Without blood, the human body would simply stop working. This essential fluid of life dispenses crucial nutrients throughout the body, exchanges oxygen and carbon dioxide, and carries our immune system’s ‘militia’ to stave off infections. But not all blood is equal, and in the event of a transfusion, mixing incompatible blood types can lead to death.
The most common blood type in the world is type O. This blood type, which is characterized by the absence of certain antigens on the surface of red blood cells, is found in almost half of the global population.
Type O blood lacks the A and B antigens, which means that it can be transfused into people with any blood type without causing a reaction. This makes it the safest and most reliable option for blood transfusions and wound treatment, especially in emergency situations when the blood type of the recipient is unknown.
How many blood types are there?
There are 4 main blood groups: A, B, AB and O, of which group O is the most common. These blood types are determined by the presence or absence of certain proteins, called antigens, on the surface of red blood cells. The A and B antigens are sugars that are attached to proteins or lipids on the surface of red blood cells. The O blood type does not have either of these antigens. The AB blood type has both the A and B antigens.
The presence of an Rh factor (a protein on the surface of blood cells) adds a “positive,” while the absence of it adds a “negative” designation of the blood type. That leads us to the eight common blood types: positive, and negative versions of A, B, O, AB. In the United States, the average distribution of blood types is as follows:
- O-positive: 38 percent
- O-negative: 7 percent
- A-positive: 34 percent
- A-negative: 6 percent
- B-positive: 9 percent
- B-negative: 2 percent
- AB-positive: 3 percent
- AB-negative: 1 percent
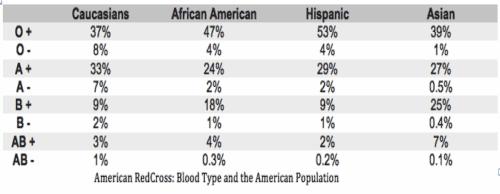
Different racial and ethnic groups typically see a different distribution. For instance, 45 percent of Caucasians are type O, but 51 percent of African-Americans and 57 percent of Hispanics are type O, according to the Red Cross. This Wikipedia page has the blood type distribution in every country.
Type O is the most demanded blood type in hospitals, both because it’s the most common and because O-negative blood is a universal donor type, meaning it is compatible with any blood type. Conversely, type AB-positive blood is called the universal recipient type because a person who has it can receive blood of any type.
How blood type is determined
Like eye color, blood type is genetically inherited from your parents. Whether your blood group is type A, B, AB or O is based on the blood types of your mother and father. For instance, if your mum is AB and your dad is A, you can expect to be A, B, or AB. If mum is AB and dad is O, the child will have an A or B blood type. When both parents are A, the child will have either O or A.

Blood is essentially made up of two types of blood cells (red and white), platelets, and a fluid called plasma. About half the blood (45%) is made up of blood cells, with the remaining 55% being plasma. Millions of blood cells are produced daily in the bone marrow, the soft spongy material that fills up bone cavities.
A person’s blood type is determined by proteins found on the surface of red blood cells called antigens. If antigen A is present in the red blood cells, then you have type A blood, while having B antigen present means you have type B blood. If both A and B are present, you have type AB blood. If neither antigen is present, you have type O blood.
The gene for type O is ‘recessive’, meaning if you have one gene for O and one for A, then you still end up with A antigens on your cell membranes, and the same goes for O and B. In order to be group O, you need both parent cells to be O. Why then is group O the most common? The simple reason is that it is the ancestral form. Except for more recent times, virtually all humans used to be type O. The A and B mutations appeared in the last 20,000 years and haven’t spread through the entire population yet. But at some point in the future, type O might actually become the least common.
Besides the ABO classification, there’s also another blood type grouping that involves Rhesus (Rh) factors. The name comes from the Rhesus monkeys, in which such proteins were first discovered. Rhesus factor D, which is the most important, is present in 85% of people, making them Rhesus-positive. The remaining 15% are grouped Rhesus-negative. The Rh grouping can be very important in some situations. For instance, a baby’s life can be endangered if it inherits a Rhesus-positive blood type from the father while the mother is Rhesus-negative — in such a situation, the mother can form antibodies against her own baby’s blood.
Blood groupings and transfusions
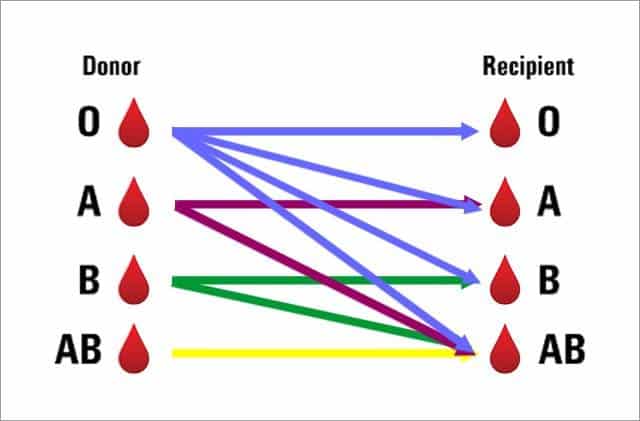
In order to safely perform a blood transfusion, it’s essential that a patient receives a blood type that is compatible with their own. For instance, if a person with Rh-negative blood receives a transfusion of Rh-positive blood, their immune system may recognize the donated blood cells as foreign and produce antibodies against them. This can lead to a condition called Rh incompatibility, which can cause serious complications such as anemia and kidney failure. If the blood type is incompatible, there’s the risk that the red blood cells will clump together, producing clots that block blood vessels and cause death. Generally, for the ABO grouping, blood transfusions follow these rules:
- A person with type A can donate to a person with type A or AB.
- A person with type B blood can donate to a person with type B or AB.
- A person with AB type blood can only donate to a person with AB. However, a person with blood type AB can receive blood from anyone, being the universal recipient.
- A person with O type blood can donate to anyone, being the universal donor. This is because type O blood has no antigen on the surface of its red blood cells. However, people with type O blood can only receive type O.
People with Rh-positive blood can receive either positive or negative donations but those who have Rh-negative blood can only receive Rh-negative blood.
Doctors will test your blood before you are allowed to donate or receive blood. However, in the event of an emergency when the patient’s blood type is unknown, type O-negative blood will be used.
It’s important to note that there are more than 600 other known antigens, the presence or absence of which can lead to “rare blood types.” The ABO grouping works just fine for most people, but in some rare cases, certain blood types may be unique to specific ethnic or racial groups. For instance, many patients with sickle cell disease require an African-American blood donation. That’s why it’s still ideal to match a blood donation type to its recipient exactly, accounting for both antigen types and Rh factors. A blood type is considered rare if a patient lacks antigens that 99% of the people are positive for. If you somehow lack an antigen that 99.99% are positive for, your blood type is extremely rare.
In conclusion, it is clear that the most common blood types are O+ and A+. These two types make up a significant portion of the global population, with O+ being the most prevalent. It is important for people to know their blood type, as it can have important implications for blood transfusions and organ transplants.