In 2018, Swiss researchers Grégoire Courtine and Jocelyne Bloch made headlines with an implant they devised that sends electrical pulses to the spinal cord of paralyzed patients. The stimulation of the spinal nerves triggers plasticity in the cells, which seems to regenerate nerve connections, allowing test subjects paralyzed from the waist down to stand and walk, something that doctors told them they were unlikely to do again in their lifetimes. Now, the same team from the Swiss Federal Institute of Technology (EPFL) and Lausanne University Hospital have showcased an upgraded version of this spinal cord electrical stimulation — and the improvements speak for themselves.
The personalized spinal cord electrode implants were shown to restore motor movements within a few hours of the therapy’s onset in three paralyzed patients. The volunteers could not only stand and walk, but also perform motor movements that are an order of magnitude more complex, such as cycling, swimming, and canoeing.

Furthermore, the newly designed electrode paddle configuration can work with patients with more severe spinal cord injuries. For instance, the two 2018 patients who first tested the system retained some residual control over their legs following injury — too little for them to walk or even stand but just enough for the external electrical stimulation to allow them to regain motor function. In the upgraded version, the three patients who underwent spinal cord stimulation are completely paralyzed and were hence unable to voluntarily contract any of their leg muscles.
One of these patients is Michel Roccati, an Italian man who became completely paralyzed after a motorcycle accident four years prior to his enrollment in the EPFL spinal cord stimulation therapy. Bloch, a professor and neurosurgeon at Lausanne University Hospital, surgically implanted the new electrode lead in his spinal cord, and after recovery Roccati was ready to put the whole thing to the test.
During one particularly windy day in downtown Lausanne, the researchers and Roccati gathered outdoors with an array of hardware. The walker used by Roccati had been fitted with two small remote controls that connect wirelessly to a pacemaker in the patient’s abdomen, which in turn relays the signals to the spinal implants. The signal is converted into discontinued electrical pulses that stimulate specific neurons, allowing Roccati to move his lower limbs.
For the entire duration of the test, Roccati was in full control. The patient grasped the walker and pressed the remote control buttons when he intended to move. For instance, he would press the right side button when he intended to move his left leg. Pressing the buttons almost magically caused his legs to spring forward. He was walking — and getting better and stronger with each therapy session.
“The first few steps were incredible – a dream come true!” he says. “I’ve been through some pretty intense training in the past few months, and
I’ve set myself a series of goals. For instance, I can now go up and down stairs, and I hope to be able to walk one kilometer by this spring.”
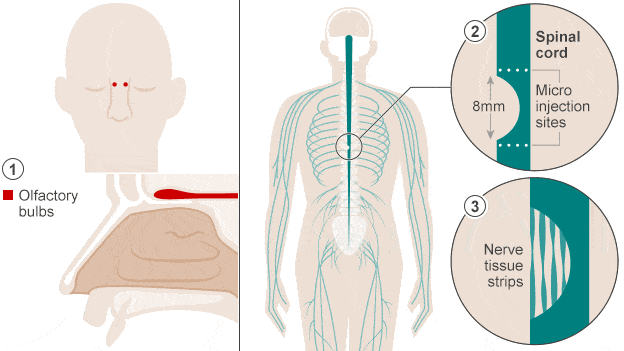
The updated system employs more sophisticated electrode paddle implants that target the dorsal roots in the lumbosacral region of the spinal cord controlled by artificial intelligence and the lowest nerve root in the spine responsible for trunk stability. These implants are controlled by an artificial intelligence system whose stimulation algorithms are supposed to imitate nature, activating the spinal cord like the brain would normally do to allow us to stand, walk, swim or ride a bike.
“Within a couple of hours, our therapy restored independent walking within a few hours after the onset of the therapy; in addition to many additional motor activities that are critical for rehabilitation and daily life,” said Robin Demesmaeker, a researcher at EPFL and the Department of Clinical Neurosciences, University Hospital Lausanne, told ZME Science.
“Central to this remarkably more effective and ultrafast therapeutic efficacy was a series of disruptive technological innovations driven by our understanding of the mechanisms through which electrical spinal cord stimulation restores movement after paralysis,” add Demesmaeker, who is also the first author of the new study that appeared today in the journal Nature Medicine.
The two other patients who’ve tested the new system also made dramatic improvements in their quality of life. In each case, the therapy — both the electrode placement on the spinal cord and the activities involved in the therapy — were personalized. After several months of intensive training, the three patients were able to regain muscle mass, move about more independently, and could take part in social activities they previously couldn’t possibly do like having a drink standing at a bar. Millions of other patients in similar conditions could stand to benefit from the same therapy.
“The main requirement is that the region of the spinal cord where the spinal implant is placed should still be intact and that the lesion should be higher,” Demesmaeker wrote in an email. “The major difficulties with more severe cervical injuries are owed to injury-induced blood-pressure instability that leads to severe orthostatic hypotension, making upright locomotor training impossible as well as highly impaired arm and hand function impeding the use of assistive devices such as crutches and a walker.”
The researchers in Switzerland are still in the middle of an ongoing clinical trial, in which they’re trying to find the most optimal path towards enabling brain-controlled spinal cord stimulation in real-time.
“We are also assessing the ability of spinal cord stimulation to alleviate other problems such as hemodynamic instability in patients with spinal cord injury and gait deficits in patients with Parkinson’s disease,” Demesmaeker said.