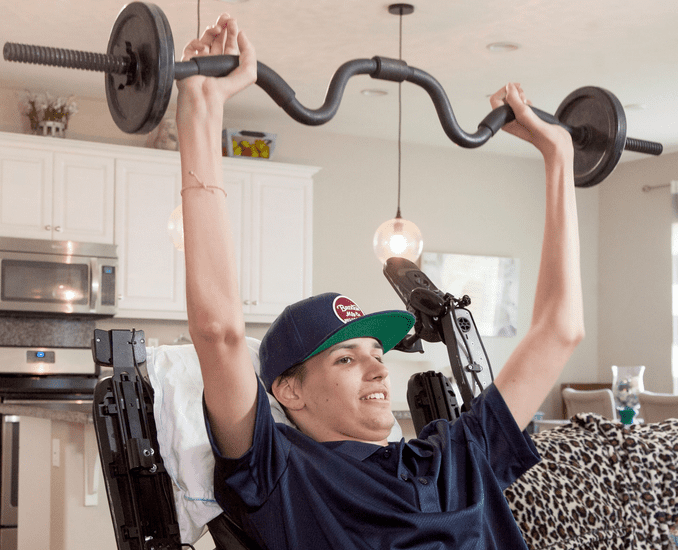
Six months ago, Kristopher (Kris) Boesen slammed into a telephone pole with his car after the vehicle fishtailed on the wet road. The traumatic injuries Kris sustained in the crash left him paralyzed from the neck down and doctors told the man’s parents there was a high risk he would remain so permanently.
“I couldn’t drink, couldn’t feed myself, couldn’t text or pretty much do anything, I was basically just existing. I wasn’t living my life, I was existing,” Kris said as he recounted the bleak days following his traumatic injury.
Faced with this prospect, Kris agreed to take part in an experimental neuroregenerative procedure developed by scientists at the USC Neurorestoration Center and Keck Medicine of USC. The 21-year-old had a novel treatment injected into the damaged cervical spine consisting of escalating doses of AST-OPC1 cells.
AST-OPC1 cells are made from embryonic stem cells which are coaxed to morph into oligodendrocyte progenitor cells (OPCs) — the cells found in the brain and spinal cord that support and replenish functioning nerve cells. Previous studies carried in a lab setting showed that AST-OPC1 stimulates vascularization and induces regeneration of denuded axons. This promotes the survival, regrowth, and conduction of nerve impulses in the injury site, the researchers say.
Only two weeks after his surgery, Kris began to show signs of improvement. Now three months after the procedure, he can now use a cell phone, operate a motorized wheelchair by himself, or hug friends and family. He can feel both arms and hands, something that lends hope that he can at least live independently.
“Now I have grip strength and do things like open a bottle of soda and feed myself. Whereas before I was relying on my parents, now after the stem cell therapy I am able to live my life.”

Kris is one of three patients who was enrolled in the clinical trial run by Asterias Biotherapeutics. Each patient was injected with two million cells into their necks, but Kris was the first patient to receive more than ten million stem cells in April.
“Typically, spinal cord injury patients undergo surgery that stabilizes the spine but generally does very little to restore motor or sensory function,” explains Charles Liu, MD, PhD, director of the USC Neurorestoration Center. “With this study, we are testing a procedure that may improve neurological function, which could mean the difference between being permanently paralyzed and being able to use one’s arms and hands. Restoring that level of function could significantly improve the daily lives of patients with severe spinal injuries.”
The surgery improved motor function up to two spinal cord levels, which for Kris now means he can brush his teeth without assistance or operate a computer. Things he wasn’t able to do on his own prior treatment.
Researchers are don’t want to jump to any conclusions, though. It’s not unheard of for some people with the same kind of injury as Kris to make a partial recovery. It’s impossible to say at this time if the marked improvement is due to the stem cell therapy, but we’ll know for sure once more patients enroll in the trial. Future versions of the clinical trial might also tell us if this procedure can be used to regain leg function as well — maybe by injecting more stem cells and in another location along the injured spinal chord. Most importantly, these trials are meant to assess the safety of such procedure.
Besides stem cells, researchers working to help the paralyzed regain bodily functions are experimenting with virtual reality training, flexible spinal chord implants, spinal chord zapping with electricity, and brain-computer interfaces.
Was this helpful?



