A team at MIT in collaboration with the Riken Brain Science Institute in Japan activated the lost memories of mice. The findings suggest memory deficiencies like amnesia have more to do with accessing data, than storage itself. Though far from applicable to humans, the research does show that it’s possible, in theory at least, to help patients with retrograde amnesia (who’d lost their memories following a trauma or brain injury) live a normal life once more.
Shining light on lost memories

Among neuroscientists, the causes and roots of amnesia are still up for debate and the community seems to be split into two currents: those who believe it is caused by damaged brain cells (a storage problem), and those who hold that the memories themselves are blocked because of faulty connections (an accessing problem). These latest findings allude to the latter as being the leading factor of memory loss, though in practice it might actually be a combination of the two.
“The majority of researchers have favored the storage theory, but we have shown in this paper that this majority theory is probably wrong. Amnesia is a problem of retrieval impairment,” said Nobel-awarded Sususmu Tonegawa, director of the RIKEN Brain Science Institute in Saitama, Japan, said in a statement.
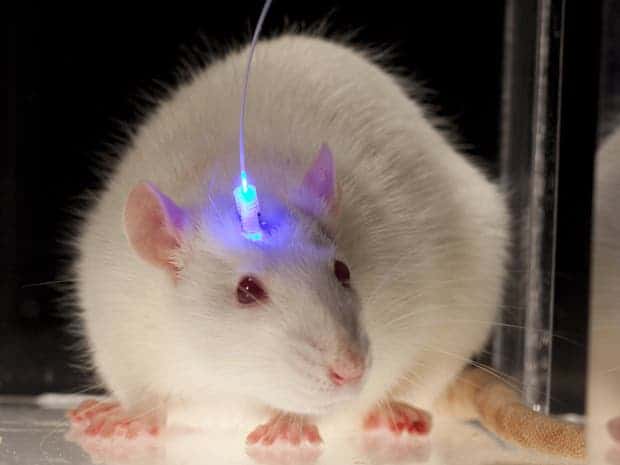
To pick the mice’s brains, the researchers used optogenetics – the combination of genetics and optics to control well-defined events within specific cells of living tissue. By way of an engineered virus, the researchers introduced a specific protein in those neurons that are typically activated when memories are made and stored; such a collection of neurons is called an engram. Since these proteins are sensitive to blue light, the researchers could control activity in the neurons, effectively turning them on or off at will.
The mice where separated into two groups. Electric shocks were applied in a distinct setting to induce a fear factor or bad memory. After a while, after the mice were introduced in the same room they became scared without any electric shock, signaling they were reliving the traumatic event. Then, some of the mice were injected with a drug called anisomycin which affects memory much in the same way as retrograde amnesia. When the drugged mice were placed in the same room, they showed no sign of fear or past memory of the same enclosure. However, once blue lights were shone on their brains, the mice instantly recalled their past memory, the researchers reported in Science.
Later on, brain scams performed by the team showed that the engrams in one part of the hippocampus – primarily associated with memory and spatial navigation – were communicating with cells in another part of the hippocampus. This network was extended to include connections with other regions of the brains, including the amygdala which is where the fear response is activated. So, because other connections in the mouse’s brain – those that were not affected by the drug – contained information about the electric shock, these were re-activated once the blue light was shone.
“If you test memory recall with natural recall triggers in an anisomycin-treated animal, it will be amnesiac, you cannot induce memory recall. But if you go directly to the putative engram-bearing cells and activate them with light, you can restore the memory,” Tonegawa said.
“Our conclusion is that in retrograde amnesia, past memories may not be erased, but could simply be lost and inaccessible for recall,” he went on. “These findings provide striking insight into the fleeting nature of memories, and will stimulate future research on the biology of memory and its clinical restoration.”
While there’s much promise and insight, the same procedure is impossible for amnesic human patients, due to both technical and ethical challenges. For one, the memory that needs to be activated needs to be studied and patterned before using a brain scan. Then, you need some specific proteins injected and a blue laser fitted inside your skull. On the other hand, this opens terrain for biomedical specialists and other neuroscientists to find pathways and drugs that might declutter these connections. In those cases where memory loss is merely a matter of neuron connectivity, there’s hope these can be activated once more.
Was this helpful?



