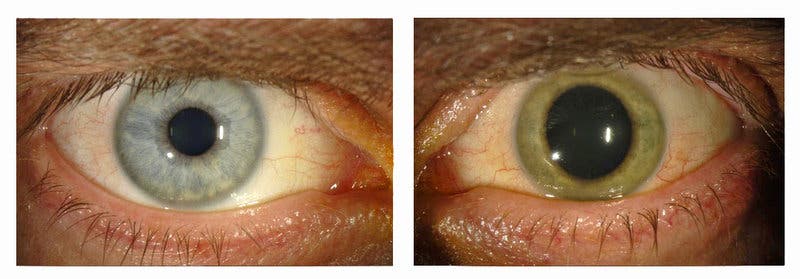
The current procedure for Ebola survivors is waiting 42 consecutive days for the tests to come back negative, then the patients can be discharged from quarantine. More and more evidence is surfacing, however, showing that the virus can still linger on through various nooks and crannies in the human body, undetected from standard testing. For instance, one man was treated for Ebola, but the virus was still present in his eyes. It wasn’t dormant either, since the inflammation caused his normally blue eyes to turn into green. Other evidence suggests Ebola can linger in the testes and be transmitted through sexual contact, but also in the uterus and joints. Only the case where Ebola was present in semen led to a transmission of the disease, so survivors aren’t necessary contagious. These serious findings do suggest more quarantine measures are required, though.
We still don’t know much about Ebola
Recently, the case of a British nurse who had contacted Ebola while working in West Africa has been making headlines. Pauline Cafferkey was treated for Ebola for one month at the Free Royal Hospital in London and later discharged after her condition improved and tests turned out negative. She returned to work as a public health nurse at Blantyre Health Centre in South Lanarkshire, but later fell ill again with Ebola symptoms and was yet again quarantined at the Free Royal as “critically ill”. The latest update (19/10/2015) from Free Royal suggests her condition has improved to “serious but stable”. UPDATE: The Scottish nurse was actually suffering form meningitis triggered by the virus, not a relapse.
Then, last week, a study published in the New England Journal of Medicine involving 93 men who had recovered from Ebola in Sierra Leone found the virus was still present in their semen. All men who were tested three months after recovery had Ebola in their semen, and 65% turned positive for those who were between four and six months past recovery, ZME Science reports. Doctors believe at least 20 Ebola cases have been the result of sexual transmission so far. One man still tested positive at nine and a half months.
“This new research shows that Ebola virus can persist in the semen and be transmitted sexually many months after the original infection has disappeared. The fact that there has so far been only one isolated [official] report of this type of infection suggests that this kind of transmission may be rare, but it highlights just how much we still don’t understand about the Ebola virus, infection and recovery,” Dr Jeremy Farrar, director of the Wellcome Trust told The Guardian.
“It also reminds us that the Ebola epidemic could be far from over. With more than 17,000 Ebola survivors, it’s possible that further cases of delayed transmission and late complications will occur.
“We must remain vigilant and continue to monitor the long-term health of survivors so that any new infections can be identified quickly and measures put in place to prevent further cases.”
Indeed, if Ebola is transmitted sexually even after the virus has been flushed out of the rest of the body (apart from the testes), then we should have seen more cases considering the number of surviving males. Is this a case of under reporting? Possibly. Liberia, a massive Ebola hotspot, has launched a testing program for surviving males, but Guinea has not. Clearly, Ebola has a lot more secrets than doctors bargained for.
A study which surveyed Ebola survivors from the 2014-2015 outbreak found 90 percent had chronic joint pain and 98 percent had poor appetites or an aversion to food. Some of these have been put on the emotional and physical strain that the disease had instated in the survivors, but it could be that these patients were still carrying the virus. Take the case of Dr. Ian Crozier, who worked in Sierra Leone and unfortunately contacted the virus. Though the rest of his body was Ebola free post treatment, his eyes were teeming with the virus which almost had him blind. Standard tests would have surely missed a positive detection. Another study reports how the Ebola lingered in the uterus of two pregnant women.
This begs the question: why won’t Ebola go away for good? Speaking to NPR, Ilhem Messaoudi, a viral immunologist and professor of biomedical sciences at the University of California, Riverside, says the immune system stays away from critical locations in the body like the “eyes, brain, placenta, fetus, testes, joint spaces and central nervous system,” where it could actually do more damage than good, mistaking healthy cells for the infectious kind. This makes them great places for viruses to hide, and Ebola isn’t alone. Other viruses like hepatitis B or herpes viruses do it too. But Messaoudi says this shouldn’t had been the case with Ebola, which has a tiny genome compared to other viruses that linger in off limits locations for the immune system. “Acute viruses like influenza, Ebola, yellow fever, West Nile [virus] — they infect, they replicate, and they’re cleared. That’s just how we’ve always thought of them. I’ve never heard of a yellow fever reservoir or a West Nile reservoir. Maybe they exist, and we just don’t know about it,” Messaoudi said.
Recognizing the need for more data, the U.S. National Institute of Allergy and Infectious Diseases and the Ministry of Health of Liberia launched a five-year program that will follow 1,500 survivors from the latest Ebola outbreak, along with 6,000 of their close contacts.
Was this helpful?



