The bandage is perhaps one of the first and most basic medical tools humans have invented. For thousands of years, people have been using strips of cloth on wounds to stop bleeding and dress wounds — but that doesn’t mean that the way we make and use bandages hasn’t changed. In fact, it’s changed quite a lot.
The ancient Egyptians cleverly used honey as both an adhesive and a natural antibiotic. Hippocrates, the noted Greek physician whose name is directly tied to the Hippocratic Oath, was known to treat ulcers with wine and cover them with fig leaves. Fast forward to the 20th century, Johnson & Johnson employee Earle Dickson invented the now ubiquitous Band-Aid.
But what about the bandage of the 21st century? I think you already have an idea of what it looks like: strap a boatload of sensors and electronics, and now it’s a ‘smart’ bandage!
From rough linen to high-tech sensors

These high-tech bandages are typically designed to do one of two things: either gather data about the state of a wound or help heal the wound. But the smart bandage developed by a team led by Yuanwen Jiang, a chemical engineer at Stanford University, does both.
The battery-free, flexible device can monitor wounds in real-time, while also delivering treatment and significantly reducing scar tissue formation. For instance, it could be strapped to the site of chronic injuries, such as on the painful leg of a diabetic or on foot ulcers that can last for months. These sorts of chronic wounds that don’t heal can easily ruin a patient’s quality of life, causing anxiety and depression, as well as costing healthcare systems across the world more than $25 billion each year.
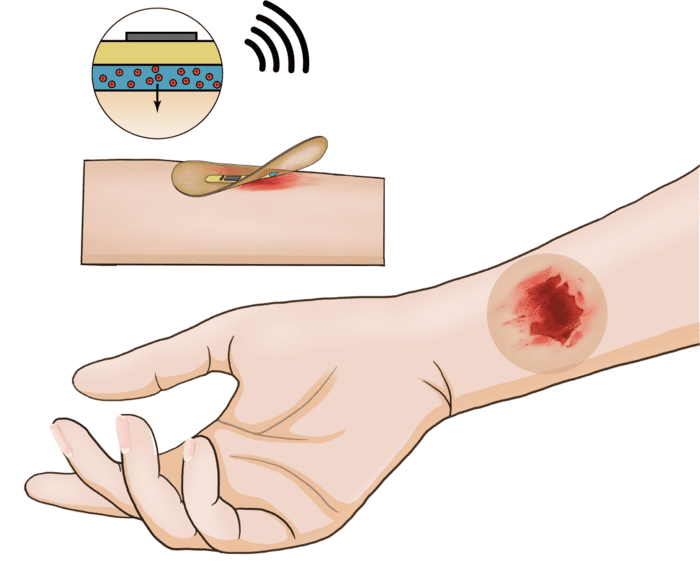
In order to monitor wound healing, the device uses impedance and temperature sensors that are embedded inside wireless circuitry. If the device senses that the wound is healing poorly or, worse, has become infected, the central processing unit will direct more electrical stimulation across the wound bend to accelerate tissue closure and reduce infection. If the electrical impedance increases and the local temperature declines that means inflammation is subsiding and the wound is actually healing. All the data from the sensors can be tracked wirelessly in real-time using a smartphone app.
Remarkably, all the electronics, including the sensors, radio antenna, microcontroller unit, memory, and all the other components, fit inside a single, flexible electrical layer that is only 100 microns thick. That’s about as thick as a single coat of latex paint.
Smart materials, smart sensing
On top of the active electrical layer lies a custom-made hydrogel, which is a skin-like polymer that delivers healing electrical stimulation and facilitates data collection from the sensors. The hydrogel is engineered to have an adhesive surface that is tight enough to securely attach itself to the wound surface, but loose enough so that the patient or doctor may cleanly and gently pull away the bandage without harming the wound when warmed to only 40°C (104°F).
“In sealing the wound, the smart bandage protects as it heals,” says Yuanwen Jiang, co-first author of the study and a postdoc at the Stanford School of Engineering. “But it is not a passive tool. It is an active healing device that could transform the standard of care in the treatment of chronic wounds.”
To speed up the healing process, the bandage electrically stimulates the site of the wound. Previous research found that electrical stimulation limits bacterial infection, prevents the development of biofilms, helps with tissue repair, and proactively promotes new tissue growth. While they were testing their electronic bandage, the Stanford researchers also found evidence that electrical stimulation seems to promote the expression of certain pro-regenerative genes, such as Selenop (an anti-inflammatory gene) and Apoe (a gene that promotes muscle growth and repair).
That’s not all. Electrical stimulation also increases the production of white blood cells, particularly monocytes and macrophages — immune cells play a key role in closing wounds and proliferating the active phase of wound healing.
For now, this particular iteration is only a proof of concept. The researchers need to figure out how to reduce costs and solve some long-term data storage issues, and they’re also looking at ways to improve it. For instance, new sensors could be added that measure other important indicators, such as metabolites, biomarkers, and acidity.
But the technology could be coming sooner rather than later. Coupled with a machine learning algorithm, all of this massive stream of data could be turned into actionable diagnostics that are more accurate and quicker.
Conventional bandages will still have their time and place. After all, why ruin a classic if it’s not broken? But it’s great to see bandage technology reach the next level.
The findings were reported in the journal Nature Biotechnology.
Was this helpful?



