A new report published by the leading health journal The Lancet focuses on hospitalization and death rates faced by countries as the COVID-19 crisis continues to unfold.
The study takes estimates from mainland China of the proportion of people infected by the COVID-19 virus who required hospitalization, and the latest death rate estimates from across the globe.
Analysis of both sets of data results in a stark message for the elderly, with both showing a sharp increase corresponding to advancing age. The overall death rates for individual age groups range from 0.0016% for 0–9-year-olds to 7.8% for people aged 80 and above.
Whilst hospitalisation rates vary from 0.4% of those aged 10 to 19, 3.4% for those in their thirties to 11.8% for those in their 60s and 18.4% for those aged 80 and above.
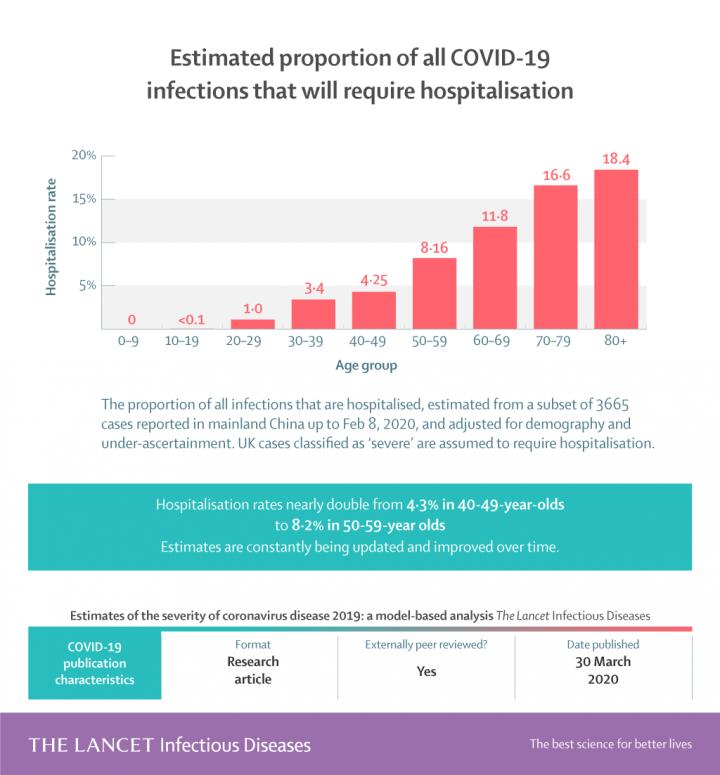
The report’s authors also have a stark warning for countries currently fighting the pandemic, without urgent intervention even the most advanced healthcare systems worldwide are likely to be overwhelmed by the number of people requiring treatment. They temper this by saying that this outlook could change as the pandemic continues.
“Our estimates can be applied to any country to inform decisions around the best containment policies for COVID-19,” says Professor Azra Ghani from Imperial College London, UK. “There might be outlying cases that get a lot of media attention, but our analysis very clearly shows that at aged 50 and over, hospitalisation is much more likely than in those under 50, and a greater proportion of cases are likely to be fatal.”
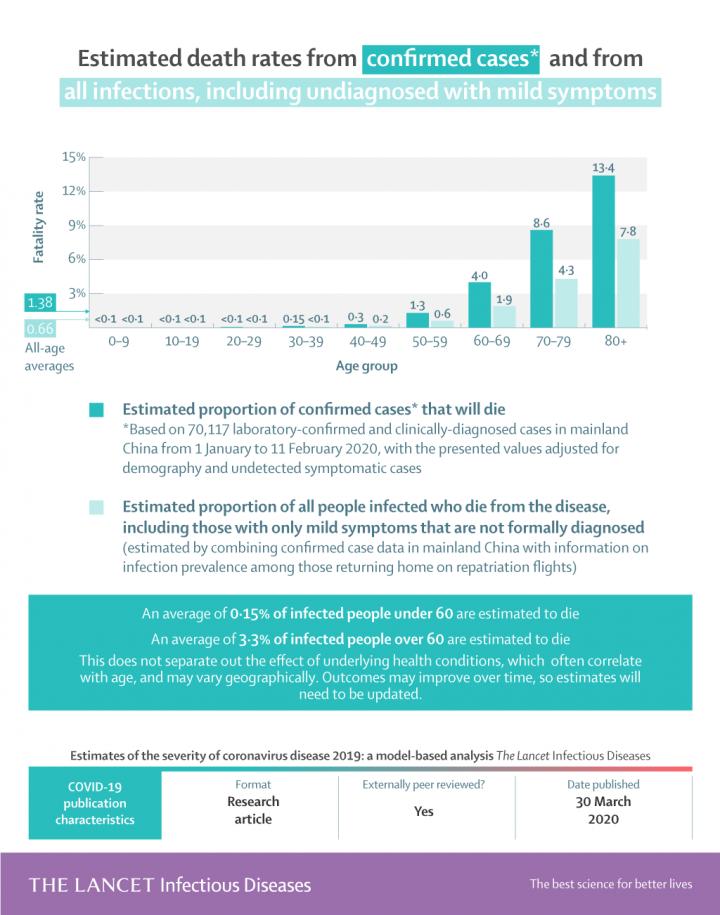
These are estimated death rates by age. (The Lancet Infectious Diseases)
Researchers estimated the COVID-19 death rate at 0.66% (when factoring unconfirmed cases)
Other key findings from the study include a slightly reduced overall death rate, with the rate of deaths from confirmed COVID-19 cases estimated at 1.38%. This rate is lowered to 0.66% when estimated unconfirmed cases are factored in. This rate is likely to vary in countries with higher populations of the elderly.
Whilst these estimates are lower than previous figures they still dwarf the rates for previous pandemics such as the H1N1 pandemic of 2009, which was found to be fatal in only 0.02% of confirmed cases.
“This study provides critical estimates on the proportion of people requiring hospitalisation which, when applied to the UK population, enabled us to get a handle on how many people might need to access NHS services,” says Professor Neil Ferguson from Imperial College London, UK. “As the UK epidemic unfolds, more data are becoming available, and at the moment the proportion of people in each age group most likely to require hospitalisation, and most likely to die from infection, are consistent with the estimates in this study.”
The study predicts that as 50–80% of the world’s population can be expected to be infected with COVID-19, it is unlikely that any healthcare systems are equipped to cope.
The study’s results vary from those previously conducted because it is the first to estimate the proportion of infections that will require hospitalisation and to adjust for the fact that only people with more severe symptoms are likely to be tested. This has resulted in a reduction from the estimated death rates in confirmed cases which has ranged from 2–8%, and a reduction in the overall death rate which had been estimated to be between 0.2–1.6%. Though these reductions are unlikely to carry with them much relief.
To conduct their research, the international team considered 3,665 cases from mainland China to estimate the proportion of cases likely to be severe enough to require hospitalisation. To estimate the average time between a person displaying symptoms and dying, 24 deaths in Hubei Province were examined.
The time between the first symptoms of COVID-19 to death is 17.8 days
They estimated that the time between the first symptoms and death is 17.8 days. They add that as this data was derived from early cases the time-lag may now be longer.
The average recovery time was estimated using data from 2,010 international cases — in which 169 people recovered. They found the time span from first symptoms to recovery was longer than that between early symptoms and death at 22.6 days.
Death rates from confirmed cases were estimated using data on 44,672 cases in mainland China. So they could estimate death rates relevant to the wider population, the team took data from 689 people repatriated from Wuhan to other countries and from the 3,711 people quarantined onboard the cruise liner Diamond Princess.
In all of their estimates, the team considered all individuals as being equally likely to be infected with COVID-19 — even across the age ranges considered. This is standard practice in studies that examine respiratory conditions.
The study concludes that most people infected with COVID-19 will recover, even those with severe symptoms, but they add that their study was unable to account for people with underlying medical conditions. This is something that will only be possible when individual cases can be added to the data. Likewise, they were unable to ascertain the disparity in death and hospitalisation rates between richer and poorer areas.
“Estimates of case fatality ratios might vary slightly from country to country because of differences in prevention, control, and mitigation policies implemented, and because the case fatality ratio is substantially affected by the preparedness and availability of health care,” says Dr Shigui Ruan, from the University of Miami, USA, who was not involved in the study. “Early studies have shown that delaying the detection of infected cases not only increases the probability of spreading the virus to others — most likely family members, colleagues, and friends — but also makes the infection worse in some cases, thereby increasing the case fatality ratio.”






