In a feat that surprised even the scientists who made the experiment, mice disabled by a condition similar to multiple sclerosis (MS) began to walk and even run again after human stem cells had been transplanted. The findings could potentially offer new means of treating MS, a terribly disease which plagues some 2.3 million people worldwide.
Growing stem cells and new legs
University of Utah researchers first transplanted human stem cells with no particular beneficial expectations. The scientists thought the stem cells would be rejected in the first place, like most foreign cells by the host’s immune system, however something much more than this happened. The plagued mice began to walk again within a short period, 10 to 14 days, following the transplant.
“My postdoctoral fellow Dr. Lu Chen came to me and said, ‘The mice are walking.’ I didn’t believe her,” said co-senior author, Tom Lane, Ph.D., a professor of pathology at the University of Utah, who began the study with co-first author Chen at the University of California, Irvine.
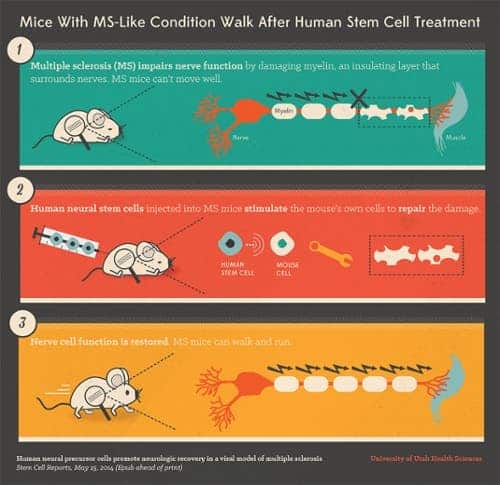
Multiple sclerosis (MS) is a potentially debilitating disease in which your body’s immune system eats away at the protective sheath (myelin) that covers your nerves. Damage to myelin causes interference in the communication between your brain, spinal cord and other areas of your body. This condition may result in deterioration of the nerves themselves, a process that’s not reversible.
Current treatments and drugs only concentrate on halting any of disease’s progress or ameliorating symptoms; once MS is in a later stage, it can not be reversed and there is no cure. Results from the study demonstrate the mice experience at least a partial reversal of symptoms. Immune attacks are blunted, and the damaged myelin is repaired, explaining their dramatic recovery.
“The way we made the neural stem cells turns out to be important,” said Loring, describing the reason behind the novel outcome.
The human neural stem cells send chemical signals that instruct the mouse’s own cells to repair the damage caused by MS. Experiments by Lane’s team suggest that TGF-beta proteins comprise one type of signal, but there are likely others. This realization has important implications for translating the work to clinical trials in the future.
“Rather than having to engraft stem cells into a patient, which can be challenging from a medical standpoint, we might be able to develop a drug that can be used to deliver the therapy much more easily,” said Lane.
Next, the researchers need to assess the long term effects of the human stem cell transplanted mice.
“We want to try to move as quickly and carefully as possible,” Lane continued. “I would love to see something that could promote repair and ease the burden that patients with MS have.”
Findings appeared in the journal Stem Cell Reports.






