
As any diabetic patient is painfully aware, insulin can be incredibly expensive — and that’s particularly true for Americans. But why is a drug that was discovered a century ago so costly?
Insulin is the definite poster child of drug price gouging. If people wonder why ‘Big Pharma’ is so hated across the world, look no further than the ridiculous pricing for insulin and the dubious business practices of the handful of companies that manufacture it.
Over the past decade, the cost of insulin had tripled in the United States, and the out-of-pocket prescription costs that patients have to pay for the life-saving drug have doubled just in the last five years. But why is insulin so expensive in the US, and what can be done about it?
How much is a vial of insulin?
The cost of a single vial of insulin varies depending on the type of insulin and whether or not it is covered by insurance. Each insurance plan can cover insulin products differently.
In 2012, the average cost of insulin per diabetes patient was $2,864 per year. By 2022, this cost has jumped to nearly $12,000 per year for those who are uninsured and those with poor coverage.
Today, one vial of insulin can cost $250 and a pack of pens ranges from $375 to $500. Most patients require two to three vials of insulin per month or 1-2 packs of insulin pens, but some people need up to six vials per month.
For instance, Eli Lilly’s brand-name product, Humalog U-100, has a list price of $274.70 for a single 10 mL vial. But a study in 2018 published in BMJ Global Health found that the cost to make insulin ranged from around $2 to $6 for a 10mL vial.
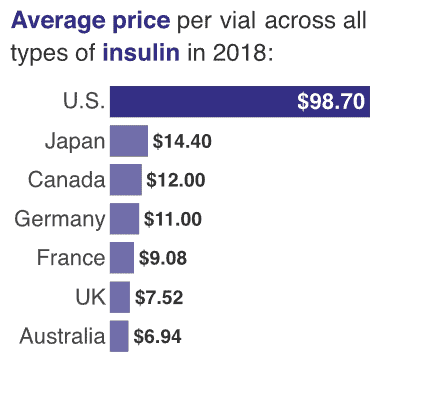
Overall, US list prices are five to 10 times higher than those of other countries. In 2018, the average price for a standard unit of all types of insulin in the US stood at $98.70, while the average price among all the other OECD countries was $8.81, according to the RAND Corporation.
Besides insulin, diabetic patients need other types of medication, which also tend to be high-priced. According to a 2016 study, the total average out-of-pocket pharmacy and medical costs for patients with diabetes reached $18,500 in 2016 — a surge of $6,000 from 2012 costs, half of which are accounted for by spending on insulin. Studies demonstrate that diabetes is the most expensive chronic disease in the United States, costing more than $327 billion in 2017.
As a result of these exorbitant prices, one in five patients say that they ration their insulin because they can’t afford full proper doses, according to a 2021 study published in the Annals of Internal Medicine. In some cases, this can cost lives. For patients with type 1 diabetes, just a single day without insulin is enough to send them to the emergency room.
There are nearly 30 million people suffering from diabetes in the United States, 5% of whom — or about 1.5 million — suffer from type 1 diabetes, hence they require insulin to literally survive. Although people with type 2 diabetes can control their blood sugar with diet and exercise, many still need insulin shots, especially as their condition deteriorates.
How much does a month of insulin cost in the United States?
Every patient’s needs are different, depending on the severity of their diabetes and individual factors such as weight. Assuming a patient needs 3 vials or 10 pens of insulin for a 30-day treatment, a monthly supply can cost:
| Drug Name | Average Price Per Package | Average Price Per Month |
| Novolog (insulin aspart) Novolog Flex Pen | $333.99/vial $123.99/pen | $1,001.97 $1,239.90 |
| Humalog (lispro) Humalog Kwikpen (lispro) | $316.22/vial $134.99/pen | $948.66 $1,349.90 |
| Lantus (insulin glargine) Lantus Solostar (pen) | $314.99/vial $101.73/pen | $944.97 $1,017.30 |
| Basaglar KwikPen (insulin glargine) | $88.21/pen | $882.10 |
| Humulin N (insulin isophane) | $122.67/pen | $1,226.70 |
| Novolin N (insulin isophane) | $166.99/vial | $500.97 |
| Levemir (detemir)Levemir Flextouch (pen) | $446.99/vial $112.98/pen | $1340.97 $1129.80 |
| Novolin R (insulin regular) | $161.00/vial | $483.00 |
| Toujeo Solostar (insulin glargine) | $115.18/pen | $1151.80 |
| Tresiba (insulin degludec)Tresiba Flextouch (pen) | $351.38/vial $123.18/pen | $1054.14 $1231.80 |
Why is insulin so darn expensive?
Diabetes was a death sentence until the early 20th century, as there was no treatment for the disease. That all changed in 1921 when a team of Canadian scientists discovered insulin, a hormone that regulates blood sugar levels.
The discovery of insulin was hailed as a miracle, and the scientists who made it became heroes. They sold the patent for insulin to the University of Toronto for the symbolic figure of $1, so that the drug would be widely available to everyone who needed it. Not long after, insulin from pigs and cattle was being produced and sold on a massive scale around the world.
“Insulin does not belong to me, it belongs to the world,” Frederick Banting, co-inventor of insulin, said at the time.
Fast forward to the present day, and the situation could not be more different. Insulin is now one of the most expensive drugs in the US, with prices skyrocketing in recent years.
Only three pharmaceutical giants — Novo Nordisk, Sanofi-Aventis, and Eli Lilly — produce and control 90% of the global insulin supply. Basically, these big three control the market. They also tend to mirror each other’s prices.
Usually, when a drug has been on the market for decades, its patent expires, which means any manufacturer can produce a generic version that should drive the prices down by a high margin. But this expectation falls apart in the case of insulin — if anything, the reverse is true.
Part of the reason for this is something called ‘evergreening’, the practice involving various techniques to extend the protection of a drug and block competition that might lead to price reductions. Oftentimes, this means simply making an incremental improvement to the insulin product, thereby resetting the patent’s length by decades.
Early insulin was not ideal, requiring multiple injections for some patients. Some even developed potentially dangerous allergic reactions. Over the decades, manufacturers have introduced all sorts of new processes and technologies that vastly improved insulin, making the drug purer and safer.
In the 1970s, manufacturers stopped making insulin from animals. Instead, everyone now uses a technique based on recombinant DNA technology that basically produces human insulin from genetically modified bacteria.
That was great news for animals, but kinda bad news for patients. Although there’s no clear reason why a company would stop producing the animal-version of insulin, this cheap, older alternative has disappeared from the market — at least in the U.S. You can still find animal-derived insulin in other countries, such as in Canada, where insulin can be almost ten times cheaper.
By making minor modifications to their manufacturing process or packaging, manufacturers were also able to extend patent protections, thereby discouraging competitors and promoting a cartel-like business environment. This strategy is a win-win for big business but a lose-lose for patients who require life-saving therapy because these patent extensions discourage generic drugs from being developed.
Unlike aspirin or Adderall, which are chemical drugs that contain the same ingredients every time, insulin is a biological drug. This means that manufacturing is a lot more complicated since you have to work with live cells. It also means that the rules for generic drug patents don’t apply. For instance, the generic equivalent of a biological drug is called a ‘biosimilar’.
In the US, there are only 17 FDA-approved biosimilars for insulin. Many of these biosimilars are manufactured by one of the ‘big three’ manufacturers, which doesn’t help to bring the price down. Biosimilars can cost up to $250 million to produce and take up to eight years to bring to the market, versus a one-year investment of as little as $1 million for conventional generics, Vox reports.
When asked how they explain the high price of insulin, manufacturers often cite the “complexity of the supply chain” as a reason high up their list. That may be true, but that doesn’t explain why cheaper, easy-to-manufacture animal-derived insulin isn’t offered as an alternative.
The role of healthcare insurance in insulin price gauging
Another factor contributing to the high cost of insulin is the way healthcare is structured in the US. Unlike other developed countries, the US does not have a universal healthcare system, which means that many people rely on health insurance to pay for their medical expenses.
However, health insurance companies often negotiate prices with pharmaceutical companies, and they may not cover the full cost of a drug if they deem it to be too expensive. This puts the burden of paying for insulin on the patient, who may not be able to afford it.
A 2022 study that appeared in the journal Health Affairs found that 14% of Americans who use insulin spend at least 40% of their disposable income on insulin, after paying for other essentials like food and housing. This figure does not include expenses on related diabetes care, such as glucose monitors, insulin pumps or other medications.
Is there a silver lining?
So, what can be done to address the high cost of insulin in the US? One solution is to reform the patent system to prevent pharmaceutical companies from holding monopolies on life-saving drugs. This would allow other companies to produce generic versions of insulin, which would increase competition and lower prices. However, this seems as unrealistic at this moment as implementing a universal healthcare system in the US.
But frustration over insulin price gauging has reached an all-time high, which explains why a handful of states, chief among them California, are planning to make their own insulin and put the drug on the market at a price equivalent to the cost of production. States buy a lot of drugs too, through their Medicaid programs and health plans for government workers, so they would also reap the rewards if those drugs are cheaper.
California has already passed a bill that will give it the legal authority to manufacture its own insulin and has set aside $100 million for this effort. At first, California would like to work with existing enterprises that could be interested in producing generic insulin for the state as a subcontractor. One such enterprise could be Mark Cuban’s Cost Plus drug company. Another important player is the nonprofit Civica RX, first launched in 2018 and aims to produce several cheap generic versions of essential medicine for hospitals in the US. In the long term, however, California wants to open its own manufacturing facilities, staffed by civil workers.
Other states are pushing for legislation that would lower out-of-pocket costs for patients in dire need of insulin. At least 22 states so far have passed bills that cap co-payments for insulin at $100 or less for a 30-day supply. However, these measures are only for people with health insurance.
The bottom line is that insulin is expensive because manufacturers control its price and since competition (or the competitive spirit) is almost non-existent. In other words, insulin is expensive because it can be in the U.S.
Was this helpful?



