The Nanoflare technology uses a genetic-based approach to detect and image live cancer cells present in the blood stream, well before these had a chance to develop into a tumor. The gene-hunting particles developed at Northwestern University might help doctors develop personalized treatments for their patients and curb cancer spread, according to the paper published in PNAS.
Hunting cancer’s genes
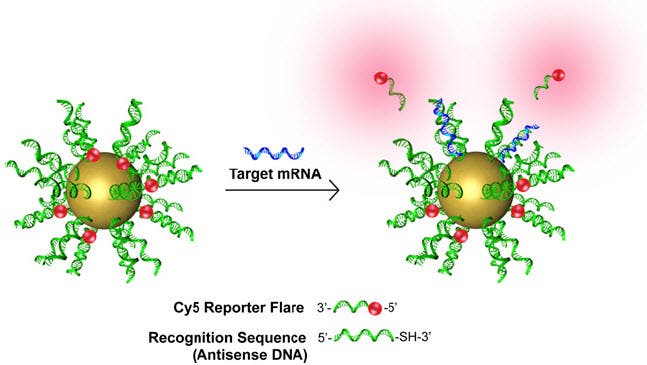
We’ve heard about nanoparticles that bind to cancer cells and mark these for detection, but Nanoflare works fundamentally different. Each Nanoflare is a tiny spherical nucleic acid with a gold nanoparticle core outfitted with single-stranded DNA “flares”. While conventional cancer nanoparticles bind to particles on the cancer cell’s surface, the new approach tracks tumor cells by recognizing a specific genetic code. But first the core nanoparticle, only 13 nanometers across, enters the cell, healthy or not. Once inside, if the specific genetic code is found inside, the Nanoflare binds to the target and lights up – it releases a powerful florescent signal. Easily visible, the researchers can then isolate the cells in question, culture them and apply various treatments to see which one works best. Once the doctors know which is the key treatment, they then serve it to the patient. Nanoflare was specifically designed for breast cancer, but the authors note it could be applied for other forms as well.
“This technology has the potential to profoundly change the way breast cancer in particular and cancers in general are both studied and treated,” said Chad A. Mirkin, PhD, a noted nanomedicine expert and a corresponding author of the study.
“Cancers are very genetically diverse, and it’s important to know what cancer subtype a patient has,” Mirkin said. “Now you can think about collecting a patient’s cells and studying how those cells respond to different therapies. The way a patient responds to treatment depends on the genetic makeup of the cancer.”
What’s truly groundbreaking about Nanoflare is that it can detect cancer cells in the blood stream. When the technique was tested with four different NanoFlares, each with a different genetic target relevant to breast cancer metastasis, cancer cells were detected with less than 1 percent incidence of false-negative results.
“When it comes to detecting and treating cancer, the mantra is the earlier, the better,” Thaxton said. “This technology may enable us to better detect circulating cancer cells and provides another tool to add to the toolkit of cancer diagnosis.”
Via KurzweilAI
Was this helpful?



