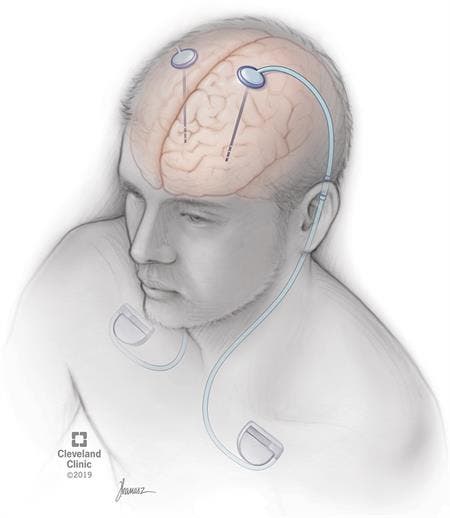
Schematic of deep brain stimulation, which involves implanting electrodes in the brain.
For some people diagnosed with depression, their condition is so severe that neither therapy nor drugs make a dent in it. Such was the case of Sarah, a 38-year-old patient, who agreed to undergo an experimental procedure that involved treating her depression using a brain implant that interrupts patterns of neural activity linked to the condition. It actually worked, putting a smile on Sarah’s face for the first time in five years.
Although the therapy involved a single patient, experts in the field have praised the study, pointing out that this form of personalized therapy may be the future — not just for treating depression but also a score of other psychiatric illnesses.
The success of the therapy also validates prior research, showing that certain patterns of brain activity underlie symptoms of mental illness and tweaking them towards a pattern seen in healthy people can improve the mental health of patients.
Katherine Scangos, an assistant professor of clinical psychiatry at the University of California, San Francisco (UCSF) and lead author of the new study describing the breakthrough psychiatric treatment, said the therapy “is an incredible advancement in our knowledge of the brain function that underlies mental illness.”
Before volunteering for the therapy, Sarah, a Northern California native, often had sudden bouts of crying. At the peak of her depression, she had to quit her job at a health tech company and moved in with her parents at the request of her doctor. She was on more than 20 different medications and spent months in the hospital. She had also tried various experimental techniques that previously worked on some hard cases like herself, including transcranial magnetic stimulation and electroconvulsive therapy. However, her symptoms didn’t improve.
But weeks later, scientists at the University of California, San Francisco surgically implanted a matchbook-sized device in her brain, Sarah’s persistent suicidal thoughts disappeared.
The device is calibrated specifically to Sarah’s brain activity. It detects neural patterns that occur when she is depressed then delivers pulses of electrical stimulation that rewire these patterns into a healthy state.
Sarah’s score on a standard depression scale was 33 in August 2020, before her surgery. A score between 20 and 27 reflects ‘severe’ depression. Two weeks after the “brain pacemaker” was successfully implanted, her scores quickly dropped to 14. A few months later she scored 10, the range where doctors consider a patient is in remission.
Previous deep brain stimulation implants for depression were found to produce no better improvements than a “sham” implant meant to induce a placebo effect. But, those implants were designed to be”one size fits all”, whereas the present implant is personalized to Sarah’s depression neural activity.
According to Scangos and colleagues, who presented their findings in the journal Nature Medicine, one person’s depression might look very different from another. Before they performed the surgery, the researchers spent ten days analyzing Sarah’s brain while she was interviewed about her feelings. They also applied stimulation to different locations in varying doses.
Using this training data, the deep brain stimulation was automated with the help of a machine learning algorithm after the implant was inserted in Sarah’s right brain hemisphere. The implant fires electrical impulses about 300 times each day with bursts lasting a couple of seconds. There is no obvious sensation when the implant is firing, aside from a feeling of alertness and positivity, Sarah said.
Electrodes were implanted in two key brain regions: the ventral striatum, which is involved in emotion, motivation, and reward, and the amygdala, primarily associated with emotional processes.
The implant hasn’t eliminated depression-causing activity in Sarah’s brain; it just corrects it. Furthermore, the patient is still taking psychiatric medication. Nevertheless, her condition has improved dramatically — a night and day difference. Even now, a year after her surgery, Sarah’s depresion is kept at bay.
Nearly a third of patients with depression don’t respond to standard treatment. Deep brain stimulation may be the therapy some of these patients have been waiting for to live a normal life. However, the invasive procedure and high cost (at least tens of thousands of dollars) will act as an entry barrier for many.
“Future work is required to determine if the results and approach of this n-of-1 study generalize to a broader population,” the scientists concluded in their paper’s abstract.
Was this helpful?



