
Picture this: a patch no larger than a band-aid, clinging to your skin, humming silently as it keeps a keen eye on your body’s internal vital signs. You’re not confined to a hospital bed or tethered to bulky machinery, but, instead, you’re free to roam, work, and play.
Sounds a bit like something out of a science fiction production, but this is very much in the realm of reality. Dubbed the ultrasound system-on-patch (USoP), this innovative medical monitoring device seeks to condense all the best features of the bulky ultrasound scanners that are typically found in hospital rooms into a very small, mobile package.
According to the engineers at the University of California San Diego behind the wearable device, the USoP is not just a sensor. It’s a complete, integrated system, designed to sense deep tissue vital signs wirelessly even when the patient is on the move.
This new wearable ultrasound technology is a unique solution to address many vital sign monitoring challenges in clinical practice,” Muyang Lin, a Ph.D. candidate in the Department of Nanoengineering at UC San Diego and the first author of the study, told ZME Science.
“By using wearable ultrasound technology, we untether the patient from bulky machines and automate the ultrasonic examination. Using a wearable patch, we can monitor deep tissue physiology on a mobile subject, which has never been achieved by any device before.”
Untangling the Tether
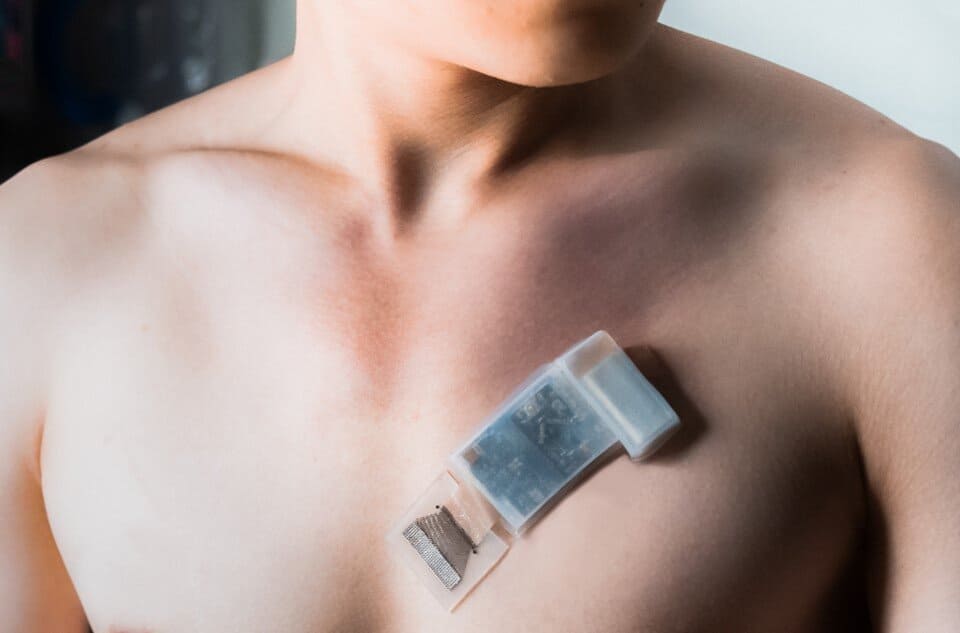
This device is designed to delve deep into your tissues, tracking physiological signals from as deep as 165 mm (6.5 inches) beneath the skin and continuously measuring central blood pressure, heart rate, cardiac output, among other vitals, for up to twelve hours at a time.
But how does it all work?
Traditional soft ultrasonic sensors, while revolutionary in their own right, had one big drawback. They were bound by cables, chaining the user to the spot and limiting their freedom of movement.
The UC San Diego team of researchers severed these chains by incorporating a small, flexible control circuit that communicates with an ultrasound transducer array to collect and transmit data wirelessly. And then, there’s the brain of the operation, the machine learning component, tasked with interpreting the data and keeping track of subjects in motion.
The Internet of Medical Things
Yet, the USoP isn’t just an upgrade; it’s an innovation that propels medical monitoring into the uncharted territory of the Internet of Medical Things (IoMT). Picture a network of medical devices, all connected to the internet, all wirelessly transmitting data into the cloud for analysis and professional diagnosis. The USoP is just one of these devices, which seem bound to become ever more present in the high-tech medical practice of the future.
And what could this mean for you?
Imagine a future where a patch, maybe not all that different from this iteration of the USoP, could monitor your vital signs as you go about your daily activities. It could evaluate your cardiovascular function in motion, detecting any abnormal values that could signal heart failure. Or, if you’re the picture of health, it could measure your cardiovascular responses to exercise in real-time, helping tailor a workout plan just for you.
But this project wasn’t always as ambitious. In fact, it started out as something much more simple.

According to Lin, the initial goal was quite modest: to build a wireless blood pressure sensor. As the team worked, however, they realized that this system could measure a much wider array of critical physiological parameters than blood pressure alone.
So, how does this miniaturized ultrasound patch differ from the full-fledged ultrasound device we’re accustomed to seeing in hospitals? Lin clarifies in an email: “Our ultrasound patch can perform general tissue imaging but cannot image blood flow.”
While it can’t do everything a hospital ultrasound machine can do just yet, it brings a unique feature to the table. This patch, unlike its larger counterparts, can quantitatively measure deep tissue physiological parameters from a moving subject, making it ideal for real-time, on-the-go monitoring.
“With our patch technology, people could wear it and measure their signals anywhere and anytime. We believe this enables many life-saving applications. For example, this patch can capture abnormal values of blood pressure and cardiac output at rest or during exercise, which are hallmarks of hypertensive crisis and heart failure,” said the researcher.
From Singular to Universal
One challenge the team faced was the transferability of their machine learning algorithm. The system initially proved ‘stubborn’, unable to correctly apply its learned lessons from one subject to another.
But a solution was found. An advanced adaptation algorithm now allows the machine intelligence to be transferred from subject to subject, making the model’s results both reliable and generalizable.
Now, the researchers are busy planning clinical trials with large sample sizes in order to test the device’s efficacy in a real-world setting.
“As we envision this device as the next generation of deep-tissue monitoring devices, clinical trials are our next step,” states Xiaoxiang Gao, a postdoctoral scholar in the Department of NanoEngineering at UC San Diego and co-first author of the study.
The ambitions for this technology don’t end at the lab doors. Dr. Sheng Xu, a professor of nanoengineering at UC San Diego Jacobs School of Engineering and a co-founder of Softsonics LLC, sees the potential for commercialization of this wearable ultrasound technology. Picture a world where your personal trainer, physiotherapist, or even yourself, could monitor your physiological parameters anywhere, anytime.
By making the invisible visible, this patch offers a new way to look inside ourselves, turning the mirror inward in order to enhance our health.
The findings appeared in the journal Nature Biotechnology.
Was this helpful?



