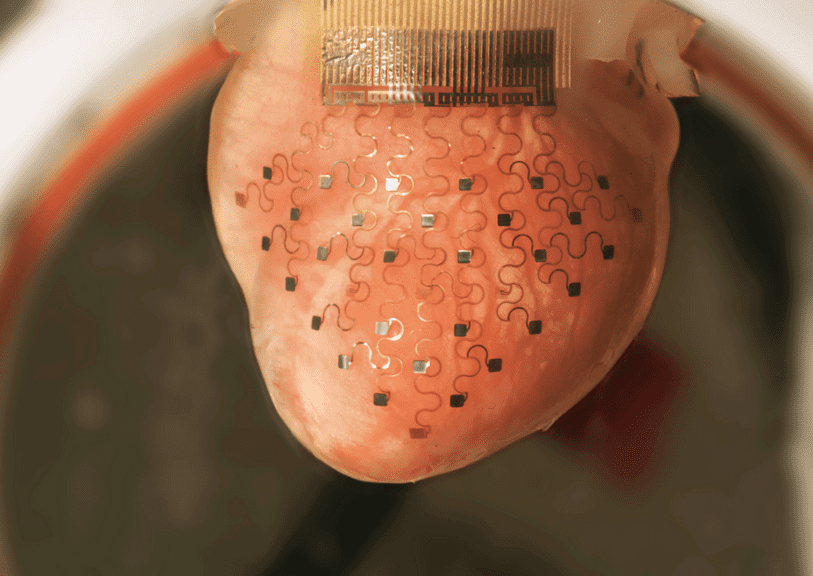
Exploiting both the latest in 3D printing and stretchable electronics, scientists at University of Illinois at Urbana-Champaign and Washington University in St. Louis have devised a new electronic membrane that could replace pacemakers. The membrane is designed to ‘cloth’ the heart and constantly delver electrical shocks to maintain a constant heart beat rate, avoiding arrhythmia and minimizing heart attack risks.
Similar ideas have been proposed since the early 1980s so genuinely, the concept isn’t entirely novel. However, these pioneering earlier models stood no chance at being practical, since the crude fabrics with bulky electronics sowed directly onto the membrane interfered directly with the heart and did more harm than good.
This new design is like a spider-web network of sensors and electrodes, all built-on a flexible membrane using 3-D printing. Because everything is custom designed according to the patient’s needs, it all fits like a glove. The real stroke of genius, however, lies in the use of stretchable electronics. John Rogers, a materials scientists from the University of Illinois, was responsible for this aspect and while the electronic components (sensors, electrodes ) themselves are made out of conventional rigid materials (like silicon), the circuits are laid out in curved, s-shaped design that allows them to stretch and bend without breaking.
“When it senses such a catastrophic event as a heart attack or arrhythmia, it can also apply a high definition therapy,” said biomedical engineer Igor Efimov of Washington University, who helped design and test the device.
“It can apply stimuli, electrical stimuli, from different locations on the device in an optimal fashion to stop this arrhythmia and prevent sudden cardiac death,” Efimov said.
The researchers liken the heart glove to the pericardium itself – the heart’s membrane – as the device senses and interacts with the heart in different ways that are relevant to clinical cardiology. A prototype membrane was fitted to a rabbit’s heart, keeping the organ operating perfectly “outside of the body in a nutrient and oxygen-rich solution”.
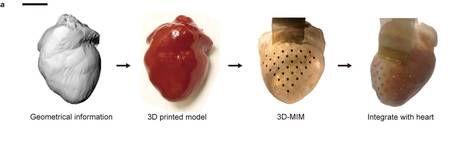
Impressive, by all means, but for the moment the device will remain a research tool. It’s still uncertain when this solution, either stand alone or integrated part of another system, would become available for heart treatments.
The research is published in the journal Nature Communications.






