work by blocking fatty acid synthesis pathways.
“MRSA secretes enzymes, called ‘lipases,’ that free the fatty acids in human LDLs, or bad cholesterol,” Hammer said. “We used mass spectrometry to identify how MRSA was able to perform this feat — the first time this process has been observed.”
Past research focused on MRSA’s interaction to fatty acids found on the skin — as much as 30% of the world’s population carry MRSA on their skin without any adverse health effects. The present study is the first to identify how MRSA can draw fatty acids from inside the host body and the mechanisms that allow it to do so.
Hammer says he and his team will focus their future research on how to prevent MRSA from drawing these fats from the ones it infects. If successful, the findings could make our antibiotics effective against staph yet again.
The paper “Staphylococcus aureus Utilizes Host-Derived Lipoprotein Particles as Sources of Fatty Acids” has been published in the Journal of Bacteriology.
Was this helpful?



